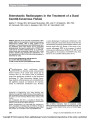
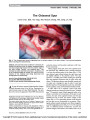
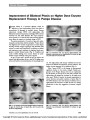
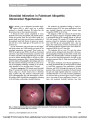
| OCR Text |
Show Pupillary Dysfunction in an Atypical Case of Mitochondrial Myopathy With Tubular Aggregates Nadeem Ali, MA, MRCOphth, FRCSEd (Ophth), Catherine E. Woodward, BSc, Mary Sweeney, BSc, Rahul Phadke, MD, FRCPath, Janice L. Holton, PhD, MRCPath, James Acheson,MRCP, FCRS (Glas), FRCOphth, Gordon T. Plant,MD, FRCP, FRCOphth, Fion D. Bremner, PhD, FRCOphth Abstract: A 62-year-old man presented with diplopia, ocular ductional deficits, and sluggish pupils. Pupillom-etry demonstrated large hyporeactive pupils with no evi-dence of damage to the sympathetic or parasympathetic innervation, indicating a myopathy of the iris muscula-ture. A single large deletion in mitochondrial DNA and characteristic histochemical features on muscle biopsy suggested a mitochondrial cytopathy. However, ultra-structural examination of skeletal muscle fibers showed tubular aggregates (TAs), a finding not reported in mito-chondrial cytopathy. The combination of pupillary abnor-malities and TAs suggests that mitochondrial dysfunction may not explain the full extent of abnormalities in this case. Journal of Neuro-Ophthalmology 2010;30:153-156 doi: 10.1097/WNO.0b013e3181dbfdcd 2010 by North American Neuro-Ophthalmology Society The smooth muscles of the iris are reported to be spared in chronic progressive external ophthalmoplegia (CPEO), a mitochondrial cytopathy (1,2). However, pu-pillary function has never been quantitatively studied in this condition. Moreover, there is no reason why these muscles should be spared from the effects of mitochondrial dysfunction. We present a case in which ocular ductional deficits were combined with pupil dysfunction and unusual ultra-structural muscle features, raising questions about the na-ture of this condition. CASE REPORT A 62-year-old Indian man presented with an 8-month history of slowly progressive binocular horizontal diplopia. He reported no ptosis, diurnal variation in the diplopia, fatigability, or weakness of his arms or legs. There had been no pain, redness, lid swelling, or proptosis. Medical history was unremarkable, and he was a nonsmoker and non-drinker. There was no family history of neurological disease. Neuro-Ophthalmological Examination Our examination revealed best-corrected visual acuities of 20/20 in both eyes, normal color vision, and full visual fields. The pupils were noted to react sluggishly both to light and to the viewing of a near target. Horizontal ductions were moderately reduced in both eyes. In the right eye, there was a reduction in supraduction, and in the left eye, a re-duction in infraduction. The patient reported diplopia in all positions of gaze. In primary gaze position, there was a large alternating exotropia with a large left hypertropia (Fig. 1). There was no ptosis, and levator function and orbicularis strength were clinically normal. Intraocular examination revealed visually insignificant posterior cortical cataracts and mild changes in the macular retinal pigment epithelium, findings that were thought to be age related. The peripheral retina appeared normal. Examination of the remaining cranial nerves was unremarkable. Tone and strength were normal in all muscles groups, with neither fatigability nor myotonia. Laboratory Studies The patient underwent the following investigations, which produced normal or negative results: acetylcholine receptor antibodies, muscle-specific tyrosine kinase (MUSK) anti-bodies, striated muscle antibodies, thyroid thyroglobulin antibodies, thyroid microsomal antibodies, and treponemal Department of Neuro-Ophthalmology (NA, JA, GTP, FDB); Neu-rogenetics Unit (CEW, MS); Department of Neuropathology (RP, JLH), National Hospital for Neurology and Neurosurgery, Queen Square, London, United Kingdom. The authors declare no financial interests. Address correspondence to Nadeem Ali, MA, MRCOphth, FRCSEd (Ophth), Moorfields Eye Hospital, City Road, London EC1V 2PD; E-mail: nadeem.ali@nhs.net Ali et al: J Neuro-Ophthalmol 2010; 30: 153-156 153 Original Contribution Copyright © North American Neuro-ophthalmology Society.Unauthorized reproduction of this article is prohibited. serology. Intravenous edrophonium had no effect on his ophthalmoplegia. Imaging Studies CT of the brain and orbits and MRI of the thymus were normal. Electromyography Electromyography revealed normal nerve conduction, re-petitive stimulation, and single-fiber studies. Muscle sam-pling showed abundant spiky polyphasic units recorded not only from the orbicularis oculi but also minimally from the extensor digitorum communis, tibialis anterior, and rectus femoris. These findings were suggestive of a mild myopathic process rather than neuromuscular junction dysfunction. Muscle Biopsy Triceps muscle biopsy revealed the presence of 3 ragged red fibers and more than 10 cytochrome oxidase-negative