| Title |
Isolated Bilateral Internuclear Ophthalmoplegia After Ischemic Stroke |
| Creator |
de Andrade, DC; Lucato, LT; Yamamoto, FI; Marchiori, PE; Scaff, M; Conforto, AB |
| Affiliation |
Department of Neurology, University of São Paulo, São Paulo, Brazil. ciampi@terra.com.br |
| Abstract |
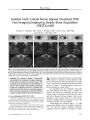
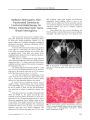
A 63-year-old man suddenly developed an isolated bilateral internuclear ophthalmoplegia (INO). High-resolution brain MRI showed signal abnormalities consistent with acute ischemic stroke limited to the infra-aqueductal region of the midbrain bilaterally. This case offers graphic evidence that stroke can be responsible for an isolated bilateral INO. |
| Subject |
Cerebral Aqueduct, pathology; Humans; Magnetic Resonance Imaging, methods; Male; Middle Older people; Ocular Motility Disorders, etiology; Ocular Motility Disorders, pathology; Stroke, complications; Stroke, pathology |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225650 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s60k5fn5/225650 |