| Title |
Concurrent Sino-Orbital Aspergillosis and Cerebral Nocardiosis |
| Creator |
Pieroth, L; Winterkorn, JMS; Schubert, H; Millar, WS; Kazim, M |
| Affiliation |
Department of Ophthalmology, The New York Presbyterian Hospital-Columbia University Medical College, New York, New York, USA. |
| Abstract |
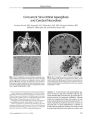
A 79-year-old man with myelodysplastic syndrome developed a right optic neuropathy with optic disc edema and intractable periocular pain, one month after undergoing removal of a gangrenous gallbladder. Although results of a temporal artery biopsy were negative, he was treated with prednisone for presumed temporal arteritis. Attempts at tapering the prednisone dose led to recurrence of periocular pain. On neuro-ophthalmologic evaluation six months after the prednisone treatment was begun, he had developed right fourth and sixth cranial nerve palsies, and magnetic resonance imaging demonstrated a right orbital apex mass. Trans-sphenoidal biopsy revealed Aspergillus fumigatus. During treatment of aspergillosis, the patient developed a left hemiparesis. Magnetic resonance imaging disclosed multiple ring-enhancing cerebral masses. Biopsy revealed Nocardia asteroides. The patient was successfully treated for both infections with recovery of neurologic function except for the right optic neuropathy. Although immunocompromised patients are known to be subject to multiple infections, this may be the first reported case of concurrent sino-orbital aspergillosis and cerebral nocardiosis. |
| Subject |
Older people; Amphotericin B/therapeutic use; Anti-Bacterial Agents/therapeutic use; Antifungal Agents/therapeutic use; Aspergillosis/complications; Aspergillosis/diagnosis; Aspergillosis/drug therapy; Brain Diseases/complications; Brain Diseases/diagnosis; Brain Diseases/drug therapy; Fatal Outcome; Humans; Imipenem/therapeutic use; Magnetic Resonance Imaging; Male; Minocycline/therapeutic use; Nocardia Infections/complications; Nocardia Infections/diagnosis; Nocardia Infections/drug therapy; Orbital Diseases/complications; Orbital Diseases/diagnosis; Orbital Diseases/drug therapy; Paranasal Sinus Diseases/complications; Paranasal Sinus Diseases/diagnosis; Paranasal Sinus Diseases/drug therapy |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225397 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6jh6s9g/225397 |