fibers. Mitochondrial respiratory chain enzyme activity assays were normal. Electron microscopy showed subsarcolemmal ac-cumulations of scattered abnormal mitochondria, many of which contained type 1 paracrystalline inclusions. Tubular aggregates (TAs) were noted in several fibers, some of which contained abnormal mitochondria (Fig. 2). No TAs were seen at the light microscopic level. Genetic Analysis Mitochondrial genetic analysis confirmed a single large deletion in mitochondrial DNA detected by long-range polymerase chain reaction followed by Southern blotting. Sequencing confirmed the presence of the common deletion of 4,977 base pairs, with break points in the flanking repeats between nucleotides 8,470 and 8,482 and nucleotides 13,447 and 13,459. The patient was therefore diagnosed with CPEO. Pupillary Function Based on the clinical impression of hyporeactive pupils, infrared video pupillometry was performed and compared with our normative database of measurements from 315 healthy control subjects (3) (Fig. 3; Table 1). Slit-lamp examination showed no abnormality of pupil shape and no iris damage or sector palsy. The resting pupil diameters were significantly larger than expected for his age (outside the 95% upper limit of the normal range) both in darkness and in light. The amplitudes of the responses of both pupils to a transient light stimulus were attenuated (below 95% lower limit of the normal range). The pupillary miosis to the viewing of a near target was also attenuated (although it could only be reliably recorded from the right eye), and there was no light-near dissociation. Startle responses (mydriasis following a sudden noise) were present but sluggish in both eyes. Pharmacological testing demonstrated a normal mydri-atic response to topical 4% cocaine drops and no cholinergic supersensitivity to 0.1% pilocarpine drops. Pupillometry thus confirmed that both pupils were abnormally large with sluggish responses to light, and near stimuli, and sudden FIG. 1. Our patient displays a left hypertropia and exo-tropia in primary gaze and no ptosis. FIG. 2. Electron microscopy of triceps muscle biopsy. A. Subsarcolemmal accumulations of abnormal mitochondria (M). B. Abnormal mitochondria (m), and tubular aggregates (TA) in the same fiber. Original Contribution 154 Ali et al: J Neuro-Ophthalmol 2010; 30: 153-156 Copyright © North American Neuro-ophthalmology Society.Unauthorized reproduction of this article is prohibited. noise. Without evidence of damage to the sympathetic or parasympathetic innervation, myopathic dysfunction was suggested. DISCUSSION CPEO describes a spectrum of conditions characterized by bilateral ptosis and global restriction of eye movements (4). It represents the commonest ocular manifestation of the mitochondrial myopathies (5) and can occur in isolation or in association with nonocular features (6). However, there are several features of the present case that are not typical of CPEO. First, the ductional deficits were not symmetrical in the 2 eyes. The eyes were markedly misaligned, whereas in CPEO, they are usually aligned. Although asymmetric ophthalmoplegia has been rarely described (4,7), its extent, when accurately measured, is usually small. One study found that in 68% of muscle pairs, the degree of asymmetry was less than 5 ; asymmetry greater than 18 occurred in less than 2% of muscle pairs (8). Second, our patient lacked ptosis. Bilateral ptosis is al-most always found in CPEO and is the presenting com-plaint in up to 90% of cases (4). Cases of CPEO without ptosis have only rarely been described (9). Third, involvement of the iris musculature has not been reported in CPEO. In the present case, pupillometry confirmed the clinical impression of large sluggish pupils. The clinical signs, pupillometric measurements, and phar-macological tests indicated intact innervation of the sphincter and dilator iris muscles but poor contractility due to an intrinsic myopathic process. Given the genetic and histological evidence supporting a diagnosis of mitochon-drial cytopathy, it seems reasonable to conclude that in this unusual case, the smooth muscles of the iris may have been affected by this single large mitochondrial DNA deletion. The large resting diameters of these pupils suggest a greater FIG. 3. Pupil responses to a transient light stimulus in our patient (A) and in a healthy control subject aged 63 years (B). In comparison with the healthy control subject, the pupils of our patient have larger resting diameters and show attenuated responses to light stimulus. TABLE 1. Pupillometric measurements in our patient. Measurement Right pupil Left pupil Normal range (3) Dark diameter (mm) 7.80 7.01 4.00-7.25* Light diameter (mm) 6.58 5.53 1.80-3.82* Amplitude of light response (mm) 0.75 0.98 1.79-3.95 (R)† 1.61-3.55 (L)† T3/4 redilatation time (seconds) 4.96 5.28 0.30-2.72 (R)‡ 0.44-2.86 (L)‡ Amplitude of near response (mm) 0.58 Poor quality recording None defined