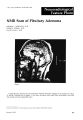
| OCR Text |
Show J. crin. Neuro-opllthalmol. 4: 229-238, 1984. Cecocentral Scotomas in Gliomatosis Cerebri ROBERT T. SPECTOR, M.D.* J. LAWTON SMITH, M.D. JOSEPH C. PARKER, JR., M.D. Abstract A previously healthy 69-year-old white male presented with slowly progressive, painless loss of vision in both eyes. Bilateral cecocentral scotomas were found, and this was his only chief complaint for 9 months. Signs of progressive neurologic dysfunction ensued, and the patient was followed through a complete neuropathologic study at postmortem examination. To our knowledge, this is the only reported instance of pathologically confirmed gliomatosis cerebri with an initial presentation of bilateral chronic cecocentral scotomas. We recently encountered a 69-year-old white male who presented with slowly progressive painless loss of vision in both eyes as his c~ief complaint for a period of over 9 months. ThiS IS the first report, to our knowledge, of pathologically confirmed gliomatosis cerebri with an initial presentation of chronic bilateral cecocentral scotomas. Case Report In February 1981, a 69-year-old white male presented to his ophthalmologist in Tampa, Florida, because he thought his glasses needed changing. The patient's initial complaint was that he was having difficulty differentiating red from green traffic lights as well as noting a decrease in his visual acuity. Glasses were prescribed, and over the next 6 months he had two more changes in his prescription. The patient continued to note painless and steadily decreasing acuity, and was seen again in September 1981, when a visual acuity of 20/200 in both eyes was recorded. Perimetric examination revealed bilateral central scotomas. The remainder of his ocular examination was within normal limits. The patient was started on folic acid by mouth for 2 weeks and received From the Bascom Palmer Eye Institute. University of Miami School of Medicine, Miami, Florida. • Dr. Spector is with Greenwich Ophthalmology Associates, and is Assistant Professor of Clinical Ophthalmology, Columbia University. ew York, New York. December 1984 a single injection of vitamin B12 . On follow-up examination a few weeks later, no subjective or objective improvement in his vision was noted. He was then hospitalized at Tampa General Hospital on October 11, 1981, for neurological evaluation. A thorough history for toxin exposure was negative. Dietary history revealed a satisfactory well-rounded diet, and the patient denied a history of tobacco or alcohol excess. A CT scan of the brain and orbits with a metrizamide study (Fig. 1) revealed no abnormalities, but some degree of empty sella syndrome was present. Electroencephalogram and visual-evoked potentials was reported as unremarkable. The patient was then referred to the Bascom Palmer Institute. Neuro-ophthalmological examination on November 12,1981, revealed that the patient's only complaint was a bilateral painless visual loss. His corrected acuity was 13/200 in both eyes. He could identify only one of 15 AO pseudoisochromatic color plates with each eye. The peripheral visual fields were full, but he had dense bilateral central scotomas (Fig. 2). On the tangent screen, however, a cecocentral component was definitely elicited. There appeared to be a nucl~us of density in the scotoma, in that the central scotoma was more depressed than the ·waist" or cecocentral connection. The scotomas were much larger to colored targets than to white targets. Ophthalmoscopy showed some temporal pallor of the discs in both eyes, and this was more marked in the left eye (Figs. 3 and 4). The initial impression was that the diagnosis of nutritional optic neuropathy or toxic amblyopia had not been absolutely excluded. The patient was treated with hydroxocobalamin 1,000 /lg/ml by 1 cc injections intramuscularly at weekly intervals for 10 weeks. He was then asked to return for a follow-up examination. The patient was seen again on May 3, 1982. At that time, upon taking an interval history, the