| OCR Text |
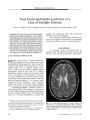
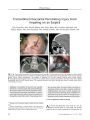
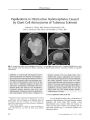
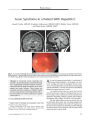
Show PHOTO ESSAY Papilledema in Obstructive Hydrocephalus Caused by Giant Cell Astrocytoma of Tuberous Sclerosis Deborah Y. Chong, MD, Parima Hirunwiwatkul, MD, Paul E. McKeever, MD, PhD, and Jonathan D. Trobe, MD FIG. 1. Preoperative MRIs. Axial FLAIR ( A), postcontrast T1 coronal ( B), and postcontrast T1 sagittal ( C) MRIs show a large mass centered within the foramen of Monro, extending to dilated lateral ventricles. Subcortical nodules are apparent { arrowheads). Abstract: A 5- year- old girl with progressive hemiparesis and headache was found by brain imaging to have a large tumor centered at the foramen of Monro, blocking cerebrospinal outflow and producing massive lateral ventriculomegaly. Total excision of the mass led to a pathologic diagnosis of giant cell astrocytoma. Dermatologic abnormalities had been detected shortly after birth but were unexplained. Abdominal imaging disclosed renal cysts, and ophthalmologic examination disclosed papilledema and retinal plaques. On this basis, a diagnosis of tuberous sclerosis ( TS) was finally made. Two months after surgery, papilledema had resolved and visual function appeared to be normal. Although the patient apparently escaped visual loss, other reports affirm that giant cell astrocytoma, a common tumor in TS, may go undetected for long enough to produce irreversible optic neuropathy from chronic papilledema. Because patients with TS may not report visual loss, they should undergo periodic ophthalmologic screening. (/ Neuro- Ophthalmol 2007; 27: 50- 54) Kellogg Eye Center, Department of Ophthalmology and Visual Sciences ( DYC, JDT), and Departments of Pathology ( PEM) and Neurology( JDT), University of Michigan, Ann Arbor, Michigan; and Department of Ophthalmology ( PH), Faculty of Medicine, Chulalongkorn University, Bangkok, Thailand. Address correspondence to Jonathan D. Trobe, MD, Kellogg Eye Center, 1000 Wall Street, Ann Arbor, MI 48105; E- mail: jdtrobe@ umich. edu A 5- year- old girl presented with a 2 month history of progressive right hemiparesis, behavioral changes, morning headaches, and emesis. Brain MRI revealed a large intraventricular mass centered within the foramen of Monro and left lateral ventricle and extending into the right lateral ventricle ( Fig. 1). The lateral ventricles were abnormally dilated. 50 J Neuro- Ophthalmol, Vol. 27, No. 1, 2007 Papilledema in Giant Cell Astrocytoma J Neuro- Ophthalmol, Vol. 27, No. 1, 2007 FIG. 2. Hypopigmented macule on right upper forehead representing an ash- leaf spot ( arrows) and erythematous papules over nasal bridge and malar eminences consistent with angiofibromas ( arrowhead). There was no history of developmental delay or seizures. Her parents and a dermatologist had noted hypopigmented macules 5 days after birth and erythematous papules over the midface at age 3 ( Fig. 2), but no diagnosis was made. The combination of skin lesions and the brain mass, which appeared radiologically to be a subependymal giant cell astrocytoma, suggested a diagnosis of tuberous sclerosis ( TS). FIG. 3. Abdominal postcontrast T1 axial MRI demonstrates cysts in the left kidney ( arrows). The patient underwent an abdominal MRI that showed renal cysts ( Fig. 3) and a cardiac nuclear perfusion study that demonstrated a left ventricular aneurysm. The large intraventricular brain mass was resected, and pathologic evaluation confirmed the diagnosis of giant cell astrocytoma ( Fig. 4). The tumor was composed mainly of large plump astrocytic cells that were usually unin-ucleated. Multinucleated cells with two or three nuclei were uncommon. Although the nuclei were pleomorphic, a clue to their relatively benign nature included rounded borders without sharp indentation of the nuclear membranes ( Fig. 4A). Mitotic activity was