| OCR Text |
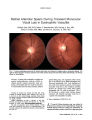
Show ORIGINAL CONTRIBUTION Temporary Adduction Deficit After Nasal Septoplasty and Radiofrequency Ablation of the Inferior Turbinate Saeid Atighechi, MD, S. Hossein Alimohammadi, MD, Mohammad Hossein Baradaranfar, MD, and S. Abbas Mirvakili, MD Abstract: A 19-year-old boy developed an adduc-tion deficit after bilateral radiofrequency ablation of the inferior turbinate and septoplasty. Postoperative imaging disclosed an intact medial orbital wall and high T2 signal and enlargement of the medial rectus. Within 3 months, the motility deficit had resolved. This manifestation is attributed to injury of the medial rectus from radiofrequency ablation and represents the first reported case. (J Neuro-Ophthalmol 2009;29:29-32) Septoplasty and radiofrequency ablation of the inferior turbinate are common procedures in the management of patients with nasal obstruction due to septal deviation and hypertrophy of the inferior turbinate (1). Ophthalmic complications of these procedures are rare (2-7). We report a patient with temporary postoperative diplopia due to medial rectus paresis. CASE REPORT A 19-year-old boy had symptoms of nasal obstruc-tion owing to septal deviation and bilateral hypertrophy of the inferior turbinate and reduced air flow, especially on the right (Fig. 1). Septoplasty was performed under general anesthesia with a hemi-transfix incision on the left side of the nasal septum. When the procedure was finished, the muco-perichondrial flap was completely intact. With a bipolar radiofrequency probe at 10-watt power, the inferior turbinate was treated under standard protocol. No intra-operative complications were noted. Upon awakening from Department of Otolaryngology Yazd University of Medical Sciences, Shahid Sadughi Hospital, Yazd, Iran. Address correspondence to Saeid Atighechi, MD, Department of Otolaryngology, Head and Neck Surgery, Yazd University of Medical Sciences, Shahid Sadughi Hospital, Ibn-e-sina Street, Yazd, Iran; E-mail: saeidatighechi@yahoo.com anesthesia, the patient reported diplopia. Limited adduction of the right eye and swelling of the inferior right eyelid were noted (Fig. 2). Ophthalmologic consultation disclosed a visual acu-ity of 20/20 bilaterally, confirmed the ocular motility and eyelid findings, and found normal pupillary function and direct ophthalmoscopy. Postoperative CT with 2-mm thickness and 3-mm intervals and MRI of the orbit and brain with 3-mm sections were performed on the second and third postoperative days, respectively. They did not disclose any abnormalities except edema of the right orbit, inflammation in the right anterior ethmoid cells, and high-intensity T2 MRI signal and enlargement of the right medial rectus. The medial wall of the orbit was intact (Figs. 3 and 4). The patient was treated with 1 mg/kg/day prednis-olone orally. On the fourth postoperative day, swelling of the eyelid was improved, and diplopia in primary gaze position was minimally improved. The patient was discharged with a tapering schedule of oral prednisolone. Within 3 months of surgery, ocular motility had returned to normal (Fig. 5). FIG. 1. Preoperative precontrast coronal CT shows right-ward septal deviation and hypertrophy of the inferior turbinates. J Neuro-Ophthalmol, Vol. 29, No. 1, 2009 29 J Neuro-Ophthalmol, Vol. 29, No. 1, 2009 Atighechi et al FIG. 2. Our patient's ocular motility on the first postoperative day shows a right exodeviation and a complete right adduction deficit. Top, primary position; middle, right gaze; bottom, left gaze. DISCUSSION Our patient had temporary dysfunction of the medial rectus after standard nasal septoplasty and radiofrequency ablation of the inferior turbinate. The anatomic proximity of the orbit to the adjacent sinus and nose exposes the orbital contents to trauma in sinus and nose surgery (2-7). Huang et al (8) divided injury to the medial rectus into four patterns, particularly with reference to the degree of direct injury (mainly the degree of muscle tissue loss). Pattern I was applied to muscle transection, pattern II to partial muscle transection, pattern III to a contused, entrapped muscle, and pattern IV to a contused muscle without entrapment. Our patient fits pattern IV, but unlike the patients of Huang et al (8), the orbital wall in our patient was intact. Two patients with ocular motility disorders without orbital wall damage have been previously reported (6,9). Kosko et al (6) described a patient with unilateral partial third nerve palsy after bilateral sinus surgery. The diplopia and anisocoria resolved 2 months after the surgery. They suggested that this complication resulted from postopera-tive edema (6). Bayramlar et al (9) reported temporary hypertropia, supraduction deficit, ipsilateral mydriasis, and accommodative paresis after bilateral endoscopic ethmoidec-tomy, bilateral partial inferior turbinectomy, and septoplasty FIG. 3. Precontrast axial CT performed on the second postoperative day shows an intact right lamina papyracea and continuity of the right medial rectus. There are postoper-ative changes within the right anterior ethmoid air cells. 