patient's wife (a registered nurse) volunteered some definite changes in the patient's history from his previous state. She noted that her husband would now repeat answers to questions 229 Cecocentral Scotomas Figure 1. Cc1mputed t'lTI1Ugraphic (CT) scan made OClL1ber 13, 1981, with a cuwnal \'ielV uf metrizamide studY showing lmlv 5<101" degree uf empty 5ella. ArTlnvs dll(ument metrizamide within the sella. jls Date 11-12-81 _ Operator _ 3/330 W (0) int TeH object. sc Aimark petlmeter VISUAL FIELDS (peripheral) 3/330 W (0) int Test object' l/~36 W (6.6 tnt for central scotomas) LE. R.e. Yi.loll _ 1J120Q (1-6 Vlaioll__~ _ Figure 2. Peripheral visual fields on November 12. \98\, 9 months after the onset of progressive visual loss. Dl>cumenl intdct peripheral fields with dense bilateral cecocentral scotomas are present. 230 Journal of Clinical Neuro-ophthalmology Spector, Smith, Parker Figure 3. Right "ptic disc Figure 4. Left optic disc (temporal pallor more easily seen in this picture) Arrow notes palll>f of papillomacular bundle area. December 1984 231 Cecocentral Scotomas Operator jls _ Date 5-3-82 - VitlOil _~"-"-'~_ Test object. 3/330 W (0) int sc Aimark perimeter I.E. VISUAL FIELDS ~~;\:;.\... ~ ..U 3/330 W (0) int sc Test DbjectL' _ 11/ 00 Vll'~D _ Figure 5. Visual (ield~ \~n tV1d~' 3, 1482, nt'.lrl~J 7 nl0nths after the e,aminati(Jn 5t:'en in Fig. '") In addition to bilateral ll'l'll(t'ntr,-1] ~l-lltllnlJ~. theft' i.... Ilc,)W ,-1n Inll)ngrullus rIhht htlnl0nyn1uus ht.:·nlianl lpia, denser JDOVt', consistent wIth left uptlL tract ll1\uhl'Tlwnl. Nute that acuitl' i5 IdeTltIcal with that noted In Fig. 2 Figure 6. Computed tomographic scan shows normal optic nerves and clinoids on May 4, 1982. three or four times. He also had developed dysphagia and would choke two to three times a day. He had begun to tire very easily on trivial efforts. His gait had become much slower over the past month, and he had a tendency to stagger and veer to the right while walking. Examination now revealed that the acuity was once again 13/ 200 best-corrected in both eyes. However, the visual fields now demonstrated a dense, incongruous right homonymous hemianopia, superimposed on the cecocentral scotomas (Fig. 5), pointing to involvement of the left optic tract. He showed evidence of dementia, disorientation, and difficulty with spatial orientation. 232 The patient was admitted to the Bascom Palmer Eye Institute. Computed tomography (Figs. 6-9) now showed a definite lesion in the white matter of the left side of the brain. This appeared to be compromising the frontal horn of the left lateral ventricle with a mass effect shifting to the right. A digital subtraction angiogram showed no evidence of aneurysm. An electrocephalogram showed evidence of involvement in the left hemisphere. Because of the rapid progression of dementia and left hemispheral white matter signs, further invasive workup was advised. With visual loss, dementia, and rapid progression, the possibility Journal of Clinical Neuro-ophthalmology December 1984 Figure 7. Enhanced a"lal CT scan shuws normal cavernuus sinus regluns and minimall v emptv sella appearance. Figure 8. CT scan now shows abnormality primarily in white matter of left hemisphere (arrows). Figure 9. CT scan of May 4. 1982. showing compression uf frontal horn of left lateral ventricle at this point. Spector. Smith. Parker 233 Cecocentral Scotomas Figure 10. Dlabram uf bram sectIOns-an e'densi\'t' \\'ell-dlfferentidted fibrillary astwcytuma (hash marks) m\'l)I\'es the right and left limbic "',terns mcludlJ1b hl'puthalamus. basal ganglia, tempural lubes. and left parietu-uccipital lubes. In twu areas (dark reblunsl. th~ malibnant gliuma had murphulupc features uf a ghublastoma multiforme. Figure 11. Scattered thwughout the limbic system in both cerebral hemispheres, there is an extensive fibrillary and pilacy tic astrllCytllma charactl'nzed by increased astrocytes with a fuca I fasicicular pattern. (H&E, original magnification X250.) 