| Title |
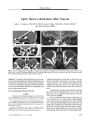
Cerivicocranial Arterial Dissections |
| Creator |
Caplan, LR; Biousse, V |
| Affiliation |
Department of Neurology (LRC), Harvard Medical School, Boston, Massachusetts 02215, USA. lcaplan@caregroup.harvard.edu |
| Abstract |
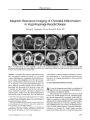
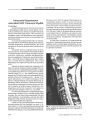
Cervicocranial dissections are an increasingly recognized cause of stroke in the young. When the dissections narrow the vascular lumen, they often alter blood flow enough to cause transient ischemic attacks in the brain. Alterations in the endothelium activate the coagulation cascade, leading to the formation of intramural clot that may embolize distally to cause brain infarction. Pain and neuro-ophthalmic symptoms and signs are common manifestations. |
| Subject |
Carotid Artery, Internal/pathology; Carotid Artery, Internal, Dissection/pathology; Carotid Artery, Internal, Dissection/physiopathology; Carotid Artery, Internal, Dissection/therapy; Humans; Magnetic Resonance Angiography/methods; Vertebral Artery/pathology; Vertebral Artery Dissection/pathology; Vertebral Artery Dissection/physiopathology; Vertebral Artery Dissection/therapy |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225334 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6xq0b1q/225334 |