| Title |
Progressive Visual Loss Because of a Suprasellar Pneumatocele After Trans-sphenoidal Resection of a Pituitary Adenoma |
| Creator |
Lee, AG; Van Gilder, JC; White, ML |
| Affiliation |
Departments of Ophthalmology, University of Iowa Hospitals and Clinics, Iowa City, Iowa 52242, USA. andrew-lee@uiowa.edu |
| Abstract |
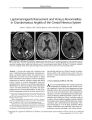
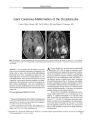
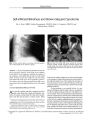
A 63-year-old man who underwent uneventful trans-sphenoidal resection of a pituitary adenoma with fat packing complained postoperatively of progressive binocular visual acuity loss. Neuroimaging showed a suprasellar pneumatocele compressing the optic chiasm and a communication between the sphenoid sinus and the sella. After a second trans-sphenoidal procedure to remove the air and fully pack the sphenoid sinus, visual acuity recovered dramatically. A rare complication of trans-sphenoidal surgery for pituitary adenoma, suprasellar pneumatocele probably forms through a ball-valve mechanism that results from incomplete packing of the sellar floor. This case highlights the need for effective sphenoid sinus packing and for ophthalmic monitoring after trans-sphenoidal surgery. |
| Subject |
Adenoma/surgery; Disease Progression; Humans; Magnetic Resonance Imaging; Male; Middle Older people; Neurosurgical Procedures/adverse effects; Pituitary Neoplasms/surgery; Pneumocephalus/complications; Pneumocephalus/diagnosis; Pneumocephalus/etiology; Pneumocephalus/surgery; Reoperation; Sella Turcica; Sphenoid Sinus/surgery; Tomography, X-Ray Computed; Vision Disorders/etiology; Vision Disorders/physiopathology; Visual Fields |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225156 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s63f7vpw/225156 |