234 Journal of Clinical Neuro-ophthalmology of Jakob-Creutzfeldt disease arose, and brain biopsy was advised. A left parieto-occipital craniotomy with brain biopsy was performed at the Veterans Administration Hospital in Tampa, Florida, with a chosen area that was affected by the mass on computed tomography. The pathological report of the biopsy specimens was malignant fibrillary astrocytoma. The patient was placed on Decadron and showed only modest improvement in mentation. On September 15, 1982, he lapsed into a coma, and stayed relatively the same until his death in early December 1982. A postmortem examination was obtained. Pathological Findings Multiple macroscopic coronal and horizontal sections of the brain, brain stem, and cerebellum demonstrated mildy dilated nonobstructive lateral ventricles. Minimal nonocclusive cerebral atherosclerosis was evident. No increased mass effect was apparent. The centrum semiovale had focal dusky gray areas, particularly in the left anterior temporal lobe. Multiple firm adhesions were seen in the tip of the right and left temporal horns. A diagram of brain sections is seen in Spector, Smith, Parker Figure] O. This revealed an extensive well-differentiated fibrillary astrocytoma (hash marks) involving the right and left limbic systems including the hypothalamus, basal ganglia, temporal lobes, and left parieto-occipital lobe. In two areas (dark regions), the malignant glioma had morphologic features of a glioblastoma multiforme. Multiple histological sections from the brain, brain stem, and cerebellum demonstrated focally reduced myelin in the centrum semiovale with widespread atypical fibrillary and pilocytic astrocytes (Fig. 11) associated with microcystic changes, fascicular patterns, capillary proliferations, and scattered atypical and malignant gemistocytes. Focal perivascular hemosiderin was seen. The focal fascicular pattern is seen in Figure 11. The extensive fibrillary pattern of the astrocytoma is shown in Figure 12. This well-differentiated fibrillary astrocytoma had focal cellular pleomorphism and isolated calcifications and involved the cerbral cortex, leptomeninges, left optic radiation, optic chism, right and left anterior and posterior hypothalamus, right and left internal capsules, right and left frontal lobes, left inferior basal ganglia, anterior temporal lobes, right optic tract, right lateral geniculate body, posterior corpus callosum, left superior parieto- Figure 12. Note fibrillary pattern of astrocytoma here. (H&E, original magnification x250). December 1984 235 Cecocentral Scotomas Figure 13. Within left upper parietu-uccipltal and right basal ganglia regiuns. the well-diiierentiated fibrillary astrocytoma possesses giant tumor cells and many malignant gemistocytes consistent with a glioblastoma multiforme. (H&E. original magnification X250). occipital lobe, right parietal lobe, midbrain, substantia nigra, and upper basis pontis. Within the left upper parieto-occipital lobes and right basal ganglia, Figure 13 documents giant tumor cells and many malignant gemistocytes consistent with a glioblastoma multiforme. This multifocal glioblastoma multiforme showed focal necrosis (Fig. 14) surrounding a cellular pleomorphic glioma. These two disparate areas in this malignant gliomatosis cerebri which showed glioblastoma multiforme changes, manifested by necrosis, uninucleated and multinucleated tumor giant cells, increased vascularity, endothelial proliferation, and adjacent malignant fibrillary astrocytosis, were in right basal ganglia and left superior occipital lobe. Sections of the eye demonstrated cystic retinal changes with reduced internal ganglionic cells. No significant Alzheimer's senile changes or other degenerative alterations were evident. I. 2 Discussion Cecocentral scotomas are visual field defects indicating disease involving the papillomacular 236 bundle region of the optic nerves. There are varied etiologic causes for such field defects. With bilateral cecocentral scotomas, the most common etiology that must be considered is nutritional optic