30 q 2009 Lippincott Williams & Wilkins Adduction Deficit After Nasal Septoplasty J Neuro-Ophthalmol, Vol. 29, No. 1, 2009 FIG. 4. Axial T2 MRI performed on the third postoperative day shows enlargement and high signal within the right medial rectus. but without radiofrequency ablation in a Caldwell-Luc approach for chronic sinusitis. In their patient, all of these manifestations resolved within 2 months (9). The medial rectus dysfunction in our patient probably resulted from the radiofrequency ablation. In their review of 1,600 patients who underwent percutaneous radiofrequency trigeminal rhizotomy, Kanpolat et al (10) noted transient sixth cranial nerve palsy in 11 patients and transient third cranial nerve palsy in 2 patients. Two patients had permanent sixth cranial nerve palsy. The proposed mechanisms of the side effects or complications of percutaneous radiofrequency rhizotomy are mislocation of the electrode and spread of thermal energy to neighboring neural structures (11). We have encountered FIG. 5. Three months after surgery, the patient has full ocular ductions and normal ocular alignment. 31 J Neuro-Ophthalmol, Vol. 29, No. 1, 2009 Atighechi et al no previous reports of similar injury to the medial rectus or any other extraocular muscle after radiofrequency ablation in nasal or sinus surgery. There is one report (12) of irreversible blindness in one eye and impairment of the infratemporal visual field in the other eye after electro-coagulation performed for delayed bleeding after functional endoscopic sinus surgery. These complications were attributed to expansion of thermal energy to neighboring neural structures. Postoperative imaging in our patient did not demonstrate orbital or intracranial abnormalities except edema of the medial rectus muscle and anterior ethmoid air cells. In such circumstances, the patient can be reassured that the deficits are transient and that complete recovery may be anticipated within months. REFERENCES 1. Joe S, Benson A. Nonallergic rhinitis. In: Cummings CW, Flint PW, Harker LA, et al., eds. Cummings otolaryngology, head and neck surgery. 4th ed. Philadelphia: Elsevier Mosby; 2005:998. 2. Buus DR, Tse DT, Farris BK. Ophthalmic complications of sinus surgery. Ophthalmology 1990;97:612-9. 3. Pelletier CR, Jordan DR, Grahovac SZ. Inferior rectus entrapment following Caldwell-Luc surgery associated with an unrecognized hypoplastic maxillary antrum. Can J Ophthalmol 1997;32:189-92. 4. Blackwell KE, Goldberg RA, Calcaterra TC. Atelectasis of the maxillary sinus with enophthalmos and midface depression. Ann Otol Rhinol Laryngol 1993;102:429-32. 5. Steward D, Simpson GT, Nader ND. Postoperative anisocoria in a patient undergoing endoscopic sinus surgery. Reg Anesth Pain Med 1999;24:467-9. 6. Kosko JR, Prat MF, Chames M, et al. Anisocoria: a rare consequence of endoscopic sinus surgery. Otolaryngol Head Neck Surg 1998;118: 242-244. 7. Eitzen JP, Elsas FJ. Strabismus following endoscopic intranasal sinus surgery. J Pediatr Ophthalmol Strabismus 1991;28:168-70. 8. Huang CM, Meyer DR, Patrinely JR, et al. Medial rectus muscle injuries associated with functional endoscopic sinus surgery: charac-terization and management. Ophthal Plast Reconstr Surg 2003;19: 25-37. 9. Bayramlar H, Miman MC, Demirel S. Inferior oblique paresis, mydriasis, and accommodative palsy as temporary complications of sinus surgery. J Neuroophthalmol 2004;24:225-7. 10. Kanpolat Y, Savas A, Bekar A, et al. Trigeminal rhizotomy for the treatment of idiopathic trigeminal neuralgia: 25-year experience with 1,600 patients. Neurosurgery 2001;48:524-32. 11. Bhatti MT, Patel R. Neuro-ophthalmic considerations in trigeminal neuralgia and its surgical treatment. Curr Opin Ophthalmol 2005;16: 334-40. 12. Vanden Abeele D, Clemens A, Tassignon MJ, et al. Blindness due to electrocoagulation following functional endoscopic sinus surgery. J Laryngol Otol 1996;110:261-264. 32 q 2009 Lippincott Williams & Wilkins |