minimal. The MIB- 1 proliferation index varied from zero to a maximum of 13% FIG. 4. Pathology of excised intraventricular giant cell astrocytoma. A. Pleomorphic cells with large, rounded nuclei that are either centric or eccentric within abundant finely granular cytoplasm. Giant cells greater than 50 | xm in diameter mingle with smaller cells. Many extend long cellular processes. Their nuclei have rounded borders ( arrow) without sharp indentations of their nuclear membranes. Small vessels have thin walls ( arrowhead). Hematoxylin and eosin ( H& E) stain. B. Neoplastic astrocytes stain positively for glial fibrillary acidic protein ( GFAP). GFAP- positive cellular processes extend from these cells ( arrow). The thin walls and contents of vessels do not express GFAP ( arrowhead). C. Large " kissing neurons" ( arrow) stain positively for neurofilament protein ( NFP). D. A distinct border of the tumor lies just below the ependymal lining ( arrow) of the lateral ventricle. These tumors often demonstrate biphasic regions that have cellular ( c) and microcystic fibrillar zones. H& E stain. 51 J Neuro- Ophthalmol, Vol. 27, No. 1, 2007 Chong et al FIG. 5. A. Fundus photographs taken 11 days postoperatively show papilledema. B. Fundus photographs taken 2 months postoperatively show complete resolution of papilledema. C. Retinal astrocytic hamartomas are visible in the right eye. among different microscopic fields. Few nuclei overex-pressed p53. Most of the neoplastic cells expressed glial fibrillary acidic protein ( GFAP) ( Fig. 4B). The pattern of GEAP expression was astrocytic, with GFAP extending out into long, stellate cellular processes. A few cells expressed neurofilament protein ( Fig. 4C). This expression is more common in giant cell astrocytomas than in astrocytomas of higher grade and has generated debate about classification and nomenclature of this tumor ( 1- 3). The tumor margin within brain tissue was distinct ( Fig. 4D). Eleven days after surgery, ophthalmologic examination disclosed normal visual acuity, confrontation visual fields, ocular motility, pupillary reflexes, intraocular pressures, ocular adnexae, and anterior segments. Ophthalmoscopy revealed bilateral optic disc swelling ( Fig. 5A) and translucent, noncalcified lesions in the retinal nerve fiber layer in the right eye ( Fig. 5C). Within 2 months after tumor resection, the papilledema had resolved ( Fig. 5B). By 4 months after surgery, all neurologic symptoms had resolved. MRI revealed that the tumor had been 52 © 2007 Lippincott Williams & Wilkins Papilledema in Giant Cell Astrocytoma J Neuro- Ophthalmol, Vol. 27, No. 1, 2007 FIG. 6. Postoperative MRIs. Axial FLAIR ( A), postcontrast T1 coronal ( B), and postcontrast T1 sagittal ( C) MRIs show complete resection of the tumor and decompression of the lateral ventricles. Persistent subcortical nodules ( arrowheads) and a subependymal nodule ( arrow) are visible. completely resected, and the ventricles were decompressed ( Fig. 6). This case is presented to highlight the threat to vision from chronic papilledema caused by obstructive hydrocephalus induced by blockage of the foramen of Monro from a subependymal giant cell astrocytoma in TS. Our patient maintained full visual function, presumably because the papilledema was not severe. Other patients may not be so fortunate ( 2,4,5). Occurring in approximately 6%- 19% of patients with TS, ( 1) giant cell astrocytomas are considered histologically benign but may grow silently to an enormous size, as exemplified by our patient. Growth may proceed for a long time without causing headache or other neurologic symptoms. The visual loss from undetected chronic papilledema may go unnoticed until it encroaches on the fixational area. Even then, patients with TS may not report it because of mental incapacity. Visual loss has been reported in 14%- 67% of patients with TS who have subependymal giant cell astrocytomas( l- 3). Despite surgical