| OCR Text |
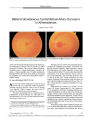
Show LETTERS TO THE EDITOR Rapid Visual Recovery After Coenzyme Q10 Treatment of Leber Hereditary Optic Neuropathy We agree with the conclusion of Mashima et al. ( 1) that the administration of idebenone, vitamin B2, and vitamin C may speed the recovery of vision in patients with Leber Hereditary Optic Neuropathy ( LHON). Recently, we treated a LHON patient with an identical and commercially available drug: ubiquinone, or coenzyme Q10, ( 2,3- dimethoxy- 5- methyl- l, 4- benzoquinone with a side chain of 10 isoprenoid units). His visual acuity ( VA) improved dramatically within 4 months ( 2). Here is a clinical summary of that case: A 21- year- old man noted the sudden onset of a visual disturbance involving the OD in November 1994. In February 1995, he developed visual blurring in the OS. Serial ophthalmologic examinations over the next 6 months revealed a decrease in visual acuity to hand movements OD and finger counting OS. Fundoscopic examination eventually showed profound optic disc pallor in the OD and mild temporal pallor in the OS, and visual fields showed bilateral central scotomas. Fluorescein angiography was unremarkable. Visual- evoked potential examination revealed an absence of P100 waves bilaterally. A homoplasmic point mutation at the 11778 position in a complex I subunit of mitochondrial DNA was noted. Beginning in July 1995, the patient was treated with coenzyme Q10 with an initial oral dose of 90 mg/ d, increasing to 160 mg/ d in the 2nd month, and to 200 mg/ d from the 3rd to the 12th month, after which it was withdrawn. Visual acuity improved to 20/ 30 OD and 20/ 200 OS in November 1995, 4 months after institution of coenzyme Q10. The improvement in vision persisted for the next 4 years, even after withdrawal of the medication. The prognosis for visual recovery is generally dismal in LHON patients with the 11778 A mutation ( 3- 5). Stone et al. ( 6) reported that only five ( 4%) of 136 affected patients recovered 20/ 40 or better visual acuity, and visual recovery never began before 12 months. In the series by Riordan- Eva et al. ( 4), only one treated patient recovered within 10 months after onset of symptoms; in that patient, the type of medication and its dose was not described. In other studies, some recovery of vision did occur in LHON patients with the 11778 A mutation but required several years ( 1,7,8). Our The Journal of Neuro- Ophthalmology welcomes letters as E- mail correspondence. Send to: jdtrobe@ umich. edu. 66 Copyright © Lippincott Williams & Wilkins. Una patient had a marked improvement of visual acuity within 4 months of starting coenzyme Q10 treatment. Chin- Chang Huang, MD Hung- Chou Kuo, MD Chun- Che Chu, MD Ling- Yuh Kao, MD Departments of Neurology ( C. C. H., H. C. K., C. C. C.) and Ophthalmology ( L. Y. K.) Chang Gung Memorial Hospital and University Taipei, Taiwan REFERENCES 1. Mashima Y, Kigasawa K, Wakakura M, et al. Do idebenone and vitamin therapy shorten the time to achieve visual recovery in Leber hereditary optic neuropathy? J Neuro- Ophthalmol 2000; 20: 166- 70. 2. Kuo HC, Huang CC, Chu CC, Kao LY, Lee HC, Pang CY, Wei YH. Coenzyme Q10 treatment in Leber's hereditary optic neuropathy. Neuro- Ophthalmology ( in press) 3. Nikoskelainen E. New aspects of the genetic, etiologic, and clinical puzzle of Leber's disease. Neurology 1984; 34: 1482- 4. 4. Riordan- Eva P, Sanders MD, Govan GG, et al. The clinical feature of Leber's hereditary optic neuropathy defined by the presence of a pathogenic mitochondrial DNA mutation. Brain 1995; 118: 319- 37. 5. Harding AE, Riordan- Eva P, Govan GG. Mitochondrial DNA diseases: genotype and phenotype in Leber's hereditary optic neuropathy. Muscle Nerve 1995; 3: S82- 4. 6. Stone EM, Newman NJ, Miller NR, et al. Visual recovery in patients with Leber's hereditary optic neuropathy and the 11778 mutation. J Clin Neuro- Ophthalmol 1992; 12: 1CM1. 7. Nikoskelainen EK. Clinical picture of LHON. Clin Neurosci 1994; 2: 115- 20. 8. Mashima Y, Hiida Y, Oguchi Y. Remission of Leber's hereditary optic neuropathy with idebenone. Lancet 1992; 340: 368- 9. Optic Nerve Enhancement in Leber Hereditary Optic Neuropathy: Four Years Later In 1999, the first report of a patient with optic nerve enhancement on orbital magnetic resonance imaging ( MRI) J Neuro- Ophthalmol, Vol. 22, No. 1, 2002 reproduction of this article is prohibited. LETTERS TO THE EDITOR JNeuro- Ophthalmol, Vol. 22, No. 1, 2002 in Leber hereditary optic neuropathy ( LHON) was published ( 1). He was an 18- year- old man with a mutation at nucleotide position 3460. Visual acuity was count fingers OD, 20/ 80 OS, and ophthalmoscopy showed elevation with obscuration of the disc margins OU. Gadolinium- enhanced orbital fat- suppressed MRI showed optic nerve enhancement OU ( Fig. 1 left). Four years later, visual acuity improved to 20/ 25 OD, 20/ 25- 2 OS with pale optic discs. Orbital MRI was now normal without optic nerve enhancement ( Fig. 1 right). Enhancement with gadolinium administration denotes disruption of the blood- brain barrier within the optic nerve ( 2). Evidently the blood- brain barrier, as documented by neuroimaging, recovered in the chronic phase of the disease. REFERENCES 1. Vaphiades MS, Newman NJ. Optic nerve enhancement on orbital magnetic resonance imaging in Leber's hereditary optic neuropathy. J Neuroophthalmol 1999; 19: 238- 9. 2. Guy J, Mancuso A, Quisling RG, Beck R, Moster M. Gadolinium- DPTA- enhanced magnetic resonance imaging in optic neuropathies. Ophthalmology 1990; 97: 592- 600. Michael S. Vaphiades, DO Department of Ophthalmology University of Arkansas for Medical Sciences Little Rock, Arkansas Nancy J. Newman, MD Emory University School of Medicine Atlanta, Georgia Errata In the article The Controlled High Risk Avonex ® Multiple Sclerosis Trial ( CHAMPS STUDY) by Steven L. Galetta, which appeared in the December 2001 issue of Journal of Neuro- Ophthalmology ( 2001; 21: 292- 295), on page 294, left column, line 2, " 9%" should be changed to " 91%." On page 295, reference 9, " even" should be changed to " event." 67 Copyright © Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. |