| OCR Text |
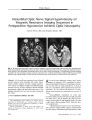
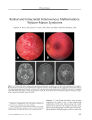
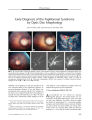
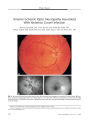
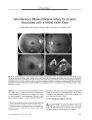
Show ORIGINAL CONTRIBUTION A Case of Posterior Ischemic Optic Neuropathy in a Posterior- draining Dural Cavernous Sinus Fistula Masato Hashimoto, MD, Kenji Ohtsuka, MD, Yasuo Suzuki, MD, and William F. Hoyt, MD Abstract: A 79- year- old woman presented with sudden unilateral visual loss after an ocular motor disturbance and pulsatile tinnitus. Neuro- ophthalmologic examination showed a presumed right posterior ischemic optic neuropathy ( PION), oculosympathetic, and third, sensory fifth, and sixth cranial nerve pareses. Selective angiography of the right internal and external carotid arteries confirmed a posterior- draining dural carotid cavernous sinus fistula ( CCF) fed by the right meningohypophyseal trunk and right middle meningeal artery. Angiography also showed an ophthalmic- middle meningeal arterial anastomosis. We postulate that the PION was caused by an arterial steal, because blood was drawn into the fistula and away from the intraorbital optic nerve. ( J Neuro- Ophthalmol 2005; 25: 176- 179) Posterior- draining dural carotid cavernous sinus fistulas ( CCF), also called " white- eyed shunts," usually cause headache, intermittent pulsatile tinnitus, and third or sixth cranial nerve palsies ( 1- 3). We have not found a report of optic neuropathy caused by a posterior- draining dural cavernous shunt. We present a case in which a presumed posterior ischemic optic neuropathy ( PION) occurred in a patient with a posterior- draining dural CCF and postulate that it arose from a " steal phenomenon," namely a drawing of arterial blood from the optic nerve into the fistula. CASE REPORT A 79- year- old woman developed vertical diplopia with persistent headache and intermittent pulsatile tinnitus in her right ear in July 2003. Several weeks later, she noticed right facial numbness. Two months after the diplopia Department of Ophthalmology, Sapporo Medical University ( MH, KO, YS); and the Neuro- ophthalmology Unit, Department of Ophthalmology, University of California, San Francisco, San Francisco, California ( WFH). Address correspondence to Masato Hashimoto, MD, Department of Ophthalmology, Sapporo Medical University, School of Medicine, S- l, W- 16, Chuo- ku, Sapporo, 060, Japan; E- mail: mashoyu5@ beige. plala. or. jp began, she experienced sudden blindness in her OD. Her son noted that she had an inwardly deviated OD. She had only light perception OD and 20/ 20 visual acuity OS. There was a relative afferent pupillary defect OD and mild right upper lid ptosis. In dim illumination, the right pupil measured 3.0 mm and the left pupil measured 5.5 mm. In bright illumination, both pupils measured 3.0 mm, compatible with a right oculosympathetic paresis. Hertel exophthalmometry showed 12 mm OD and 13 mm OS. There was total absence of abduction and a mild deficit in infraduction OD ( Fig. 1); ductions were full OS. She had hypesthesia in all three divisions of the right trigeminal nerve. Biomicroscopic examination was normal, and intraocular pressures were 15 mm Hg OU. Ophthalmoscopy was normal. Electroretinography gave normal results. These findings indicated an optic neuropathy OD, together with right third, sensory fifth, sixth, and oculosympathetic pareses. Serial dynamic magnetic resonance imaging ( MRI) of the cavernous sinuses showed that the posterior cavernous sinus and inferior petrosal sinus, especially on the right, markedly enhanced in the arterial phase ( Fig. 2). Coronal MRI with short TI inversion recovery ( STIR) technique of the orbit showed high signal intensity in the mildly dilated right superior ophthalmic vein ( SOV), suggesting slow or no flow, and low signal intensity in the distended right inferior ophthalmic vein ( IOV) and left SOV ( Fig. 3), suggesting fast ( arterial) flow. Selective cerebral angiography of the right internal and external carotid arteries confirmed a right posterior-draining dural CCF fed by the right meningohypophyseal trunk and right middle meningeal artery ( Fig. 4). There was some flow across the portal sinus into the inferior petrosal sinus on the opposite side. However, there was no anterior drainage into the ophthalmic veins. Transvenous and transarterial catheters were used to deposit venous coils and arterial polyvinyl alcohol particles into the fistula, which was closed under angiographic guidance. After embolization, we superimposed two images of the right internal carotid angiogram and the right external 176 J Neuro- Ophthalmol, Vol. 25, No. 3, 2005 Posterior- draining Dural Cavernous Sinus Fistula J Neuro- Ophthalmol, Vol. 25, No. 3, 2005 FIG. 1. The patient demonstrates mild right upper lid ptosis, absent abduction, and slightly reduced infraduction OD, findings consistent with right third and sixth cranial nerve palsies. carotid angiogram keyed by the images of the coils in the cavernous sinus. The images disclosed that the ophthalmic artery shared an arterial branch with the middle meningeal artery ( Fig. 5), indicating that our patient had an ophthalmic-middle meningeal arterial anastomosis. This suggested the possibility that the fistula, which had a major supply from the middle meningeal