| OCR Text |
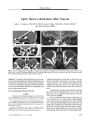
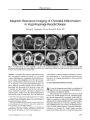
Show PHOTO ESSAY Progression from Anomalous Optic Discs to Visible Optic Disc Drusen Terrence S. Spencer, MD, Bradley J. Katz, MD, PhD, Steve W. Weber, MD, and Kathleen B. Digre, MD Abstract: At age 5, a patient underwent fundus photography that disclosed elevated optic discs without drusen. A head computed tomography did not show optic nerve calcification. At age 9, no disc drusen were evident by ophthalmoscopy, but a CT now showed optic nerve calcification. At age 12, optic disc drusen were faintly evident on photographs; visual fields showed blind spot enlargement OD and an arcuate defect OS. At age 21, he had numerous discrete disc drusen in both eyes, disc pallor, and slight progression of the visual field defects. This case documents the progression from anomalous optic discs to ophthalmoscopically visible optic nerve drusen over a 16- year period. ( JNeuvo- Ophthalmol 2004; 24: 297- 298) At age 2, an otherwise healthy boy underwent medial rectus recession OU for congenital esotropia. Fundus examinations were recorded as normal. On routine follow- up at age 5, he was found to have markedly elevated optic discs ( Fig. 1). No drusen were observed. Computed tomography of the head did not show calcification associated with buried optic nerve drusen. Over the next several years, he and immediate family members underwent additional ophthalmologic examinations that disclosed no disc anomalies in any family members. At age 9, drusen were still not ophthalmoscopically visible, but computed tomography now revealed optic nerve calcification. He was presumed to have buried optic nerve drusen ( OND). At age 10, automated perimetry revealed an enlarged blind spot OD and arcuate defects OS Department of Ophthalmology ( TSS, KBD, BJK), John A. Moran Eye Center, University of Utah Health Sciences Center, Salt Lake City, Utah, and Glacier Eye Clinic ( SWW), Kalispell, Montana. Supported by NIH RR16427 ( BJK) and an unrestricted grant to the Department of Ophthalmology and Visual Sciences from Research to Prevent Blindness, Inc, New York, New York. Address correspondence to Bradley J. Katz, MD, PhD, John A. Moran Eye Center, 75 N. Medical Dr., University of Utah Health Sciences Center, Salt Lake City, UT 84132. E- mail: Bradley. Katz@ hsc. utah. edu FIG. 1. Progression from anomalous optic discs to visible optic nerve drusen. A. Age 5: both discs show ophthalmoscopic elevation but no drusen. A head computed tomography showed no optic nerve calcification. B. Age 12: the right optic disc has not changed ophthalmoscopically, but the left disc now has a " lumpy bumpy" appearance and appears pale. Three years earlier, computed tomography had shown optic disc calcification in both eyes. C. Age 21: multiple large drusen are now ophthalmoscopically visible bilaterally. ( Fig. 2). At age 12, fundus photos showed a stable appearance of the right optic nerve, but the left optic nerve had taken on a " lumpy bumpy" appearance with some pallor ( Fig. 1). J Neuro- Ophthalmol, Vol. 24, No. 4, 2004 297 JNeuro- Ophthalmol, Vol. 24, No. 4, 2004 Spencer et al FIG. 2. Minimal progression of visual field defects from age 10 to age 21. A. Age 10: there is an enlarged blind spot OD and superior and inferior arcuate defects OS. B. Age 21: the defects OS have changed minimally and very shallow arcuate defects have appeared OD. AGE 21 At age 21, he still had no visual symptoms but now mamfested ophthalmoscopically obvious optic disc dnisen bilaterally ( Fig. 1). Perimetry disclosed minimal progression of the visual field defects ( Fig. 2). Although he did not have ocular hypertension, he was treated with topical brimonidine 0.2% in an effort to stabilize his visual field defects. OND are calcified, acellular, laminated concretions that form within the substance of the optic nerve. They occur in approximately 2% of the population ( 1) and are transmitted as an autosomal dominant trait ( 2). Some cases of OND appear to be sporadic ( 3), but most investigators agree that OND is a genetic disease that segregates in an autosomal dominant fashion ( 4), suggesting that OND is the most common inherited optic neuropathy. Some dnisen are visible on funduscopic examination (" visible drusen"), whereas some optic nerves harbor dnisen that are not visible on ophthalmoscopy (" buried drusen"). Buried drusen may be detected by ultrasonography ( 5), computed tomography ( 6), or red- free photography ( 7). Although most OND patients are asymptomatic, 71% to 75% have peripheral visual defects ( 8). There is no known treatment of the visual field loss associated with OND. This case demonstrates how anomalously elevated optic nerves in a child can represent buried optic disc drusen ( 9,10), which may eventually evolve to visible OND. REFERENCES 1. Friedman AH, Gartner S, Modi SS. Drusen of the optic disc. A retrospective study in cadaver eyes. Br J Ophthalmol 1975; 59: 413^ 21. 2. Lorentzen SE. Drusen of the optic disk. A clinical and genetic study. Acta Ophthalmol ( Copenh) 1966; Suppl90: l- 180. 3. Antcliff RJ, Spalton DJ. Are optic disc drusen inherited? Ophthalmology 1999; 106: 1278- 1281. 4. Lorentzen SE. Drusen of the optic disc. Dan Med Bull 1967; 14: 293- 298. 5. Boldt HC, Byrne SF, DiBernardo C. Echographic evaluation of optic disc drusen. J Clin Neuroophthalmol 1991; 11: 85- 91. 6. Kurz- Levin MM, Landau K. A comparison of imaging techniques for diagnosing drusen of the optic nerve head. Arch Ophthalmol 1999; 117: 1045- 1049. 7. Mustonen E, Alanko HI, Nieminen H. Changes in optic disc drusen. Demonstration by stereophotographs and electronic subtraction. Acta Ophthalmol ( Copenh) 1982; 60: 3- 15. 8. Savino PJ, Glaser JS, Rosenberg MA. A clinical analysis of pseudo-papilledema. II. Visual field defects. Arch Ophthalmol 1979; 97: 71- 75. 9. Miller NR. Appearance of optic disc drusen in a patient with anomalous elevation of the optic disc [ letter]. Arch Ophthalmol 1986; 104: 794- 5. 10. Auw- Haedrich C, Staubach F, Witschel H. Optic disk drusen. Surv Ophthalmol 2002; 47: 515- 532. 298 © 2004 Lippincott Williams & Wilkins [KBDdcapseudoburieddrusen] [KBDdcaburieddrusen] |