| Title |
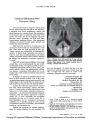
Intracranial meningiomatosis causing foster kennedy syndrome by unilateral optic nerve compression and blockage of the superior sagittal sinus. |
| Creator |
Acebes, X; Arruga, J; Acebes, J J; Majos, C; Muoz, S; Valero, Isaac Alarcon |
| Affiliation |
Ophthalmology Department, Bellvitge Hospital, L'Hospitalet de Llobregat, Spain. |
| Subject |
Adult; Female; Fluorescein Angiography; Humans; Magnetic Resonance Imaging; Meningeal Neoplasms; Meningioma; Nerve Compression Syndromes; Optic Nerve Diseases; Sinus Thrombosis, Intracranial; Superior Sagittal Sinus; Visual Fields |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225847 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6q2759g/225847 |