| OCR Text |
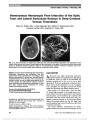
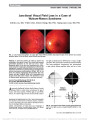
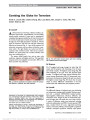
Show Acute Optic Neuropathy Associated With an Intracranial Mass in a Patient With POEMS syndrome Heather E. Moss, MD, PhD, Grant T. Liu, MD Abstract: A 43-year-old man with POEMS syndrome (poly-neuropathy, organomegaly, endocrinopathy, monoclonal gammopathy, and skin changes), including long-standing optic disc swelling, had sudden painless vision loss in the left eye. Brain MRI revealed an intracranial mass adjacent to the left optic nerve and enhancement of the optic nerve. The mass decreased in size following chemotherapy for mye-loma with some recovery of vision. This represents a unique case of optic neuropathy due to presumed plasmacytoma in osteosclerotic IgA myeloma and POEMS syndrome. Journal of Neuro-Ophthalmology 2012;32:45-47 doi: 10.1097/WNO.0b013e318234db5d © 2012 by North American Neuro-Ophthalmology Society Observations of multiorgan system involvement associ-ated with plasma cell dyscrasia led to the characteriza-tion of POEMS syndrome, with the acronym standing for prominent findings of polyneuropathy, organomegaly, endo-crinopathy, monoclonal gammopathy, and skin changes. Other common signs include optic disc edema, ascites, pleural effusion, and thrombocytosis. Although optic disc edema occurs in one third to one half of patients with POEMS syndrome (1), vision loss is rare. CASE REPORT A 43-year-old man noted sudden painless loss of vision in his left eye following 2-3 days of stuttering visual decline in that eye. Six years earlier, he had been diagnosed with POEMS syndrome on the basis of demyelinating polyneuropathy, hepatosplenomegaly, hypogonadism, hyperprolactinemia, hypothyroidism, vitamin D deficiency, adrenal insufficiency, IgA lambda monoclonal proteinemia, skin darkening, a scle-rotic bone lesion in the spine, and extravascular volume over-load causing ascites and pleural effusions. He had received a stem cell transplant with clinical improvement for 2 years followed by recurrent symptoms of volume overload. Mild optic disc swelling and high serum vascular endothelial growth factor (VEGF) were found at the time of recurrence and were attributed to POEMS syndrome. He had been chronically managed on 20 mg of dexamethasone weekly. Chemotherapy was planned for treatment of recurrent symptoms and neces-sitated stopping dexamethasone, 2 weeks prior to vision loss. Two weeks prior to vision loss, his acuity was 20/40 in each eye with normal color vision, posterior subcapsular cataracts, and bilateral optic disc swelling (Fig. 1). The disc swelling had been present for at least 6 months. Automated visual fields demonstrated general depression in the left eye (mean deviation 25.6 dB, compared with 21.9 dB in the right eye) without focal visual field loss. Because optic disc edema is a common finding in patients with POEMS syn-drome, no further testing was performed. The patient was evaluated 4 days after acute vision loss in the left eye. Visual acuity was 20/40, right eye, and hand motions, left eye. Pupils were equal, round, and reactive to light with a left relative afferent pupillary defect. Color vision was normal on the right, but the patient could not identify any of the color plates with the left eye. The appearance of the optic disc edema was unchanged, and the fundi were otherwise normal. MRI of the orbits performed 3 days later revealed enlargement and enhancement of the left optic nerve and an adjacent enhancing lesion in the suprasellar cistern (Fig. 2). Lumbar puncture had an opening pressure of 17 cm H2O. Cerebrospinal fluid analysis demonstrated elevated protein of 131 mg/dL (normal, ,45 mg/dL), normal glucose, no pleo-cytosis, and no malignant cells. Steroid therapy was immediately reinitiated (single dose of 40 mg of dexamethasone followed by 20 mg weekly) and, Division of Neuro-Ophthalmology, Department of Ophthalmology and Visual Sciences (HEM), University of Illinois Medical Center, Chicago, Illinois; and Division of Neuro-Ophthalmology, Depart-ments of Neurology (GTL) and Ophthalmology (GTL), University of Pennsylvania School of Medicine, Philadelphia, Pennsylvania. The authors report no conflicts of interest. Address correspondence to Heather E. Moss, MD, PhD, Department of Ophthalmology, University of Illinois (MC 648), 1855 W. Taylor Street, Chicago, IL 60612; E-mail: hemoss@uic.edu Moss and Liu: J Neuro-Ophthalmol 2012; 32: 45-47 45 Clinical Observation Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. 