| Title |
Radiosensitive Orbital Inflammation Associated with Temporal Arteritis |
| Creator |
Cockerham, KP; Cockerham, GC; Brown, HG; Hidayat, AA |
| Affiliation |
Allegheny Ophthalmic and Orbital Associates, 420 East North Avenue, Suite 116, Pittsburgh, PA 15212, USA. kpcorb@aol.com |
| Abstract |
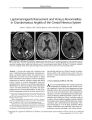
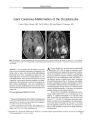
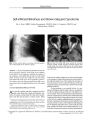
A 75-year-old woman developed acute loss of vision in the OD, ipsilateral periocular pain, an afferent pupillary defect, sectoral optic disc edema, and later ipsilateral proptosis and an intraconal mass. She denied any symptoms of temporal arteritis, and a sedimentation rate was normal. Orbital biopsy demonstrated chronic granulomatous inflammation with perivasculitis. A temporal artery biopsy disclosed findings consistent with temporal arteritis. Following 2000 cGy of external beam radiation, her visual function and orbitopathy completely resolved. This unusual presentation of orbital inflammation in association with temporal arteritis demonstrates that pathologic findings of temporal arteritis may be clinically nonspecific and that external beam radiation may be an effective therapy in this setting. |
| Subject |
Older people; Female; Giant Cell Arteritis/complications; Giant Cell Arteritis/pathology; Giant Cell Arteritis/radiotherapy; Humans; Inflammation/etiology; Inflammation/pathology; Inflammation/physiopathology; Inflammation/radiography; Orbital Diseases/etiology; Orbital Diseases/pathology; Orbital Diseases/physiopathology; Orbital Diseases/radiography; Temporal Arteries/pathology; Tomography, X-Ray Computed; Treatment Outcome; Visual Acuity; Visual Fields |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225151 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s63f7vpw/225151 |