decompression, optic nerve damage can persist or even progress( 2,4,5). Our patient had dermatologic signs of TS noted shortly after birth and at age 3 but did not undergo neuroimaging to evaluate for an intracranial mass until she presented at age 5 with neurologic symptoms. She did not have an ophthalmologic examination until after hydrocephalus was noted on neuroimaging and the tumor had been resected. Subependymal giant cell astrocytomas may cause not only visual loss but also death. They are blamed for 25% of deaths in TS, with 12.5% directly resulting from elevated intracranial pressure ( 6). Poorer outcomes have been noted in patients older than 11 or 12 years at the time of resection of the tumor ( 2,5). Because ophthalmoscopy is difficult for non-ophthalmologists, it is reasonable for all patients with TS to undergo periodic ophthalmologic examinations to rule out papilledema. The finding of papilledema would mandate neuroimaging. Because giant cell astrocytomas can recur after surgical resection and evolve from smaller subependymal nodules ( 1), periodic follow- up ophthalmoscopy is also reasonable. Visual loss also occurs rarely in the setting of retinal astrocytic hamartomas. Although these are typically static or slow- growing lesions ( 7), they may give rise to vitreous hemorrhage ( 8), exudative retinal detachment ( 9), neo-vascular glaucoma ( 9), and invasive perforation of the sclera ( 9). In consideration of these facts, ophthalmologic monitoring is warranted. Lastly, consultation with specialists in other fields may also assist in the diagnosis and management of TS. Dermatologic examination for ash- leaf spots ( hypopig-mented macules), shagreen patches ( leathery connective tissue nevi), facial angiofibromas ( erythematous papules formerly termed " adenoma sebaceum"), fibrous plaques of the forehead ( raised, discolored patches), and periungual fibromas ( fleshy tumors around or underneath the nail) may contribute to making an initial diagnosis of TS ( 10). Patients should also undergo evaluation for renal cysts and angiomyolipomas. Although rare, renal failure, significant hemorrhaging, and malignant transformation can occur from these renal lesions ( 10). Furthermore, patients should 53 J Neuro- Ophthalmol, Vol. 27, No. 1, 2007 Chong et al be screened for cardiac rhabdomyomas, which can cause cardiac arrhythmias and congestive heart failure, and pulmonary lymphangiomyomatosis, which can lead to dyspnea and pneumothorax ( 10). REFERENCES 1. Kim SK, Wang KC, Cho BK, et al. Biological behavior and tumorigenesis of subependymal giant cell astrocytomas. J Neuro-oncol 2001; 52: 217- 25. 2. Goh S, Butler W, Thiele EA. Subependymal giant cell tumors in tuberous sclerosis complex. Neurology 2004; 63: 1457- 61. 3. Sharma MC, Ralte AM, Gaekwad S, et al. Subependymal giant cell astrocytoma- a clinicopathological study of 23 cases with special emphasis on histogenesis. Pathol Oncol Res 2004; 10: 219- 24. 4. Kiratli H, Bilgic S. Spontaneous regression of retinal astrocytic hamartoma in a patient with tuberous sclerosis. Am J Ophthalmol 2002; 133: 715- 6. 5. Dotan SA, Trobe JD, Gebarski SS. Visual loss in tuberous sclerosis. Neurology 1991; 41: 1915- 7. 6. Shepherd CW, Gomez MR, Lie JT, et al. Causes of death in patients with tuberous sclerosis. Mayo Clin Proc 1991; 66: 792- 6. 7. Zimmer- Galler IE, Robertson DM. Long- term observation of retinal lesions in tuberous sclerosis. Am J Ophthalmol 1995; 119: 318- 24. 8. Coppeto JR, Lubin JR, Albert DM. Astrocytic hamartoma in tuberous sclerosis mimicking necrotizing retinochoroiditis. JPediatr Ophthalmol Strabismus 1982; 19: 306- 13. 9. Shields JA, Eagle RC Jr, Shields CL, et al. Aggressive retinal astrocytomas in 4 patients with tuberous sclerosis complex. Arch Ophthalmol 2005; 123: 856- 63. 10. Crino PB, Nathanson KL, Henske EP. The tuberous sclerosis complex. N EnglJ Med 2006; 355: 1345- 56. 54 © 2007 Lippincott Williams & Wilkins |