| Title |
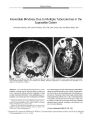
Sarcoidosis of the Anterior Visual Pathway |
| Creator |
Frohman, LP; Guirgis, M; Turbin, RE; Bielory, L |
| Affiliation |
Institute of Ophthalmology and Visual Sciences, UMDNJ-New Jersey Medical School, 90 Bergen Street, Newark, NJ 07103, USA. Frohman@umdnj.edu |
| Abstract |
OBJECTIVES: To describe the clinical spectrum and a rational approach to the diagnosis of anterior visual pathway sarcoidosis. METHODS: Retrospective chart review of all patients examined in neuro-ophthalmic consultation by 1 author from 1989 to 1998 with a diagnosis of sarcoidosis. RESULTS: There were 24 patients (17 female, 7 male, mean age 40 years) with anterior visual pathway sarcoidosis, 17 (71%) of whom were not previously known to have sarcoidosis. Visual acuity ranged from 20/20 to NLP. Normal fundi were observed in 15%. Among the 85% who had fundus abnormalities, pallor was present in 55%, disc edema in 26%, periphlebitis/sheathing in 14%, and optic disc granuloma in 10%. Ten patients (42%) had uveitis, active in only 3 (13%). An elevated angiotensin-converting enzyme (ACE) was present in 16 (76%) of 21 patients tested; evidence of sarcoidosis on chest radiograph was present in 13 (72%) of 18; gallium scanning was abnormal in 13 (93%) of 14; neuroimaging abnormalities of the optic nerves, chiasm, or tract were present in 16 (70%) of 23; lymphocytic pleocytosis or elevated cerebrospinal fluid protein was identified in 14 (88%) of 16 patients, with both values elevated in 7 (44%) patients. Histologic confirmation was obtained in 13 (81%) of 16 who underwent biopsy; in the remaining patients, diagnosis was based entirely on clinical and laboratory evidence. CONCLUSIONS: Anterior visual pathway disease may be underrecognized as a presentation of sarcoidosis. Classic fundus findings of periphlebitis and optic granuloma are typically absent. An aggressive diagnostic evaluation may help establish the diagnosis early in its course. |
| Subject |
Adult; Older people; Diagnostic Techniques, Ophthalmological; Eye Diseases/diagnosis; Eye Diseases/etiology; Female; Humans; Magnetic Resonance Imaging; Male; Middle Older people; Optic Nerve Diseases/complications; Optic Nerve Diseases/diagnosis; Sarcoidosis/complications; Sarcoidosis/diagnosis; Visual Acuity; Visual Pathways/pathology |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225296 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6671k7b/225296 |