| Title |
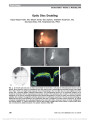
Cat Scratch Neuroretinitis: The Role of Acute and Convalescent Titers for Diagnosis |
| Creator |
Gulati, Archit; Yalamanchili, Sushma; Golnik, Karl C; Lee, Andrew G |
| Affiliation |
Department of Ophthalmology, The Methodist Hospital (AGL), Houston, Texas Departments of Ophthalmology, Neurology, and Neurosurgery, Weill Cornell Medical College (AGL, SY), New York, New York Department of Ophthalmology, University of Iowa Hospitals and Clinics (AGL), Iowa City, Iowa Department of Ophthalmology, University of Texas Medical Branch (AGL), Galveston, Texas Baylor College of Medicine (AG, AGL) Department of Ophthalmology, University of Cincinnati (KCG), Cincinnati, Ohio |
| Abstract |
Cat scratch neuroretinitis (CSN) is a clinical diagnosis supported by serological testing. We present 2 cases of CSN in which initial acute titers were negative or equivocal for Bartonella henselae while convalescent titers were shown to be positive. We report these cases to emphasize that a single acute negative titer is insufficient to exclude the diagnosis of CSN and that convalescent titers should be obtained in patients for whom there is a high clinical suspicion of the disease. |
| Subject |
Adult; Anti-Bacterial Agents; Azithromycin; Bartonella henselae; Cat-Scratch Disease; Child; Female; Humans; Immunoglobulin G; Magnetic Resonance Imaging; Male; Retinitis |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
227326 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s61v8m1c/227326 |