| Title |
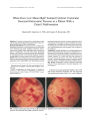
Optic Neuropathy and Central Retinal Artery Occlusion in Non-Hodgkin Lymphoma |
| Creator |
Fierz, AB; Sartoretti, S; Thoelen, AM |
| Affiliation |
Department of Ophthalmology, University Hospital, Zurich, Switzerland. |
| Abstract |
We report a patient with systemic large cell non-Hodgkin lymphoma in remission who presented with the rare combination of optic neuropathy and central retinal artery occlusion. Another unusual feature of this case is the lack of enhancement in the affected region on magnetic resonance imaging only hours after the first dose of steroids. Despite prompt treatment with steroids and radiotherapy, lymphomatous infiltration of the meninges developed 2 months later and was ultimately fatal. |
| Subject |
Older people; Blindness/diagnosis/etiology; Brain Neoplasms/complications/diagnosis; Eye Neoplasms/complications/diagnosis; Fatal Outcome; Female; Fluorescein Angiography; Humans; Lymphoma, Large B-Cell, Diffuse/complications/diagnosis; Magnetic Resonance Imaging; Optic Nerve Diseases/diagnosis/etiology; Papilledema/diagnosis/etiology; Retinal Artery Occlusion/diagnosis/etiology |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225221 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6q55vrv/225221 |