| Title |
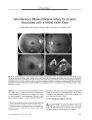
Retinal and Intracranial Arteriovenous Malformations |
| Creator |
Reck, SD; Zacks, DN; Eibschitz-Tsimhoni, M |
| Affiliation |
Department of Ophthalmology and Visual Sciences, Kellogg Eye Center, University of Michigan, Ann Arbor, Michigan 48105, USA. |
| Abstract |
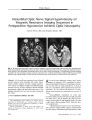
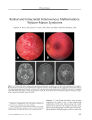
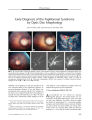
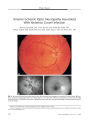
A 7-year-old girl who failed a vision screening examination was found to have a retinal arteriovenous malformation (AVM) in her right eye along with a small angioma of her right lower lip. Magnetic resonance imaging and cerebral angiography revealed a large AVM involving the thalamus and basal ganglia as well as a small AVM involving the right ophthalmic artery. The combination of retinal and intracranial AVMs is known as Wyburn-Mason syndrome. The retinal AVMs of this syndrome do not grow or bleed. Visual loss is usually the result of optic neuropathy from associated orbitocranial AVMs. The natural course of the intracranial AVMs of this syndrome is poorly documented. However, they tend to be extensive and inaccessible and therefore difficult to treat. |
| Subject |
Cerebral Angiography; Child; Female; Hemangioma, pathology; Humans; Intracranial Arteriovenous Malformations, complications; Intracranial Arteriovenous Malformations, diagnosis; Lip Neoplasms, pathology; Magnetic Resonance Angiography; Ophthalmic Artery, abnormalities; Retinal Artery, abnormalities; Retinal Vein, abnormalities; Syndrome |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225438 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s69058t8/225438 |