| OCR Text |
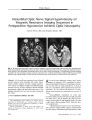
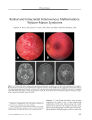
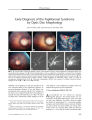
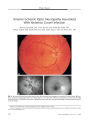
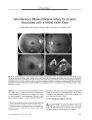
Show ORIGINAL CONTRIBUTION Presumed Pituitary Abscess Without Infectious Source Treated Successfully With Antibiotics Alone Apjit Kaur, MS, Ajai Agrawal, MS, and Manish Mittal, MD Abstract: A 12- year- old girl developed acute frontal headache and severe visual loss in both eyes. A presumptive diagnosis of pituitary abscess was made on the basis of suggestive magnetic resonance imaging findings. These consisted of a large non- enhancing area within the pituitary gland and thin irregular glandular rim enhancement. There was no evidence of pre- existing intracranial or systemic infection. The patient recovered completely after treatment with intravenous and oral antibiotics without surgical drainage. This case highlights the need for a high index of suspicion for pituitary abscess based on unusual imaging findings even when there is no source of infection. ( J Neuro- Ophthalmol 2005; 25: 185- 188) Pituitary abscess is a rare and potentially life- threatening intrasellar infection ( 1- 12). The infection may arise within the gland or from a nearby or remote source. Preexisting sellar lesions need not be present. We report a case of pituitary abscess in a child that was diagnosed on the basis of magnetic resonance imaging ( MRI) with no identified source of infection (" primary pituitary abscess"). The patient responded to intensive parenteral antibiotic therapy alone. No surgical drainage was required. CASE REPORT A 12- year- old girl presented with rapid onset diminution of vision in both eyes associated with a severe frontal headache. The patient had no history of diplopia or evidence of infection. Visual acuity was light perception OD and finger counting OS. Neither pupil reacted normally to direct light. Department of Ophthalmology ( AK, AA), King George's Medical University, Lucknow, India. Life Speciality Diagnostics ( MM), Lucknow, India. Address correspondence to Dr. Ajai Agrawal, Sri Laxman Bhawan, 20/ 2, Indira Nagar, Lucknow- 226016, India. E- mail: ajaiagrawal@ rediffmail. com apjit@ rediffinail. com. Phone : 0091- 522- 2341586 Ophthalmoscopy showed mild temporal disc pallor OD and no abnormalities OS. The remainder of the ophthalmic, neurologic, and systemic examinations was normal. Computed tomography ( CT) showed irregular lytic areas involving the basisphenoid bone ( Fig. 1) with a hypodense, peripherally enhancing pituitary mass. MRI revealed an enlarged sella and a bulging pituitary gland with a convex superior margin ( Fig. 2). Effacement of both cavernous sinuses was seen without encasement of the internal carotid arteries. The lesion appeared mildly hypointense on Ti- weighted images and heterogeneously hyperintense on T2- weighted images. There was edema and compression over distal parts of both optic nerves and chiasm. There was a focal breech in the sellar floor with extension of the lesion into the left part of the sphenoid sinus ( Fig. 2). Post contrast images showed a large necrotic area of relative non-enhancement lined with thin irregular rim enhancement. Mild meningeal enhancement of the left optic nerve sheath and the base of cavernous sinus was noted. Laboratory tests revealed a leukocytosis ( 14,000/ mm3) with no other abnormalities. The endocrinological profile was unremarkable. FIG. 1. Pre- treatment coronal CT scan with bone windows shows areas of bone destruction and trabecular loss in the sellar floor ( arrows). J Neuro- Ophthalmol, Vol. 25, No. 3, 2005 185 J Neuro- Ophthalmol, Vol. 25, No. 3, 2005 Kaur et al FIG. 2. Pre- treatment MRIs. A. Sagittal T1 - weighted scan shows a depressed sellar floor and chiasmal compression ( arrow). B. Coronal unenhanced T1 - weighted scan shows an enlarged pituitary gland. C. Coronal enhanced T1 - weighted scan shows a large internal necrotic area ( thin arrow). The suprasellar component