| Title |
Acute Retrobulbar Optic Neuritis and Macular Detachment Associated With Morning Glory Optic Disc Anomaly |
| Creator |
Murphy, Marjorie A; Janigian, Robert H; Filippopoulos, Theodoros; Tung, Glenn A |
| Affiliation |
Departments of Ophthalmology and Diagnostic Imaging (GAT), The Warren Alpert Medical School of Brown University |
| Abstract |
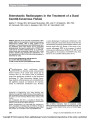
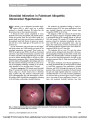
A 31-year-old woman with morning glory optic disc anomaly (MGDA) developed acute retrobulbar optic neuritis and a bullous macular detachment. MRI demonstrated truncation of the perineural space of the affected optic nerve as well as focal optic nerve enhancement. Optical coherence tomography (OCT) showed retinoschisis associated with the macular detachment. The MRI and OCT findings support the vitreous as the source of the subretinal fluid. This is the first reported case of optic neuritis in MGDA. |
| Subject |
Acute Disease; Adult; Disease Progression; Female; Humans; Macula Lutea/pathology; Macula Lutea/physiopathology; Magnetic Resonance Imaging; Methylprednisolone/therapeutic use; Optic Disk/abnormalities; Optic Disk/physiopathology; Optic Nerve/pathology; Optic Nerve/physiopathology; Optic Nerve Diseases/complications; Optic Nerve Diseases/pathology; Optic Nerve Diseases/physiopathology; Optic Neuritis/etiology; Optic Neuritis/pathology; Optic Neuritis/physiopathology; Peripheral Nerves/pathology; Peripheral Nerves/physiopathology; Retina/pathology; Retina/physiopathology; Retinal Detachment/etiology; Retinal Detachment/pathology; Retinal Detachment/physiopathology; Tomography, Optical Coherence; Vitreous Body/pathology; Vitreous Body/physiopathology |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
227055 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6k109bb/227055 |