| OCR Text |
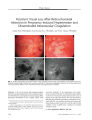
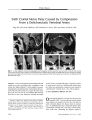
Show PHOTO ESSAY Persistent Visual Loss After Retinochoroidal Infarction in Pregnancy- Induced Hypertension and Disseminated Intravascular Coagulation Nishal Patel, MRCOphth, Paul Riordan- Eva, FRCOphth, and Victor Chong, FRCOphth FIG. 1. Fundus photography ( top) taken within 3 days of delivery shows patchy retinal edema in the posterior pole with intraretinal hemorrhages. Visual acuity was finger counting OU. Fluorescein angiography ( bottom) in the late phase shows extensive perfusion defects of the choroidal circulation accompanied by late leakage. Abstract: A 40- year- old woman had pregnancy- induced hypertension, disseminated intravascular coagulation ( DIC), choroidal infarction, and magnetic resonance imaging ( MRI) high- signal abnormalities in the occipital regions. With Retinal Research Unit, King's College Hospital, University of London, London, England. Address correspondence to Dr. Nishal Patel, Retinal Research Unit, Normandy Building, King's College Hospital, University of London, Denmark Hill, SE5 9RS, London, England; E- mail: drnishl975@ yahoo. w i l l . Ill-. ll. ll .' v'IVIIII. 1 w i l l successful treatment of the hypertension and spontaneous resolution of the DIC, the MRI signal abnormalities resolved, but visual acuity remained decreased because of damage to the retina and choroid. This case demonstrates that pregnancy- induced hypertension, particularly if combined with DIC, may produce infarction of the retina and choroid and persistent visual loss even if the effect of this condition on the occipital lobes is limited to reversible vasogenic edema. { JNeuro- Ophthalmol 2005; 25: 128- 130) 128 J Neuro- Ophthalmol, Vol. 25, No. 2, 2005 Photo Essay J Neuro- Ophthalmol, Vol. 25, No. 2, 2005 FIG. 2. T2- weighted magnetic resonance images performed 2 days after delivery ( A) and 3 months later ( B). In A, there are high- signal regions in the occipital subcortical white matter bilaterally. In B, the scan is normal. The disappearance of the abnormal signal indicates that the original abnormality represented vasogenic edema. A fter the delivery of twins by caesarean section, a 40- year- old woman had pregnancy- induced hypertension. She was treated successfully with intravenous labe-talol 200 mg twice daily for 2 days to control an initial blood pressure of 210/ 140, followed by the same dose orally for 5 days. A low platelet count ( 92,000), a raised fibrinogen level ( 5.5), and an elevated fibrin degradation product D- dimer ( 1.6 | Jig/ mL, normal < 0.4 | jim/ mL) indicated disseminated intravascular coagulation, which resolved spontaneously without treatment. Visual acuity was 20/ 20 OU after delivery but deteriorated 5 days later to finger counting at 3 feet OU. Goldmann visual fields revealed bilateral central scotomas. Ophthalmoscopy showed pallid retinal edema with scattered hemorrhages at both posterior poles ( Fig. 1 top). Fluorescein angiography showed extensive choroidal ischemia in the macular region accompanied by late leakage from retinal vessels OU ( Fig. 1 bottom). Magnetic resonance imaging ( MRI) T2 and FLAIR sequences performed 2 days after delivery showed subcortical and cortical high- signal predominantly within the occipital regions bilaterally ( Fig. 2A). This signal change was initially believed to represent watershed infarction ( diffusion- weighted MRI was not performed). However, a repeat MRI 3 months later showed no abnormalities on the same pulse sequences ( Fig 2B). At 12 months after delivery, visual acuity had improved to 20/ 200 OD and 20/ 120 OS and ophthalmoscopy showed bilateral optic disc pallor indicative of inner retinal and/ or optic nerve infarction and macular pigmentary changes indicative of choroidal infarction ( Fig. 3). The reversal of the MRI abnormalities indicates that the initial signal change did not represent watershed ischemia, but rather vasogenic edema associated with hypertensive encephalopathy ( 1). Identical MRI signal abnormalities are seen in patients treated with cyclophilins ( cyclosporine or tacrolimus). Discontinuation of the agent leads to clinical and imaging recovery ( 2,3). The persistent visual loss in our patient is caused by ischemic damage to the retina and choroid. In most cases of retinochoroidal ischemia in the setting of pregnancy- induced hypertension, the visual prognosis is good ( 4). In this case, the poor outcome may reflect the superimposition of disseminated intravascular coagulation, itself known to be a risk factor for choroidal ischemia ( 5). Our case demonstrates that pregnancy- induced hypertension, particularly if combined with disseminated intravascular coagulation, may infarct the retina and choroid FIG. 3. Fundus photography performed 14 months after delivery shows the late effects of retinochoroidal infarction OU, as evidenced by optic disc pallor and pigment deposition in the macular regions. Visual acuity was 20/ 200 OD and 20/ 120 OS. 129 J Neuro- Ophthalmol, Vol. 25, No. 2, 2005 Patel et al even if the effect of this condition on the posterior brain hemispheres is limited to reversible vasogenic edema. REFERENCES 1. Jungensen JS, Nibble L, Hoffmann KT, et al. Postpartum blindness. Lancet 2001; 358: 1338. 2. Cosottini M, Lazzarotti G, Ceravolo R, Michelassi MC, Canapicchi R, Murri L. Cyclosporine- related posterior reversible encephalopathy syndrome ( PRES) in non- transplant patient: a case report and literature review. Eur J Neurol 2003; 10: 461- 2. 3. Wong R, Beguelin GZ, de Lima M, Giralt SA, Hosing C, Ippoliti C, Forman AD, Kumar AJ, Champlin R, Couriel D. Tacrolimus- associated posterior reversible encephalopathy syndrome after allogeneic haematopoietic stem cell transplantation. Br J Haematol 2003; 122: 128- 34. 4. Sathish S, Arnold JJ. Bilateral choroidal ischaemia and serous retinal detachment in pre- eclampsia. Clin Exper Ophthalmol 2000; 28: 387- 90. 5. Kinyoun JL, Kalina RE. Visual loss from choroidal ischemia. Am J Ophthalmol 1986; 15; 101: 650- 6. 130 © 2005 Lippincott Williams & Wilkins |