| Title |
Transient Ocular Motor Nerve Palsies Associated With Presumed Cranial Nerve Schwannomas |
| Creator |
Robert K. Shin; Luis J. Mejico; Aki Kawasaki; Valerie A. Purvin; Mark L. Moster; Brian R. Younge; Dan Boghen |
| Affiliation |
Departments of Neurology and Ophthalmology & Visual Sciences (RKS), University of Maryland School of Medicine, Baltimore, Maryland; Departments of Neurology and Ophthalmology (LJM), SUNY Upstate Medical University, Syracuse, New York; Department of Ophthalmology (AK), University of Lausanne, Hpital Ophtalmique Jules Gonin and Asile des Aveugles, Lausanne, Switzerland; Departments of Ophthalmology and Neurology (VAP), Indiana University Medical Center, Indianapolis, Indiana; Departments of Neurology and Ophthalmology (MLM), Thomas Jefferson University School of Medicine, Philadelphia, Pennsylvania; Department of Neuro-Ophthalmology (MLM), Wills Eye Hospital, Philadelphia, Pennsylvania; and Dpartement de Neurosciences (DB), Universit de Montral, Centre Hospitalier de lUniversit de Montral, Montral, Qubec, Canada |
| Abstract |
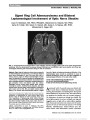
BACKGROUND: Cranial nerve schwannomas are radiologically characterized by nodular cranial nerve enhancement on magnetic resonance imaging (MRI). Schwannomas typically present with gradually progressive symptoms, but isolated reports have suggested that schwannomas may cause fluctuating symptoms as well. METHODS: This is a report of ten cases of presumed cranial nerve schwannoma that presented with transient or recurring ocular motor nerve deficits. RESULTS: Schwannomas of the third, fourth, and fifth nerves resulted in fluctuating deficits of all 3 ocular motor nerves. Persistent nodular cranial nerve enhancement was present on sequential MRI studies. Several episodes of transient oculomotor (III) deficts were associated with headaches, mimicking ophthalmoplegic migraine. CONCLUSIONS: Cranial nerve schwannomas may result in relapsing and remitting cranial nerve symptoms. |
| Subject |
Adult; Older people; Cranial Nerve Neoplasms; Female; Humans; Magnetic Resonance Imaging; Male; Middle Older people; Neurilemmoma; Oculomotor Nerve Diseases; Young Adult |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
227708 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s66b08p3/227708 |