| Title |
Idiopathic Hypertrophic Pachymeningitis Mimicking Lymphoplasmacyte-Rich Meningioma |
| Creator |
Hosler, MR; Turbin, RE; Cho, ES; Wolansky, LJ; Frohman, LP |
| Affiliation |
Department of Ophthalmology and Visual Science, New Jersey Medical School, Newark, New Jersey 07103, USA. |
| Abstract |
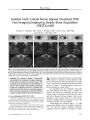
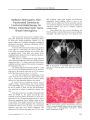
A 28-year-old woman with a 6-year history of optic neuropathy and 8 years of hearing loss had enhancing dural lesions around the brain stem and in both internal auditory canals on MRI. Histopathology from cranial procedures performed in 1990 and 1993 was originally interpreted as inflammatory meningioma, now known as lymphoplasmacyte-rich meningioma (LRM). Because the clinical course was more consistent with a relapsing process, the original surgical specimens were restudied with additional immunocytochemical stains. The review led to a pathologic diagnosis of idiopathic hypertrophic pachymeningitis (IHP). IHP and LRM can be confused on both imaging and histopathologic grounds. |
| Subject |
Adult; Diagnosis, Differential; Dura Mater, pathology; Female; Humans; Hypertrophy; Magnetic Resonance Imaging; Meningeal Neoplasms, diagnosis; Meningioma, diagnosis; Meningitis, diagnosis; Plasma Cells, pathology |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225643 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s60k5fn5/225643 |