| OCR Text |
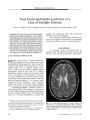
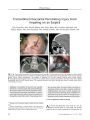
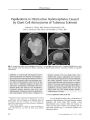
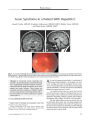
Show ORIGINAL CONTRIBUTION Wall- Eyed Bilateral Internuclear Ophthalmoplegia From Lesions at Different Levels in the Brainstem Chien- Ming Chen, MD and Sung- Hsiung Lin, MD Abstract: Wall- eyed bilateral internuclear ophthalmoplegia ( WEBINO) is a rarely reported syndrome. There is dispute about whether WEBINO is caused by a pontine or a midbrain lesion and whether the medial rectus subnuclei are implicated. In a study of the clinical and imaging features of four patients with WEBINO, we found that that three of four lesions involved the midbrain but not necessarily the medial rectus subnuclei. ( J Neuro- Ophthalmol 2007; 27: 9- 15) all- eyed bilateral internuclear ophthalmoplegia ( WEBINO) is a rarely reported syndrome named by Lubow in 1971 ( 1) to describe patients with bilateral adduction deficits and exotropia in primary gaze position. WEBINO is thought to be caused by a lesion in the midbrain involving the medial rectus subnuclei as well as the medial longitudinal fasciculus ( MLF) bilaterally. The postulated involvement of the medial rectus subnuclei is believed to be necessary to account for the exotropia, in as much as in bilateral internuclear ophthalmoplegia ( INO) alone, the eyes are generally aligned in primary gaze position. Several authors have argued against implicating the medial rectus subnuclei in WEBINO. For example, Moncayo and Bogousslavsky ( 2) classify WEBINO as a pontine rather than a midbrain stroke. Others maintain that it is impossible to exclude the involvement of the medial rectus subnuclei in the WEBINO syndrome ( 3). We present four cases of WEBINO caused by lesions at different levels in the brainstem. We discovered midbrain involvement in three cases, but in those cases, the medial rectus subnuclei were not necessarily affected. Section of Neurology, Department of Internal Medicine ( CMC) and Department of Ophthalmology ( SHL), Feng Yuan Hospital, Department of Health, Executive Yuan, Taiwan, Republic of China. Address correspondence to Chien- Ming Chen, MD, Department of Internal Medicine, Feng Yuan Hospital, Department of Health, Executive Yuan, 100, An- Kan Rd, Feng Yuan, Taichung, Taiwan, ROC; E- mail: jmchen@ mail. fyh. doh. gov. tw CASE REPORTS Case 1 A 66- year- old man with a 3 year history of systemic hypertension and diabetes mellitus presented with dizziness, unsteadiness, and double vision that had begun 2 days earlier. General physical and neurologic examinations were normal except for ocular motility. In primary gaze position, both eyes were exodeviated, with the left eye being more so. On horizontal gaze, the abducting eye deviated fully, but the adducting eye did not cross the midline. Downgaze was intact, but upgaze and convergence were impaired. Pupils measured 4 mm in dim illumination and constricted normally to direct light. There was no ptosis ( Fig. 1). Brain MRI performed 4 days later disclosed a slit- like T2 hyperintense lesion in the paramedian midbrain that extended from the aqueduct dorsally almost to the interpeduncular cistern ventially ( Fig. 2A, B). The cause was presumed to be an infarct. His dizziness and unsteadiness soon subsided. Eight weeks later, the upgaze impairment, exotropia, and left adduction deficit had disappeared. MRI performed 4 months after the onset, when the only clinical deficits were absent right adduction and convergence, showed that the lesion had become smaller ( Fig. 2C, D). By 9 months after onset, the convergence deficit was gone, but the right adduction deficit lingered. Case 2 An 84- year- old man with uncontrolled systemic hypertension developed acute mild left hemiparesis. He veered to the left on sitting and standing. No dysmetria was seen on finger- to- nose testing. Ocular motility examination showed mild bilateral exotropia, particularly on attempted upgaze. Bilateral adduction deficits were noted on horizontal gaze, together with nystagmus in the abducting eyes. Downgaze was normal, but upgaze and convergence were defective ( Fig. 3). There was no ptosis and no facial or bulbar palsy, and the plantar responses were flexor bilaterally. Brain MRI performed the following day revealed two hyperintense lesions on FLAIR and diffusion-weighted imaging ( DWI), one at the dorsal pons- midbrain J Neuro- Ophthalmol, Vol. 27, No. 1, 2007 9 J Neuro- Ophthalmol, Vol. 27, No. 1, 2007 Chen and Lin FIG. 1. Case 1: Ocular motility. Bilateral exodeviation is present in primary gaze position. Neither eye adducts on horizontal gaze. Downgaze is intact, but upgaze and convergence ( bottom) are deficient. r Wk. W Mr \ 7 Hi M WU • iVMj ^^^^ - j FIG. 2. Case 1: Brain imaging. T2 axial ( A) and coronal ( B) MRI reveals a paramedian slit- like high signal abnormality almost bisecting the midbrain ( arrow). Four months later, T2 axial ( C) and coronal ( D) MRI, when the patient had only a right internuclear ophthalmoplegia ( INO) and a convergence deficit, shows persistence of the dorsal portion of the lesion near the aqueduct. 10 © 2007 Lippincott Williams & Wilkins WEBINO J Neuro- Ophthalmol, Vol. 27, No. 1, 2007 FIG. 3. Case 2: Ocular motility. The left eye is exodeviated in primary gaze position. There is no adduction of either eye on horizontal gaze. Downgaze is normal, but upgaze and convergence are defective. junction abutting the fourth ventricle and extending into the right paramedian midbrain and the other in the right subcortical region ( Fig. 4). The former lesion accounted for the ocular findings and the latter lesion for the mild left hemiparesis. He was determined to have had an ischemic stroke. Within 2 weeks, he had regained the ability to walk. Within 6 weeks, the left adduction and upgaze deficits and FIG. 4. Case 2: Brain imaging. Axial FLAIR ( A- C), axial diffusion- weighted ( D, E), and T2 coronal ( F) MRI show a hyperintense signal at the dorsal pons- midbrain junction bilaterally that extends to the right paramedian midbrain. There is also an unrelated signal abnormality in the right subcortical region. ; ; J Neuro- Ophthalmol, Vol. 27, No. 1, 2007 Chen and Lin exotropia had disappeared, but the right adduction and convergence deficits persisted. Case 3 A 51- year- old schizophrenic woman suddenly developed vomiting and the inability to walk followed by altered consciousness over a 1 day period. She was stuporous with apparent incomplete right hemiparesis. Plantar responses were flexor bilaterally. When her eyelids were manually elevated, alternating exotropia was noted. Both eyes failed to cross the midline on oculocephalic maneuver ( Fig. 5). Brain CT scanning ( Fig. 6A- C) disclosed an enhancing mass at the pons- midbrain junction with enlargement of the third and lateral ventricles. Ventriculoperitoneal shunting was performed immediately. She gradually recovered consciousness. At 1 month after onset, she was able to cooperate with clinical eye movement testing. In primary gaze position, her left eye was exodeviated. On horizontal gaze, the right eye adducted 50% beyond the midline, and the left eye did not cross the midline. Both eyes abducted normally. A brain CT scan performed immediately after shunting ( Fig. 6D- F) clearly disclosed a mass extending through the midbrain into the third ventricle. An astrocytoma or oligodendroglioma was presumed, but pathologic confirmation was not obtained. Case 4 A 65- year- old diabetic hypertensive woman developed acute dense right hemiplegia. Six weeks earlier, she had sustained a minor stroke with mild hemiplegia and hemisensory loss affecting the left limbs. On our examination, she had a new right upper motor neuron facial palsy and a right extensor plantar response. Bilateral exodeviation of the eyes was noted in primary and downgaze, which was more prominent in the left eye. Neither eye crossed the midline on attempted horizontal gaze, and there was nystagmus in the abducting eye. Upgaze and downgaze were intact, but convergence was impaired ( Fig. 7). Emergency brain CT scanning disclosed a small right periventricular subcortical infarct that had probably occurred 6 weeks earlier. Brain MRI performed 5 days after new stroke onset ( Fig. 8) disclosed a signal