| OCR Text |
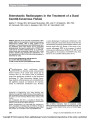
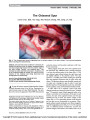
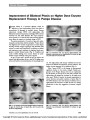
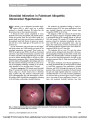
Show Choroidal Infarction in Fulminant Idiopathic Intracranial Hypertension We describe a case of idiopathic intracranial hyper-tension (IIH) in which visual loss is partially attributed to choroidal infarction. We believe that this phenomenon has not been reported previously. A 20-year-old white woman complained of severe headaches with nausea, photophobia, and pulsatile tinnitus. During the previous week, she had noticed rapidly pro-gressive visual loss in both eyes with severe constriction of her peripheral visual field. Review of systems was remark-able only for a recent weight gain of 20 pounds over the previous year. On our examination, body mass index was 26.6 kg/m2 and blood pressure was 110/68 mmHg, and results of the neurologic examination were normal. Visual acuity was 20/20 in the right eye and 20/30 in the left eye. Automated and kinetic visual fields showed bilateral constriction with an inferior nasal defect and enlarged blind spot in the right eye and an inferior altitudinal defect in the left eye. Oph-thalmoscopic examination (Fig. 1) showed bilateral severe optic disc edema with peripapillary hemorrhages and nerve fiber layer ischemic whitening. In the left eye, there was an area of juxtapapillary whitening extending to the macula, which appeared to be in the deep retina or choroid. Fluorescein angiography (FA) showed normal choroidal filling 25 seconds after injection and normal retinal per-fusion, ruling out a branch retinal artery or cilioretinal artery occlusion (Fig. 2A). However, indocyanine green (ICG) videoangiography (Fig. 2B) demonstrated a choroi-dal perfusion defect matching the juxtapapillary whitening in the left fundus, confirming a choroidal infarction. We attributed the ophthalmic findings to raised in-tracranial pressure (ICP) with severe papilledema in both eyes, choroidal infarction, and anterior ischemic optic neuropathy (AION) in the left eye. The diagnosis of IIH was confirmed by normal brain MRI and magnetic resonance venography (MRV) and by a cerebrospinal fluid (CSF) opening pressure of 560 mm H2O with normal CSF contents (1). A diagnostic lumbar puncture relieved her headaches immediately, and treat-ment with 500 mg oral acetazolamide twice a day was begun. Her visual function, however, remained poor, and she underwent bilateral sequential optic nerve sheath fen-estrations (ONSFs) 8 and 21 days later. The headaches did not recur. The optic disc edema resolved, and she developed optic disc pallor in both eyes. The juxtapapillary whitening resolved within 2 weeks of the ONSFs. The altitudinal defect remained unchanged in the left eye, and the visual field improved in the right eye but remained constricted (Fig. 3). Final visual acuity was 20/20 in both eyes. Our patient developed severe bilateral papilledema in the setting of fulminant IIH (2) and had visual loss related to visual field constriction from papilledema, choroidal infarction, and AION. Although the anatomy of the short posterior ciliary arteries that vascularize the choroid around the optic disc might logically explain the occurrence of a choroidal infarction in acute and prominent papilledema, we could not find any previous report of such a complica-tion in the setting of severe papilledema. However, 5 pa-tients with presumed choroidal infarction have been FIG. 1. Bilateral optic disc edema with papillary cotton wool spots. In the left eye, there is an area of whitening extending to the macula and located deep to the retina. Lamirel et al: J Neuro-Ophthalmol 2010; 30: 167-168 167 Clinical Observation Copyright © North American Neuro-ophthalmology Society.Unauthorized reproduction of this article is prohibited. reported previously as a complication of ONSF performed for papilledema (3-6). Immediate recognition of the mechanism of visual loss in patients with papilledema is essential in making appropriate therapeutic decisions. Choroidal infarction should be added to the list of rare complications of severe papilledema. Ce´dric Lamirel, MD Beau B. Bruce, MD Nancy Newman, MD Vale´rie Biousse, MD Departments of Ophthalmology and Neurology Emory University School of Medicine Atlanta, Georgia Departments of Ophthalmology, Neurology, and Neurological Surgery Emory University School of Medicine Atlanta, Georgia vbiouss@emory.edu REFERENCES 1. Friedman DI, Jacobson DM. Diagnostic criteria for idiopathic intracranial hypertension. Neurology. 2002;59:1492-1495. 2. Thambisetty M, Lavin PJ, Newman NJ, Biousse V. Fulminant idiopathic intracranial hypertension. Neurology. 2007;68: 229-232. 3. Knight RS, Fielder AR, Firth JL. Benign intracranial hypertension: visual loss and optic nerve sheath fenestration. J Neurol Neurosurg Psychiatry. 1986;49: 243-250. 4. Plotnik JL, Kosmorsky GS. Operative complications of optic nerve sheath decompression. Ophthalmology. 1993;100: 683-690. 5. Rizzo JF 3rd Lessell S. Choroidal infarction after optic nerve sheath fenestration. Ophthalmology. 1994;101:1622-1626. 6. Spoor TC, Ramocki JM, Madion MP, Wilkinson MJ. Treatment of pseudotumor cerebri by primary and secondary optic nerve sheath decompression. Am J Ophthalmol. 1991;112: 177-185. FIG. 2. A. Fluorescein angiography of the left eye 25 seconds after injection of fluorescein shows normal retinal vascular filling (earlier transit times were not available and choroidal filling could therefore not be evaluated). B. Indocyanine green angiography of the left eye shows a choroidal filling defect matching the area of whitening seen on the fundus examination. FIG. 3. Automated visual fields (24-2 SITA Fast) per-formed after left optic nerve sheath fenestration show, in the left eye, an inferior nerve fiber bundle defect attrib-uted to ischemic optic neuropathy and a paracentral nasal defect above fixation attributed to choroidal infarction. Clinical Observation 168 Lamirel et al: J Neuro-Ophthalmol 2010; 30: 167-168 Copyright © North American Neuro-ophthalmology Society.Unauthorized reproduction of this article is prohibited. |