| Title |
When Does Low Mean High |
| Creator |
Lancione, RR Jr; Kosmorsky, GS |
| Affiliation |
Cole Eye Institute, Cleveland Clinic Foundation, Ohio, USA. |
| Abstract |
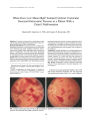
OBJECTIVE: To present an unusual case of pseudotumor cerebri with increased intracranial pressure isolated to the cerebral ventricles resulting from a Chiari I malformation. MATERIALS AND METHODS: The patient received a complete ophthalmologic examination on initial presentation and subsequent visits, including visual acuity, pupillary examination, intraocular pressures, dilated fundus examination with assessment of degree of papilledema, and visual field testing. Intracranial pressure was measured by lumbar puncture and subsequently by intracranial pressure bolt monitoring. Magnetic resonance imaging (MRI) was used to diagnose the Chiari I malformation. RESULTS: The patient initially presented with bitemporal headaches, elevated opening pressure on lumbar puncture, and mild papilledema with a normal MRI. After lumboperitoneal shunt placement and several revisions, the patient presented with decreased vision OD secondary to Terson syndrome and worsening papilledema. Subsequent evaluation revealed normal lumbar opening pressures and a Chiari I malformation. She underwent ventriculoperitoneal shunt placement with resolution of her symptoms. CONCLUSIONS: Tonsillar herniation is a well-documented complication of lumboperitoneal shunt revision. Obstruction of cerebrospinal flow through the foramina of Magendie and Luschka can result in increased intracranial pressure isolated to the cerebral ventricles. In a patient with signs and symptoms of increased intracranial pressure but normal lumbar opening pressure, a Chiari I malformation should be suspected, particularly with a history of multiple lumboperitoneal shunt revisions. |
| Subject |
Adult; Arnold-Chiari Malformation/complications/diagnosis/surgery; Cerebral Ventricles/pathology; Female; Fundus Oculi; Humans; Intracranial Pressure; Intraocular Pressure; Magnetic Resonance Imaging; Papilledema/diagnosis/etiology/physiopathology; Pseudotumor Cerebri/diagnosis/etiology/surgery; Reoperation; Ventriculoperitoneal Shunt; Visual Acuity; Visual Fields |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225225 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6q55vrv/225225 |