abnormality spreading over almost the entire rostrocaudal extent of the left pons, extending beyond the midline in the low to middle pons but sparing the paramedian brainstem rostral to the midpontine level. The neurologic deficits and ocular abnormality persisted. Nine months later, the patient died of hepatic cirrhosis, but no autopsy was obtained. DISCUSSION In our four cases of WEBINO, believed to be the largest with reported series accompanying MRI, three patients showed lesions involving the midbrain ( Cases 1- 3). Even in the three cases that involved the midbrain, the medial rectus subnuclei were not clearly involved. Previous attempts to define the involvement of the medial rectus subnuclei have had flaws. Before CT brain imaging became available, Gonyea ( 4) located the lesion within the pons in one of three patients with WEBINO because of concurrent left peripheral facial weakness and right arm weakness. But as the patient also had a prominent right medial rectus palsy, the lesion might have extended into the midbrain. Takamatsu and Ohta ( 5) described a patient with an initial left one- and- a- half syndrome ( OHS) and paralytic pontine exotropia ( PPE), evolving into WEBINO and later into right INO. T2 MRI showed high signal intensity lesions in the paramedian portion of the midpontine tegmentum bilaterally. The authors believed that the WEBINO was caused by a pontine lesion and that PPE, OHS, and WEBINO were reflections of the same lesion. However, the left OHS suggests involvement of the left MLF plus either the left paramedian pontine reticular formation ( PPRF) or the left abducens nucleus or both structures ( 6- 8). Contralateral exotropia in PPE is attributed to involvement of the PPRF. The gaze deviation is due to the unopposed tonic activity of the spared PPRF on the side opposite to a unilateral lesion. If both sides of the pons were symmetrically damaged, exotropia would not occur ( 6,8,9). If the lesions seen in the MRI were responsible for the unilateral exotropia of PPE as well as the bilateral exotropia in their case, there would have to be bilateral PPRF involvement. This conclusion is impossible, however, because supranuclear tonic ocular deviation via the PPRF would fail to induce exotropia bilaterally. Strominger et al ( 10) reported a largely preserved oculomotor nucleus in necropsy material of a patient with WEBINO who died of metastatic small cell carcinoma and FIG. 5. Case 3: Ocular motility. In primary gaze, the left eye is exodeviated. On horizontal gaze, the left eye does not cross the midline and the right eye adducts 50%. 12 © 2007 Lippincott Williams & Wilkins WEBINO J Neuro- Ophthalmol, Vol. 27, No. 1, 2007 ELM FIG. 6. Case 3: Brain imaging. Brain CT scanning ( A- C) discloses a pons- midbrain mass obstructing the aqueduct and enlarging the ventricles. Immediately after ventriculoperitoneal shunting 4 days later, a repeat CT scan ( C- F) shows more clearly that the lesion extends through the midbrain into the third ventricle. who had had progressive right hemiplegia, right exotropia in complex showed only slight degenerative changes. However, primary gaze, bilateral adduction deficits, and impaired con- the lesion did extend to the caudal midbrain. Given that medial vergence. Complete demyelination was documented in both rectus subgroup neurons are scattered within the MLF ( see MLFs at the pons- midbrain junction. The oculomotor below), these neurons could have been affected in that patient. FIG 7. Case 4: Ocular motility. The left eye is exodeviated in primary gaze position. There is no adduction of either eye on horizontal gaze. Vertical gaze is normal, but convergence ( bottom) is deficient. 