| OCR Text |
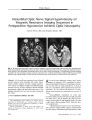
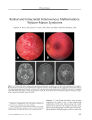
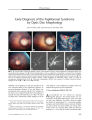
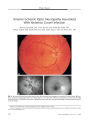
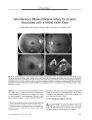
Show PHOTO ESSAY Early Diagnosis of the Papillorenal Syndrome by Optic Disc Morphology Arif O. Khan, MD, and Sawsan R. Nowilaty, MD FIG. 1. A. The disc OD is centrally excavated (" vacant") with multiple " hairpin" vessels suggestive of cilioretinal vessels. The surrounding retina appears thin. B. With scleral depression, there is a significant compromise in vascular flow. C. Doppler ultrasound confirms that the posterior ciliary arteries ( red) are the predominant blood supply to the retina. Left is temporal, right is nasal, and the center vertical line is where central retinal artery flow is normally evident but is not seen here. D. The disc OS is centrally excavated with multiple " hairpin" vessels suggestive of cilioretinal vessels. There is a patch of juxtapapillary depigmentation. E, F, G. Fluorescein angiography confirms the presence of multiple cilioretinal arteries. early diagnosis of the papillorenal syndrome before the potential development of renal dysfunction. { JNeuro- Ophthalmol 2005; 25: 209- 211) Aseven- month- old boy was referred for suspected congenital glaucoma. His medical history was unremarkable, but his father had had poor vision in the right eye since early childhood. The child's vision was central and steady but unmaintained OU. A horizontal pendular nystagmus and variable left face turn were present. Pupillary size and reactivity and ocular motility were normal. Intraocular pressure ( by Tonopen) taken while the child was sleeping was < 10 mm Hg OU. Retinal examination under ( Images are at 10 ( E), 11 ( F), and 14 ( G) seconds.) Abstract: The morphology of optic disc dysplasia is the most consistent finding in the papillorenal syndrome, an autosomal- dominant syndrome of eye and kidney mal-development often associated with the PAX2 mutation. In the absence of a recognized family history, the diagnosis is typically not made until renal disease is evident. We report an infant whose characteristic fundus findings led to the Departments of Pediatric Ophthalmology ( AOK) and Vitreo- Retinal Disease ( SRN), King Khaled Eye Specialist Hospital, Riyadh, Saudi Arabia. Address correspondence to Arif O. Khan, MD, Division of Pediatric Ophthalmology, King Khaled Eye Specialist Hospital, P. O. Box 7191, Riyadh 11462, Saudi Arabia; E- mail: arif. khan@ mssm. edu J Neuro- Ophthalmol, Vol. 25, No. 3, 2005 209 J Neuro- Ophthalmol, Vol. 25, No. 3, 2005 Khan and Nowilaty anesthesia revealed central optic disc excavations, multiple cilioretinal arteries, and a circumscribed patch of depigmentation temporal to the discs OU. With minimal scleral depression, a significant whitening of the retina and optic nerve occurred. Fluorescein angiography and Doppler imaging confirmed the presence of multiple cilioretinal arteries and decreased perfusion of the retina by the central retinal artery ( Fig. 1). Doppler imaging of the kidney demonstrated abnormal medullo- cortical differentiation on the right side ( Fig. 2). Systemic evaluation, including brain magnetic resonance imaging, urinary tract function, and hearing testing, showed no other abnormalities. On further questioning, the father reported having had a kidney transplant at age 32 for adult- onset renal failure of unknown cause. Ophthalmic examination of the father revealed a visual acuity of 20/ 60 OD and 20/ 25 OS, peripapillary atrophy OU, multiple cilioretinal arteries OU, and macular pigmentary changes OD suggestive of prior serous retinal detachments ( Fig. 3). The two siblings of the proband had normal ophthalmic examinations. The proband has normal renal function for his age and is being closely followed by a pediatric nephrologist. PAX2 testing has not been performed. Optic disc appearance is the most reliable finding in the papillorenal syndrome, even more than PAX2 genetic analysis ( 2). Alternate names for the syndrome reflect the variation in clinical findings and include " renal- coloboma syndrome," " optic nerve coloboma with renal disease," " coloboma of the optic nerve with renal disease," and " optic coloboma, vesico- ureteral reflux, and renal abnormalities" ( 1). In the past, the optic nerve head findings in the syndrome have been labeled " morning glory"- like, " optic pit"- like, colobomatous, or dysplastic. More recently, characteristic optic disc features of the syndrome have been recognized ( 2). Disc excavation is classically central, with multiple cilioretinal radial vessels emanating from all quadrants, often making " hairpin" turns over the neural rim. FIG. 2. A. Doppler ultrasound shows abnormal medullo-cortical differentiation in the right kidney. B. The left kidney is normal. When no central vessels are seen in the setting of the excavated disc, the disc has been termed " vacant" ( 3). The optic disc and renal findings may be the result of defective retinal angiogenesis ( 2,3). This hypothesis has not been proven, and an alternate one is that mutation in PAX2 results in abnormal optic stalk development with resultant abnormal vascularity of the optic nerve head ( 4). Patients with the syndrome may develop serous retinal detachments FIG. 3. A. The patient's father's optic nerve head OD has multiple fine cilioretinal arteries emanating from the central disc excavation. B. The father's optic nerve head OS has a more dysplastic appearance. There are also multiple fine cilioretinal arteries. 210 © 2005 Lippincott Williams & Wilkins Papillorenal Syndrome J Neuro- Ophthalmol, Vol. 25, No. 3, 2005 and tend to have thin hypoplastic peripheral retinas ( 2). Doppler ultrasound studies of the optic nerves may show attenuation of central retinal artery flow, but the diagnosis can be made on the basis of multiple cilioretinal arteries emanating from the optic disc ( 2). Renal disease, if present, is variable and usually progressive, often necessitating renal transplantation for chronic renal failure in young adulthood ( 5). Diagnosis of the papillorenal syndrome is typically not made unless there is frank renal disease or the prior recognition of the syndrome in a family member. The presence of characteristic ophthalmic findings, however, can allow earlier diagnosis. Early diagnosis is important, because prophylactic systemic antihypertensive treatment can limit renal morbidity ( 2,5). REFERENCES 1. Online Mendelian Inheritance in Man, OMIM ( TM). Baltimore: Johns Hopkins University, MIM Number: {# 120330}: { 3/ 24/ 2003}: World Wide Web URL: http:// www. ncbi. nlm. nih. gov/ omim/. 2. Parsa CF, Silva ED, Sundin OH, et al. Redefining papillorenal syndrome: An underdiagnosed cause of ocular and renal morbidity. Ophthalmology 2001; 108: 738^ 9. 3. Parsa CF, Cheeseman EW Jr, Maumenee IH. Demonstration of the exclusive cilioretinal vascular system supply the retina in man: Vacant discs. Trans Am Ophthalmol Soc 1998; 96: 95- 106; discussion 106- 9. 4. Chung GW, Edwards AO, Schimmenti LA, et al. Renal- coloboma syndrome: Report of a novel PAX2 gene mutation. Am J Ophthalmol 2001; 132: 910- 14. 5. Schimmenti LA, Cunliffe HE, McNoe LA, et al. Further delineation of renal- coloboma syndrome in patients with extreme variability of phenotype and identical PAX2 mutations. Am J Hum Genet 1997; 60: 869- 78. 211 [KBDpapillorenalsyndrome] |