neuropathy or tobacco-alcohol amblyopia. A history of poor nutrition, especially concerning the Bcomplex vitamin group, is elicited from such patients. Other causes for bilateral cecocentral scotomas include dominant optic atrophy, optic nerve hypoplasia, bilateral demyelinating optic neuritis, postinfectious optic neuritis, bilateral optic pits, and pernicious anemia. Patients with bilateral cecocentral scotomas due to either genetic or congenital optic nerve disease may be asymptomatic or usually present much earlier in life than this patient. Examination of family members is particularly helpful in making that diagnosis. The patient here reported presented with symptoms of bilateral cecocentral scotomas which progressed over a period of 9 months. During that period of time, neurologic dysfunction was otherwise conspicuous by its absence. It is well known that optic gliomas of adulthood vary greatly from the optic gliomas of childhood.3-6 Journal of Clinical Neuro-ophthalmology Spector, Smith, Parker - o' • ~. ... Figur~ 14. This mullifOl:oll glioblolSlomol multiformf' has fOl:oll nKl'OSis (upper olnd lower fields) surrounding ol cellulolr pll:,omorphic g1iom.l. (H&:E. origiNI moigniflCiloon )(250). The gliomas of childhood, of the so-called hamartomatous type, usually are limited in their growth potential. Such gliomas of childhood are usually located in either the orbital optic nerve or in the chiasm. With the former, the presenting symptom is uniocular visual loss, proptosis, or strabismus, and the chiasmal gliomas present with visual loss. The malignant form of glioma in the adult has presenting signs somewhat similar to the chiasmal glioma in childhood, but the pace of symptomatology is much quicker. The patient with malignant optic glioma as an adult may mimic either a binocular or uniocular optic neuritis. 7 Progression of the disease is noted to be complete within 6 weeks to 4 months. Uniformly. all patients with adult malignant optic glioma die within several months after the loss of vision. At postmortem examination, the malignant optic glioma is noted to invade adjacent "normar tissue, verifying the fact of its aggressive behavior. 8 It is still open to debate whether the tumor of malignant optic glioma is a '"hamartomatous tumor~ that enters a rapid growth phase, or if the tumor is truly acquired during adult life. The December 1984 abruptness of symptomatology certainly reflects the tumor's rapid growth. In the case presented herein, the gliomatosis cerebri probably began in both optic nerves, subsequently involved the chiasm, and spread through the left optic tract. The growth of the tumor involved invasion of cerebral structures, making surgical resection virtually impossible. The response of chiasmal gliomas to irradiation therapy has varied in various reports,' although we have noted a beneficial effect in our experience. HI The term '"gliomatosis cerebri'" is an interesting one. An excellent review of 32 cases reported ug to 1974 was presented by Couch and Weiss. I Gliomatosis cerebri is applied to a type of glioma in which there is diffuse overgrowth within the nervous system of neoplastic cells (usually of the astrocytoma or glioblastoma multiforme series) which tend to infiltrate extensively; yet neuronal elements are preserved except in areas of dense infiltration. Nevin12 proposed the name '"glioma~ tosis cerebri'" in 1938 in a report of three cases. Clinical manifestations were primarily mental de- 2J7 Cecocentral Scotomas terior.1tion. personality changes. seizures, and increased intracranial pressure signs. Focal neurologic signs appeared late in the course. Seventeen articles dealing with 32 cases were reported between 1938 and 1974, according to Couch and Weiss. The t('rm Mgliomatosis cerebr( generally was used in the English reports, while the Germans favored Scheinker's designation of "diffuse cerebral glioblastosis.