13 J Neuro- Ophthalmol, Vol. 27, No. 1, 2007 Chen and Lin FIG. 8 Case 4: Brain imaging. Axial FLAIR ( A- D), axial diffusion- weighted ( E- C), and coronal T2 ( H) MRI performed 5 days after onset shows a signal abnormality consistent with infarction that extends over almost the length of the left pons, beyond the midline in its dorsal portion in the low to middle pons but sparing the paramedian brainstem rostral to the midpontine level ( arrow). Another contradiction to the concept of medial rectus subnucleus involvement in WEBINO has come from the observations that exotropia also occurs ipsilaterally in unilateral INO, that is, in the wall- eyed monocular INO ( WEMINO) syndrome. Among four patients with WEMINO described by Johnston and Sharpe ( 11), pathologic analysis obtained for one patient showed that the lesion was confined to the pontine tegmentum. However, the authors did not specify whether the exotropia was ipsilateral or contralateral. Ikeda and Okamoto ( 12) reported a case of left WEMINO with a tiny MRI lesion in the left paramedian pontine tegmentum just adjacent to the fourth ventricle. However, this patient also had bilateral upbeat nystagmus and convergence deficiency, suggesting that the lesion might have extended into the midbrain. Recent anatomic studies ( 13- 15) are pertinent to the analysis of structure- function relationships in WEBINO. The oculomotor nuclear complex is a slanted structure with its ventral part pointing upward. The MLF passes just lateral and inferior to it. Of the medial rectus motoneurons, three subgroups can be identified. The first subgroup lies in the most ventral portion of the oculomotor complex. The second subgroup lies in the dorsal portion at the caudal level. The third subgroup, medial to the second, probably contains the medial rectus motoneurons responsible for convergence ( subgroup C of Buttner- Ennever et al) ( 13). Studies of Aktekin et al ( 14) and Glicksman ( 15) have shown that there are medial rectus subgroup neurons scattered within the MLF. Our Case 1 had WEBINO with impaired upgaze and convergence, evolving into a right INO with impaired convergence. MRI showed lesions in the paramedian midbrain, implying involvement of the medial rectus subnuclei along with the MLFs. The lesion in the first MRI looked like the midbrain cleft in a patient with WEBINO reported by Lagreze et al ( 16). Our Case 2 had a lesion at the pons-midbrain junction and right paramedian midbrain, where the possibility of medial rectus subnucleus involvement by edema or compression cannot be excluded. Our Case 3 also had a lesion extending through the midbrain into the third ventricle. In our Case 4, the lesion did not appear on MRI to reach the midbrain, but the patient clearly had convergence insufficiency. We acknowledge that convergence insufficiency may be seen in elderly persons and with cerebral lesions ( the patient had a right subcortical infarct), but it may also indicate that the lesion involved the midbrain. There is evidence from electro- oculographic studies that medial rectus subnuclear involvement is not necessary for exotropia. In two patients with WEBINO, Komiyama et al ( 17) demonstrated that deprivation of visual fixation with Frenzel goggles and eye closure diminished exotropia, 14 © 2007 Lippincott Williams & Wilkins WEBINO J Neuro- Ophthalmol, Vol. 27, No. 1, 2007 whereas one- eye fixation elicited marked outward deviation of the other eye. Conversely, a milder outward deviation of the eye on the INO side was noted during eye closure in three of seven patients with nonparalytic pontine exotropia ( NPPE, contralateral exotropia with INO). These findings imply that the exotropia in WEBINO and NPPE depends on whether the PPRF contralateral to the damaged MLF participates in the secondary deviation under fixation with the paretic eye( s). Johkura et al ( 18) described interesting ocular motor findings in four patients with OHS. All had mild outward deviation in both eyes with fixation prevented by Frenzel goggles. In three patients, the outward eye deviation was greater on the ipsilateral side and a transition from OHS to ipsilateral INO was noted, whereas a transition to ipsilateral gaze palsy was seen in the one patient whose deviation was greater on the contralateral side. These findings suggest that the eyes tend to be in divergent positions when fixation is prevented in OHS. Ipsilateral eye deviation is the result of MLF involvement and contralateral eye deviation is the result of PPRF involvement. The authors suggested that outward deviation of the ipsilateral eye is due to an imbalance of vestibular