| Title |
Macular Hole: A Rare Complication of Ocular Bartonellosis |
| Creator |
Alterman, Michael A; Young, Blair K; Eggenberger, Eric Robert; Kaufman, David I; McCulley, Timothy J |
| Abstract |
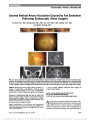
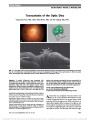
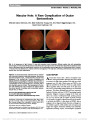
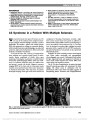
A 37-year-old woman presented with an anterior optic neuropathy related to Bartonella henselae. Twenty-nine days after symptom onset, a partial thickness macular hole developed in the involved eye. Fundus photography and optical coherence tomography confirmed the conversion to a full-thickness macular hole in 2 months. Macular hole as a complication of cat scratch disease is a rare entity, with 2 prior reported cases in children. The development of a macular hole following cat scratch disease can appear without the clinical picture of multiple white chorioretinal lesions, macular star, or vitritis. |
| Subject |
Bartonella Infections; Female; Fluorescein Angiography; Humans; Middle Older people; Optic Nerve Diseases; Retinal Perforations; Tomography, Optical Coherence |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
227451 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6mh0vk7/227451 |