| Title |
Irreversible Blindness Due to Multiple Tuberculomas in the Suprasellar Cistern |
| Creator |
Sharma, K; Pradhan, S; Varma, A; Rathi, B |
| Affiliation |
Department of Neurosurgery, Sanjay Gandhi Post-Graduate Institute of Medical Sciences, Lucknow (U.P.) 226014, India. kumud@sgpgi.ac.in |
| Abstract |
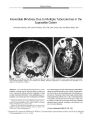
A 14-year-old girl developed fever, severe headache, vomiting, and no light perception in both eyes over a 3-day period without a previous complaint of visual or other neurologic difficulties. Neuro-ophthalmologic examination was normal apart from meningismus and blindness. Brain imaging showed ventriculomegaly and multiple enhancing nodules around the optic chiasm. Lumbar puncture showed an elevated opening pressure with lymphocytic pleocytosis. Polymerase chain reaction and enzyme-linked immunoabsorbent antibody tests on the cerebrospinal fluid were positive for Mycobacterium tuberculosis. There was no evidence of tuberculosis elsewhere in the body. Standard antituberculous treatment, including corticosteroids, did not reverse the blindness. |
| Subject |
Adolescent; Antitubercular Agents/therapeutic use; Blindness/etiology; Cerebrospinal Fluid/microbiology; Cisterna Magna/pathology; Female; Humans; Magnetic Resonance Imaging; Mycobacterium tuberculosis/isolation & purification; Tuberculoma, Intracranial/complications; Tuberculoma, Intracranial/diagnosis; Tuberculoma, Intracranial/drug therapy |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225300 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6671k7b/225300 |