| Title |
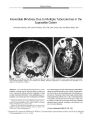
Pituitary Apoplexy Causing Optic Neuropathy and Horner Syndrome without Ophthalmoplegia |
| Creator |
Shin, RK; Cucchiara, BL; Liebeskind, DS; Liu, GT; Balcer, LJ |
| Affiliation |
Department of Neurology and Ophthalmology, University of Pennsylvania School of Medicine, 3400 Spruce Street, Philadelphia, PA 19104, USA. |
| Abstract |
A 47-year-old woman presented with headache, acute monocular vision loss, and ipsilateral Horner syndrome. Apart from the optic neuropathy, all cranial nerve function was intact. Magnetic resonance imaging revealed an enlarged pituitary gland with compression of the orbital apex. The surgical specimen was consistent with pituitary apoplexy. The combination of headache, acute visual loss, and ipsilateral Horner syndrome without ophthalmoplegia, which may suggest carotid artery dissection, is evidently an unusual manifestation of pituitary apoplexy. |
| Subject |
Anti-Inflammatory Agents/administration & dosage; Female; Headache/etiology; Horner Syndrome/diagnosis; Horner Syndrome/drug therapy; Horner Syndrome/etiology; Humans; Magnetic Resonance Imaging; Middle Older people; Ophthalmoplegia/etiology; Optic Nerve Diseases/diagnosis; Optic Nerve Diseases/drug therapy; Optic Nerve Diseases/etiology; Pituitary Apoplexy/complications; Pituitary Apoplexy/diagnosis; Pituitary Apoplexy/drug therapy; Vision Disorders/etiology |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225299 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6671k7b/225299 |