| Title |
Unilateral Ophthalmoplegia Secondary to Anterior Clinoid Process Mucocele |
| Creator |
Forer, Boaz; Hui, Ng Yuk; Sethi, Dharmbir Singh |
| Affiliation |
Department of Otolaryngology Head and Neck Surgery, Singapore General Hospital |
| Abstract |
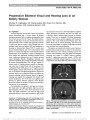
A 50-year-old Chinese man presented with rapidly progressive unilateral ophthalmoplegia and then an ipsilateral afferent pupil defect. CT and MRI revealed a mass centered in the anterior clinoid process causing bone destruction and showing high T1 and T2 signal intensity indicative of mucosal protein secretion. These imaging features suggested a mucocele, which may have resulted from sequestration of a clinoidal extension of the sphenoid sinus. The sphenoid sinus was opened via an image-guided endoscopic approach, and the lesion incised. There were no complications. The ophthalmoplegia and afferent pupil defect had completely resolved within 1 week of surgery. This is the eighth reported case of anterior clinoidal mucocele, a rare cause of ophthalmoplegia or optic neuropathy. Advances in endoscopic instrumentation, navigation systems, and intraoperative imaging have reduced the operative risk and made the endoscopic approach a feasible and safer alternative to open surgery for this condition. |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
227108 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s69g8sxs/227108 |