is compressing the optic chiasm and there is focal erosion of the sellar floor on the left ( thick arrow). D. Coronal T2- weighted scan shows a hyperintense necrotic area ( arrow) and direct extension of the lesion into the left cavernous sinus. E. Sagittal T1 - weighted enhanced scan shows a large necrotic area of relative non enhancement in the pituitary gland ( arrow) with thin, irregular rim enhancement. Given these imaging features, a pituitary abscess was suspected. The patient was treated with intravenous antibiotics ( cefazoline 1 g q 8h, amikacin 250 mg q 12 hours and chloramphenicol 400 mg q 6 h) for four weeks and an oral antibiotic ( cefadroxil 500 mg q 12 h) for one month after discharge. The patient responded to therapy with steady recovery in visual acuity, color vision, and visual fields. Follow- up contrast- enhanced MRI scan two months after the initial scan revealed moderate reduction in size of the pituitary gland with reduced mass effect over the optic chiasm and third ventricle. The pituitary gland homogenously enhanced but there was no longer any glandular rim, meningeal, or infrasellar enhancement ( Fig. 3). After four weeks of therapy, the patient's visual acuity had improved to 20/ 30 OU with normal color vision and visual fields. The patient is currently well after a one- year follow- up. Imaging has not been repeated. DISCUSSION Pituitary abscess implies involvement of the pituitary gland by an infectious process ( 1). Since the first description by Simmonds in 1914 ( 2), only 123 cases have been reported ( 3,4,5). Scanarini et al. ( 6) encountered only two such cases in 500 expansive pituitary lesions ( 0.4%) over a period of almost three decades. Jain et al. ( 7) described six cases of pituitary abscess that constituted 0.6% of all pituitary lesions operated by them over a 10- year period. In a series of 503 transsphenoidal approaches to sellar lesions, Hanel et al. ( 4) found only one case of pituitary abscess ( 0.2%). 186 © 2005 Lippincott Williams & Wilkins Presumed Pituitary Abscess J Neuro- Ophthalmol, Vol. 25, No. 3, 2005 FIG. 3. Post- treatment MRIs. Sagittal ( A) and coronal ( B) enhanced T1- weighted scans show moderate reduction in the size of the pituitary gland with a small necrotic area ( arrow, B). There is extension of the mass into the left cavernous sinus with narrowing of the internal carotid artery. There appears to be no specific gender predilection for pituitary abscess. In a series of 24 cases described by Vates et al ( 3), 9 were women and 15 were men. However, a strong female preponderance was described in the series of Domingue and Wilson ( 8). Pituitary abscesses occur in three settings ( 9). The first setting is a pre- existing pituitary adenoma, craniopharyngioma or Rathke's cleft cyst ( 6,8,10). Tumors appear to be vulnerable to infection due to impaired circulation or areas of necrosis ( 11). The second setting is direct extension or hematogenous spread from sphenoid sinusitis, meningitis, cavernous sinus thrombophlebitis, or contaminated cerebrospinal fluid leakage ( 1,12). The present case falls into the third setting, in which abscess occurs in a previously healthy gland with no identified source of infection. The clinical features of pituitary abscess are not specific to that diagnosis. Patients often present with headache along with visual acuity and field losses due to mass effect of the pituitary abscess. Domingue and Wilson ( 8) found that visual field defects were present in 16 of 29 pituitary abscess cases in whom visual field studies were performed. Vates et al. ( 3) reported non- specific headache without visual symptoms as the most common presenting complaint. Endocrine disturbances including amenorrhea, polyuria, polydipsia and sensitivity to cold have been occasionally encountered. Unusual presentations of pituitary abscess include aseptic meningitis ( 13) and pituitary apoplexy ( 14). Pituitary abscess cannot easily be differentiated by imaging from a solid pituitary mass lesion. MRI features