| Title |
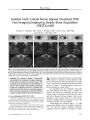
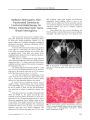
Imaging Nuances of Perineural Spread of Head and Neck Malignancies |
| Creator |
Ibrahim, M; Parmar, H; Gandhi, D; Mukherji, SK |
| Affiliation |
Department of Radiology, Division of Neuroradiology, University of Michigan Health System, Ann Arbor, Michigan, USA. |
| Abstract |
Perineural spread is a common growth pattern of head and neck malignancies. Recognizing this pattern by imaging is important for two reasons: 1) it may be the only evidence of malignancy; and 2) its presence in conjunction with a mass converts management from surgical resection to radiation or chemotherapy. High field strength magnets and thin sections with high resolution and fat suppression now allow earlier diagnosis of this entity, but even with these imaging developments, familiarity with the relevant anatomy and the subtle alterations on MRI are necessary to identify this condition. |
| Subject |
Cranial Nerve Neoplasms, pathology; Facial Nerve Diseases, pathology; Head and Neck Neoplasms, pathology; Humans; Magnetic Resonance Imaging, methods; Trigeminal Nerve Diseases, pathology |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225652 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s60k5fn5/225652 |