· The origin and spread of this tumor has been of great interest to pathologists. Personality and mental status changes were the most frequent symptoms of the disease occurring in 25 of 32 previously reported cases. These changes were followed by hemipareses, ataxia, papilledema, headache, seizure, and nausea and vomiting. The patient here reported was unique in that the process started in optic nerves, and then spread to chiasm. [eft optic tract, and subsequently extensively throughout the brain. Computed tomography revealed no evidence of mass effect early in the course of the disease and made the diagnosis even more difficult to make. Nuclear magnetic resonance might hopefully lead to earlier detection of such a case_ Summary This is a case of gliomatosis cerebri in a 69year- old man, who presented with bilateral cecocentral scotomas. After a literature search, we believe this to be the only case report of gliomatosis cerebri with such a chronic initial presentation. This rare tumor enlarges in the brain with no focal neurologic signs until quite late. Computerized tomography will usually show no changes eilrly in the course of the diseilse, because of the isodense nature of the tumor to brain tissue. Other laboratory examinations were noted to be completely normal. The diagnosis and its differential would include any neurologicill disorder with multiple areas of involvement. The diagnosis went from nutritional optic neuropathy. later to possible Jakob-Creutzfeldt disease. and was only established definitely by brain biopsy and subsequently autopsy. Though the diagnosis was not made for several months. there is little ilvailable therapy to notably mollify the natural course of this disease process. If the diagnosis could have been made eilrlier. a course of irr.1diation therapy could be tried. 238 References I. Anderson. D.R., and Spencer. W.H.: Ultrastructure and histochemical observations of optic nerve gliomas. Arch.Ophtlwlmol. 83: 324-335, 1980. 2. Luse. S.A.: Ultrastructure of reactive and neoplastic astrocytes. Lall. [uuesl. 7: 401-417,1958. 3. Baril. A.. and Richardson. E.P., Jr.: The biological and clinical behavior of pilocytic astrocytomas of the optic pathways. Brai'l 105: 161-187, 1982. 4. Yanof(, M.. Davis, R.L and Zimmerman, L.E.: Juvenile pilocytic astrocytoma of optic nerve: C1in· icopathologic study of sixty-three cases. In Ocular mId Adl/l'.ml Tllm(lr~. F. A. Jacobiec, Ed. Aesculapiu&. Birmingham, Alabama. pp. 685-707. 5. Hoyt, W,F., and Baghdassarian. S,A.: Optic nerve glioma uf childhood. Natural history and rationale for conservative management. Br. f. api/Ilia/mol. 53: 793-798. 1969. 6. Wong, I.G., and Lubow, M.: Management of optic nerve glioma of childhood: a review of 42 cases. In N,·lIr,,-ol/Mhalmology. Vol. 6, J. L Smith, Ed. C. V. Mosby. SI. Louis, 1972, pp. 51-60. 7. Pfaffenbach, D.o., Kearns. T.P., and Hollenhorst, R.W.: An unusual case of optic nerve-chiasmal glioma. Alii. f. Oplil/1Olmol, 75: 523-525, 1972_ 8. Hovt. W.F,. Meshe!. l.G .. Lessell, S., Schatz. N.J., and Suckling. RoO.: Malignant optic glioma of adulthood. Bmin96: 121-132, 1973. 9. Glaser, J.S., Hovt, W.F.. and Corbell, J.: Visual morbidity with chiasmal glioma. Arch Ol/hlhalmol, 85: 3-12.1971. iO Parker, J.C, Jr., et ill.: Chiilsmal optic glioma after radiation therapv. Neuro-ophthalmologic/pathologic correlation: f. Clin. N.'JlnHlplrlhalmol. 1: 3143, 1981 11. Cuuch, J.R., and Weiss, S.A.: Gliomatosis cerebri. Report of four cases ,1nd review of the literature. N"IIr1ll'lX!1 24: 504-511.1974 Acknowledgments The authors th,mk Drs. Gilbert Echelman, Waite Kirkcunnell. and J E. Milnis(ako, the Pathology Dep. utment of 51. Joseph's Hospital. Tampa, Floridil. and i111 uthers wlw helped refer, provide information, or care for the patient hert' reported Particular gratitude is due tu the p.ltient's wift' who cooperated in a notable m,mn",r 10 hl'lp provide all "f the milterial neCeSSary fllr this investigilli'ln. . Wri,,, {,'r reprin'._ Ill,· Robert T. Spector, M.D., Grt'en· wkh Ophth,llmulugv Associates. Dt'i1rfield Medical Buildinf;. 4 Dl'Mfield Driw. Greenwich, Connecticut 06~30. Journal of Clinical Neuro-ophthalmology |