signals destined for the ipsilateral medial rectus in the MLF and that the outward deviation of the contralateral eye is due to an imbalance of PPRF signals. Drawing an analogy to the theory of Brandt and Dieterich ( 19,20) that the ocular tilt reaction ( skew torsion and head tilt) reflects imbalance of vestibular signals in the roll plane, ipsilateral exotropia may result from imbalance in the yaw plane in disorders involving the MLF. Ipsilateral exotropia may also occur in WEMINO or OHS. MLF axons carry signals from both PPRF and vestibular nuclei. Thus, WEBINO probably represents a bilateral form of NPPE, except that it is not necessarily pontine, and it is not likely to be a bilateral form of WEMINO. The presence of up-gaze palsy, as in our Cases 1 and 2, suggests that the lesion reaches into the midbrain. REFERENCES 1. Hoyt WF, Daroff RB. Supranuclear disorder of ocular control systems in man. In: Bach- Y- Rita P, Collins CC, Hyde JE, et al, eds. The Control of Eye Movement, New York: Academic Press; 1971: 175- 235. 2. Moncayo J, Bogousslavsky J. Vertebro- basilar syndromes causing oculo- motor disorders. Curr Opin Neurol 2003; 16: 45- 50. 3. Kline LB, Bajandas FJ. Neuro- Ophthalmology Review Manual, 5th ed rev. Thorofare, NJ: Slack; 2004: 69. 4. Gonyea EF Bilateral internuclear ophthalmoplegia: association with occlusive cerebrovascular diseases. Arch Neurol 1974; 31: 168- 73. 5. Takamatsu K, Ohta T. A case of infarction in the pontine tegmentum involving the bilateral MLF and unilateral paramedian pontine reticular formation [ in Japanese]. Rinsho Shinkeigaku 1995; 35: 272- 6. 6. Sharpe JA, Rosenberg MA, Hoyt WF, et al. Paralytic pontine exotropia: a sign of acute unilateral pontine gaze palsy and internuclear ophthalmoplegia. Neurology 1974; 24: 1076- 81. 7. Pierrot- Deseilligny CH, Chain F, Serdaru M, et al. The ' one- and- a-half syndrome: electro- oculographic analyses of five cases with deductions about the physiological mechanisms of lateral gaze. Brain 1981; 104: 665- 99. 8. Bogousslavsky J, Miklossy J, Regli F, et al. One- and- a- half syndrome in ischaemic locked- in state: a clinico- pathological study. J Neurol Neurosurg Psychiatry 1984; 47: 927- 35. 9. Wall M, Wray SH. The one- and- a- half syndrome- a unilateral disorder of the pontine tegmentum: a study of 20 cases and review of the literature. Neurology 1983; 33: 971- 80. 10. Strominger MB, Mincy EJ, Strominger Al, et al. Bilateral internuclear ophthalmoplegia with absence of convergent eye movements: clinicopathologic correlation. J Clin Neuroophthalmol 1986; 6: 57- 65. 11. Johnston JL, Sharpe JA. The WEMINO syndrome- wall- eyed, monocular internuclear ophthalmoplegia: an oculographic and neuro-pathologic characterization [ abstract]. Neurology 1994; 44( Suppl 2): A311. 12. Ikeda Y, Okamoto K. Lesion responsible for WEMINO syndrome confirmed by magnetic resonance imaging. J Neurol Neurosurg Psychiatry 2002; 73: 204- 5. 13. Buttner- Ennever JA, Akert K. Medial rectus subgroups of the oculomotor nucleus and their abducens internuclear input in the monkey. J Comp Neurol 1981; 197: 17- 27. 14. Aktekin M, Aldur MM, Bayramoglu A, et al. The organization of the somatic cell nuclei within the oculomotor nuclear complex in rats. Neuroanatomy 2002; 1: 22- 25. 15. Glicksman MA. Localization of motoneurons controlling the extraocular muscles of the rat. Brain Res 1980; 188: 53- 62. 16. Lagreze WD, Warner JE, Zamani AA, et al. Mesencephalic clefts with associated eye movement disorders. Arch Ophthalmol 1996; 114: 429- 32. 17. Komiyama A, Takamatsu K, Johkura K, et al. Internuclear ophthalmoplegia and contralateral exotropia Nonparalytic pontine exotropia and WEBINO syndrome. Neuroophthalmology 1998; 19: 33^ 4. 18. Johkura K, Komiyama A, Kuroiwa Y Eye deviation in patients with one- and- a- half syndrome. Eur Neurol 2000; 44: 210- 5. 19. Dieterich M, Brandt T. Thalamic infarctions: differential effects on vestibular function in the roll plane ( 3 5 patients). Neurology 1993 ; 43: 1732^ 0. 20. Brandt T, Dieterich M. Vestibular syndromes in the roll plane: topographic diagnosis from brainstem to cortex. Ann Neurol 1994; 36: 337^ 7. 15 |