of pituitary abscess were first described in 1989 by Dickob et al ( 15) and later reviewed extensively by Wolansky et al ( 16). Like pituitary adenomas, most pituitary abscesses show high signal on T2- weighted images and signal intensity similar to that of surrounding brain on Tl- weighted images ( 15,16). Contrast- enhanced MRI has been the most useful method of differentiating pituitary abscess by showing peripheral rim enhancement. Loss of the normal posterior pituitary lobe bright signal on Tl- weighted MRI is more common in abscess than in adenoma. Notably, diabetes insipidus is present in only 10% of adenomas but occurs in almost half of patients with abscesses ( 17). Despite the use of CT and MRI, the preoperative diagnosis of pituitary abscess remains difficult. Most patients are suspected of having atypical pituitary adenomas and have undergone surgical drainage by the transsphenoidal approach followed by antibiotic therapy once the abscess is identified from the surgical specimen ( 3,8). Complete resolution of a pituitary abscess by antibiotic therapy alone ( without need for surgical drainage) is rare. A Medline search revealed only one case of pituitary abscess treated by medication alone ( 18). This case highlights the need for a high index of suspicion for pituitary abscess based on unusual imaging findings even when there is no indication of a pre- existing sellar mass or a pre- existing intracranial or systemic infection. Early diagnosis may allow the use of aggressive antibiotic treatment without the need for surgical intervention. In any case, the institution of prompt therapy is vital in dealing with this potentially life- threatening condition. REFERENCES Boggan JE. Pituitary abscess. In Wilkins RH, Rengachary SS, eds. Neurosurgery 2nd edition. New York: McGraw- Hill; 1996: 3321- 3322. Simmonds M. Zur Pathologie der Ag hypophysis. Verh Dtsch Pathol 1914; 17: 208- 12. Vates GE, Berger MS, Wilson CB. Diagnosis and management of pituitary abscess: a review of twenty four cases. J Neurosurg 2001; 95: 233^ 1. Hanel RA, Koerbel A, Prevedello DM, et al. Primary pituitary abscess: case report. Arq Neuropsiquiatr 2002; 60( 3- B): 861- 5. ShimamuraN, Ogane K, Takahashi T, et al. Pituitary abscess showing high uptake of thallium- 201 on single photon emission computed tomograph - case report. Neurol Med Chir ( Tokyo) 2003; 43( 2): 100- 3. 187 J Neuro- Ophthalmol, Vol. 25, No. 3, 2005 Kaur et al 6. Scanarini M, Cervellini P, Rigobello L, et al. Pituitary abscesses: report of two cases and review of literature. Acta Neurochir 1980; 51: 209- 17. 7. Jain KC, Varma A, Mahapatra AK. Pituitary abscess : a series of six cases. Br J Neurosurg 1997; 11: 139- 43. 8. Domingue JN, Wilson CB. Pituitary abscesses : report of seven cases and review of the literature. J Neurosurg 1977; 46: 601- 8. 9. Fong TC, Johns RD, Long M, et al. CT of pituitary abscess AJR 1985; 144: 1141- 2. 10. Selosse P, Mahler C, Klaes RL. Pituitary abscess: case report. J Neurosurg 1980; 53: 851- 2. 11. Askenasy HM, Israeli J, Karny H, et al. Intrasellar abscess simulating pituitary adenoma. Neurochirurgica 1971; 14: 34- 7. 12. Verdalle P, Roquet E, Hor F, et al. Pituitary abscess. A rare complication of sinusitis. RevLaryngol OtolRhinol ( Bord) 1997; 118: 327- 9. 13. Rudwan MA. Pituitary abscess. Neuroradiology 1977; 12( 5): 243- 8. 14. Kingdon CC, Sidhu PS, Cohen J. Pituitary apoplexy secondary to an underlying abscess. J Infect 1996; 33: 53- 5. 15. Dickob M, Scharphuis T, Distelmaier P, et al. Die Diagnostik des Hypophysen- abszesses mittels MRI und hochanflosender CT. Neurochirurgia 1989; 32: 184- 6. 16. Wolansky LJ, Gallagher JD, Heary RF, et al. MRI of pituitary abscess: two cases and review of literature. Neuroradiology 1997; 39: 499- 503. 17. Enzmann DR, Sieling RJ. CT of pituitary abscess. AMR 1983; 4: 79- 80. 18. Dechambenoit G, Datie A, Grumitzky EK et al. [ Pituitary abscess treated by medication]. Rev Neurol ( Paris) 1993; 149( 10): 567- 71. 188 © 2005 Lippincott Williams & Wilkins |