| Title |
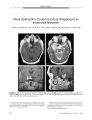
Facial and Trigeminal Neuropathies in Cavernous Sinus Fistulas |
| Creator |
Jensen, RW; Chuman, H; Trobe, JD; Deveikis, JP |
| Affiliation |
Kellogg Eye Center, Department of Ophthalmology 1000 Wall Street, Ann Arbor, MI 48105-1912, USA. |
| Abstract |
Three patients with carotid-cavernous fistulas had prominent ipsilateral facial nerve neuropathy. One patient also had ipsilateral third division trigeminal neuropathy, manifesting as painful trismus and lower facial numbness. Rarely reported in carotid-cavernous fistula, these neuropathies may occur when there is substantial drainage of the fistula into a dilated inferior petrosal sinus. Closure of the fistula in two cases resulted in full recovery of the neuropathies within weeks to months. The neuropathies may be caused by ischemia from an unfavorable arteriovenous flow gradient, venous compression, or secondary inflammation. |
| Subject |
Adult; Older people; Carotid Arteries/radiography; Carotid-Cavernous Sinus Fistula/complications; Carotid-Cavernous Sinus Fistula/diagnosis; Carotid-Cavernous Sinus Fistula/surgery; Cerebral Angiography; Facial Nerve Diseases/etiology; Female; Humans; Magnetic Resonance Imaging; Male; Middle Older people; Treatment Outcome; Trigeminal Nerve Diseases/complications; Trigeminal Nerve Diseases/etiology; Trismus/etiology |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225377 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6p87j0r/225377 |