| Title |
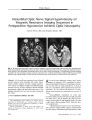
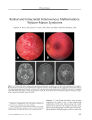
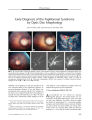
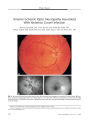
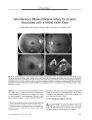
Anterior Ischemic Optic Neuropathy Associated with Rickettsia Conorii Infection |
| Creator |
Khairallah, M; Zaouali, S; Ben Yahia, S; Ladjimi, A; Messaoud, R; Jenzeri, S; Attia, S |
| Affiliation |
Department of Ophthalmology, Fattouma Bourguiba University Hospital, Monastir, Tunisia. moncef.khairallah@rns.tn |
| Abstract |
A 43-year-old man with fever, headache, and skin rash developed unilateral acute anterior ischemic optic neuropathy. The indirect immunofluorescence test was positive for Rickettsia conorii. Although retinal lesions have been described in Rickettsia conorii infection, this is the first reported case of ischemic optic neuropathy. This infection should be considered in a patient with nonarteritic anterior ischemic optic neuropathy with high fever or skin rash who inhabits or travels from an endemic area. |
| Subject |
Acute Disease; Adult; Anti-Bacterial Agents, therapeutic use; Boutonneuse Fever, diagnosis; Boutonneuse Fever, drug therapy; Boutonneuse Fever, microbiology; Doxycycline, therapeutic use; Eye Infections, Bacterial, diagnosis; Eye Infections, Bacterial, drug therapy; Eye Infections, Bacterial, microbiology; Fluorescein Angiography; Fluorescent Antibody Technique, Indirect; Humans; Male; Optic Neuropathy, Ischemic, diagnosis; Optic Neuropathy, Ischemic, drug therapy; Optic Neuropathy, Ischemic, microbiology; Perimetry; Rickettsia conorii, isolation & purification; Visual Fields |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225440 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s69058t8/225440 |