| Title |
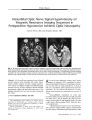
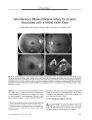
Camputed Tomography Demonstrates Short Axial Globe Length in Cases with Idiopathic Intracranial Hypertension |
| Creator |
Madill, SA; Connor, SEJ |
| Affiliation |
Eye Department, King's College Hospital, London, UK. samadill@hotmail.com |
| Abstract |
BACKGROUND: Cases with idiopathic intracranial hypertension (IIH) have been anecdotally found to demonstrate relatively short axial lengths on ultrasound A-scans. This finding has not been rigorously documented. We therefore systematically investigated globe shape in these cases using computed tomography. METHODS: Computed tomographic 0.625-mm sections of 10 cases with IIH and 10 control subjects were reformatted on a workstation. Globe lengths and widths were measured from axial reformats. Globe lengths and heights were measured from oblique sagittal reformats. Two masked observers took all the measurements. RESULTS: The mean axial lengths of the globes of cases with IIH were significantly shorter than those of controls (t test for independent samples, P<0.001). Both observers also found globe height to be significantly greater than globe length in oblique sagittal sections of cases with IIH compared with control subjects (Mann-Whitney U tests, P<0.01). The difference between length and width in axial sections was not different between cases with IIH and control subjects. Using a critical cutoff of 0.6-mm difference between globe height and length in oblique sagittal sections returned a sensitivity of 0.75 and a specificity of 0.75 for IIH detection from both right and left eyes. CONCLUSIONS: There are significant differences in globe shape and axial length between cases with IIH and control subjects. The differences in globe shape manifest significantly only in oblique sagittal sections. This imaging sign could be a useful marker for subclinical IIH. |
| Subject |
Adult; Anthropometry; Eye, pathology; Eye, radiography; Female; Humans; Male; Middle Older people; Orbit, pathology; Orbit, radiography; Pseudotumor Cerebri, diagnosis; Tomography, X-Ray Computed |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225432 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s69058t8/225432 |