| Title |
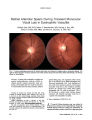
Restricted diffusion in the optic nerve and retina demonstrated by MRI in rhino-orbital mucormycosis. |
| Creator |
Hatipoglu, Hatice Gul; Gurbuz, Muge Onbasioglu; Yuksel, Enis |
| Affiliation |
Department of Radiology, Ankara Numune Education and Research Hospital, Ankara, Turkey. |
| Abstract |
A 29-year-old man developed vision loss in the right eye due to ophthalmic artery, cavernous sinus, and superior ophthalmic vein occlusion in mucormycosis. Diffusion MRI obtained within 2 days of symptom onset showed that the apparent diffusion coefficient values of the optic nerve and retina were remarkably decreased on the affected compared with the unaffected side. A follow-up MRI study 21 days after symptom onset revealed the anticipated disappearance of these signal changes, confirming that they were a true reflection of ischemia in the optic nerve and retina. This report adds to an accumulating body of literature on restricted diffusion in these tissues in conditions producing severe ischemia. |
| Subject |
Adult; Blindness; Cavernous Sinus Thrombosis; Diffusion Magnetic Resonance Imaging; Eye Infections, Fungal; Fatal Outcome; Humans; Male; Mucormycosis; Optic Nerve; Orbital Cellulitis; Paranasal Sinus Diseases; Retina |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225819 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6tt7x2z/225819 |