Startle response Present Present None defined The normal ranges are for healthy control subjects. * = age matched; † = expected values given the observed resting diameters in the dark; ‡ = amplitude matched or the range of measurements found in healthy control subjects when stimulus intensity is adjusted to produce light responses of similar amplitude to those seen in this patient. Original Contribution Ali et al: J Neuro-Ophthalmol 2010; 30: 153-156 155 Copyright © North American Neuro-ophthalmology Society.Unauthorized reproduction of this article is prohibited. impact of this genotype on sphincter muscle fibers than on dilator muscle fibers. We were struck by the apparent similarity between the pupil findings in our case and those associated with myo-tonic dystrophy (dystrophia myotonica, DM), another condition that can produce ophthalmoplegia. The pupils in patients with DM type 1 are often small or of medium size, with sluggish low amplitude light responses. They show the presence of a startle response, no light-near dissociation, and no cholinergic hypersensitivity (10). However, the present case had no other clinical features suggestive of DM (family history, grip myotonia, iridescent lens opacities), and molecular genetic testing for the recognized mutations associated with DM1 or DM2 was negative, thus making a co-occurrence of these 2 genetic disorders unlikely. A strikingly unusual feature of the present case was the finding of TAs on electron microscopy of the muscle biopsy. TAs in skeletal muscle fibers can occur as a nonspecific finding in a variety of conditions such as periodic paralysis, myotonic disorders, hyperaldosteronism, chronic use of drugs, and alcoholism. In addition, TAs have also been found more specifically in exercise-induced cramps, myasthenic syndromes, and dominantly or recessively inherited familial myopathies (11). Abnormal pupils have been reported in some of the cases of familial TA myopathies (12,13). However, TAs are not recognized as a feature of mitochondrial cytopathies. There is only a single report of a patient with distal myopathy who was found to have multiple deletions of mitochondrial DNA and a high density of TAs (14). The fact that pupil involvement is not seen in typical CPEO, together with the finding of tubular aggregates on muscle biopsy in our patient, suggests that mitochondrial cytopathy might not be the full extent of the abnormality here. Perhaps this patient has a combination of a mito-chondrial cytopathy and an inherited disorder of other origin. Additionally, this case raises the question as to the extent of undetected smooth muscle involvement in mi-tochondrial cytopathy. ACKNOWLEDGMENT The patient shown in Figure 1 provided written consent for the image to be published. REFERENCES 1. Kline LB, Bajandas FJ. Neuro-Ophthalmology Review Manual, 5th Edition. Thorofare: SLACK Inc, 2003. 2. Pane A, Burdon M, Miller NR. The Neuro-ophthalmology Survival Guide. Edinburgh: Mosby/Elsevier, 2007. 3. Bremner F, Smith S. Pupil findings in a consecutive series of 150 patients with generalised autonomic neuropathy. J Neurol Neurosurg Psychiatry. 2006;77:1163-1168. 4. Bau V, Zierz S. Update on chronic progressive external ophthalmoplegia. Strabismus. 2005;13:133-142. 5. Schoser BG, Pongratz D. Extraocular mitochondrial myopathies and their differential diagnoses. Strabismus. 2006;14:107-113. 6. Schmiedel J, Jackson S, Scha¨fer J, Reichmann H. Mitochondrial cytopathies. J Neurol. 2003;250:267-277. 7. Petty RK, Harding AE, Morgan-Hughes JA. The clinical features of mitochondrial myopathy. Brain. 1986;109: 915-938. 8. Richardson C, Smith T, Schaefer A, Turnbull D, Griffiths P. Ocular motility findings in chronic progressive external ophthalmoplegia. Eye. 2005;19:258-263. 9. Miller NR, Newman NJ. Walsh and Hoyt's Clinical Neuro-ophthalmology, 5th edition. Baltimore: Williams & Wilkins, 1998. 10. Loewenfeld IE. The Pupil: Anatomy, Physiology, and Clinical Applications, 2nd Edition. Oxford: Butterworth-Heinemann, 1999. 11. Mu¨ller HD, Vielhaber S, Brunn A, Schro¨der JM. Dominantly inherited myopathy with novel tubular aggregates containing 1-21 tubulofilamentous structures. Acta Neuropathol. 2001;102:27-35. 12. Jacques TS, Holton J, Watts PM, Wills AJ, Smith SE, Hanna MG. Tubular aggregate myopathy with abnormal pupils and skeletal deformities. J Neurol Neurosurg Psychiatry. 2002;73:324-326. 13. Shahrizaila N, Lowe J, Wills A. Familial myopathy with tubular aggregates associated with abnormal pupils. Neurology. 2004;63:1111-1113. 14. Garrard P, Blake J, Stinton V, Hanna MG, Reilly MM, Holton JL, Landon DN, Honan WP. Distal myopathy with tubular aggregates: a new phenotype associated with multiple deletions in mitochondrial DNA? J Neurol Neurosurg Psychiatry. 2002;73:207-208. Original Contribution 156 Ali et al: J Neuro-Ophthalmol 2010; 30: 153-156 Copyright © North American Neuro-ophthalmology Society.Unauthorized reproduction of this article is prohibited. |