artery, was stealing arterial blood from the ophthalmic artery and robbing the optic nerve of its intraorbital blood supply. One month after embolization, the right oculosym-pathetic had resolved, the third and sixth cranial nerve deficits had partially resolved, but the blindness in the OD persisted. DISCUSSION Dural CCF sometimes produces aseptic cavernous sinus thrombosis ( 1,4). Grove ( 1) found that a majority of patients with these fistulas are middle- aged or elderly women. FIG. 2. Serial dynamic axial magnetic resonance image in the arterial phase discloses enhancement of both cavernous and inferior petrosal sinuses, especially on the right. FIG. 3. Coronal orbit magnetic resonance image with short Tl inversion recovery technique shows high signal of the mildly dilated right superior ophthalmic vein ( arrow) and low signal of the distended right inferior ophthalmic vein ( arrowheads) and left superior ophthalmic vein. 177 J Neuro- Ophthalmol, Vol. 25, No. 3, 2005 Hashimoto et al B FIG. 4. A. Right internal carotid arteriogram shows arterial blood flow into the posterior cavernous sinus ( arrowheads) from the right menin-gohypophyseal trunk. B. Right external carotid arteriogram shows arterial blood flow into the posterior cavernous sinus ( arrowheads) from the right middle meningeal artery. There was no anterior drainage into the ophthalmic veins. In our patient, MRI findings with STIR technique disclosed slow or no flow in the right SOV and fast flow in the distended right IOV These findings suggested that the proximal SOV was thrombosed and that the secondarily dilated IOV compensated for the venous outflow from the orbit. These findings explain why our patient did not have signs of orbital venous congestion. We hypothesize that the outflow from our patient's CCF shifted from an anterior ( orbital) direction to a posterior ( intracranial) direction because of proximal SOV thrombosis. Based on the clinical findings, we believe that sudden unilateral blindness in our patient was caused by PION. Although we do not know the precise cause of the ischemic insult to her retrobulbar optic nerve, we know that it occurred in the setting of an ipsilateral dural CCF. Our demonstration of an anastomotic connection between the middle meningeal and ophthalmic arteries suggests that the optic nerve was being robbed of its normal arterial supply as blood was drawn into the fistula, whose major supply came from the middle meningeal artery. The anterior branch of the middle meningeal artery often gives off an anastomotic ramus, called the accessory ophthalmic artery or the meningolacrimal artery, entering the orbit to join the lacrimal artery. This anastomotic ramus passes through the superior orbital fissure or through the cranio- orbital foramen of Hyrtl in the greater wing of the sphenoid ( 5,6). The incidence of middle meningeal- ophthalmic artery anastomosis in different anatomic studies varies greatly. Gillilan ( 7) found it in 75% of 20 specimens and Hayreh and Dass ( 8) in 2.2% of 170 specimens. Bogousslavsky ( 9) reported a patient with amaurosis fugax resulting from a middle fossa dural arteriovenous malformation partially fed by the recurrent meningeal branch of the ophthalmic artery. He speculated that episodic lowering of ophthalmic artery/ retinal arterial blood pressure might be responsible for the amaurosis fugax. Regrettably, we could not perform retinal fluorescein angiography in our patient ( because of her allergic response to the dye) to show a reduced choroidal t B ^^^- V v / i . % • v . * W i -* FIG. 5. A. Right internal carotid angiogram after embolization. B. Right external carotid angiogram after embolization. They demonstrate that the fistula is closed. C. Superimposed image of ( A) and ( B) keyed by the image of the coils in the cavernous sinus. This tableau demonstrates that the ophthalmic artery ( large arrow) has an arterial feeder ( arrowheads) from the middle meningeal artery ( small arrow). 178 © 2005 Lippincott Williams & Wilkins Posterior- draining Dural Cavernous Sinus Fistula J Neuro- Ophthalmol, Vol. 25, No. 3, 2005 blush in the affected eye, which would have fortified our hypothesis as to the mechanism of the PION. REFERENCES 1. Grove AS Jr. The dural shunt syndrome. Pathophysiology and clinical course. Ophthalmology 1984; 91: 31^ 4. 2. Hawke SH, Mullie MA, Hoyt WF, et al. Painful oculomotor nerve palsy due to dural- cavernous sinus shunt. Arch Neurol 1989; 46: 1252- 5. 3. Acierno MD, Trobe JD, Cornblath WT, et al. Painful oculomotor palsy caused by posterior- draining dural carotid cavernous fistulas. Arch Neurol 1995; 113: 1045- 9. 4. Seeger JF, Gabrielsen TO, Giannotta SL, et al. Carotid cavernous sinus fistulas and venous thrombosis. AJR Am JNeuroradiol 1980; 1: 141- 8. 5. Hayreh SS. Arteries of the orbit in the human being. Br J Surg 1963; 50: 938- 53. 6. Diamond MK. Homologies of the meningeal- orbital arteries of humans: A reappraisal. JAnat 1991; 178: 223^ H. 7. Gillilan LA. The collateral circulation of the human orbit. Arch Ophthalmol 1961; 65: 684- 9. 8. Hayreh SS, Dass R. The ophthalmic artery. II. Intra- orbital course. Br J Ophthalmol 1962; 46: 165- 8. 9. Bogousslavsky J, Vinuela F, Barnett HJ, et al. Amaurosis fugax as the presenting manifestation of dural arteriovenous malformation. Stroke 1985; 16: 891- 3. 179 |