2 weeks later, chemotherapy consisting of cyclophospha-mide, bortezomib, and dexamethasone was started. Vision in the left eye declined to no light perception and remained 20/40 in the right eye. One month later, the patient's ascites had decreased and his energy level had increased. Vision in the left eye remained no light perception while the right optic nerve remained mildly swollen, and the left optic nerve became flat without pallor. MRI per-formed 6 weeks after acute vision loss demonstrated persistent enlargement and enhancement of the left optic nerve, with pro-gressive enlargement of the mass lesion (Fig. 3). Follow-up imaging 5 months after presentation showed some regression of the mass, and biopsy was deferred. Ten months after presentation, the patient could count fingers with his left eye and MRI showed further reduction in the size of the suprasellar mass. DISCUSSION Screening for and evaluation of vision loss in POEMS syndrome is challenging since optic nerve edema is relatively common in POEMS syndrome occurring in 29% and 55% of patients (1,2). It is a minor criterion for the diagnosis of the syndrome. The etiology of optic nerve edema is not known in most cases. Some cases can be explained on the basis of increased CSF protein or high intracranial pressure (3). Microvascular etiologies have been proposed on the basis of high VEGF levels. Systemic interstitial volume over-load may also be a factor in patients associated with cystoid macular edema (4,5). Despite optic nerve edema being common in POEMS syndrome, vision loss is unusual (3). Rare instances of acute visual decline have been attributed to macular edema (4,5) and papilledema related to elevated intracranial pressure due to venous sinus thrombosis (6). We are unaware of previous reports of an intracranial mass lesion and optic nerve enhancement in POEMS syndrome. The presumed composition of the mass lesion is plasmacy-toma. The proposed pathophysiology of vision loss in our patient may be multifactorial. First, there may be compres-sion of the optic nerve similar to reports of POEMS syndrome associated with orbitopathy (7,8). Second, in an analogous fashion to vision loss due to IgG multiple mye-loma, tumor infiltration (9,10) and ischemia (9) by IgA osteosclerotic myeloma may have contributed to the optic neuropathy. Finally, nerve conductivity may have been decreased by IgA paraproteins (11). FIG. 1. Bilateral optic disc edema is present 2 weeks prior to acute left vision loss. FIG. 2. Seven days after loss of the vision in the left eye, FLAIR (A), contrast-enhanced T1 axial (B), and coronal (C) MRI demonstrate an enhancing lesion in the suprasellar cistern (arrowhead) with enlargement and enhancement of the adjacent left optic nerve (arrows). 46 Moss and Liu: J Neuro-Ophthalmol 2012; 32: 45-47 Clinical Observation Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. ADDENDUM A follow-up MRI 14 months after presentation showed complete regression of the suprasellar mass. The abnormal signal within the optic nerve persisted. Vision remained stable at count fingers with the left eye. This complete radiographic resolution following chemotherapy directed at POEMS syndrome supports the presumed pathology of plasmacytoma. Radiation to the area is planned to prevent regrowth. ACKNOWLEDGMENTS The authors thank Lisa Birmingham for her assistance with the figures. REFERENCES 1. Dispenzieri A, Kyle RA, Lacy MQ, Rajkumar SV, Therneau TM, Larson DR, Greipp PR, Witzig TE, Basu R, Suarez GA, Fonseca R, Lust JA, Gertz MA. POEMS syndrome: definitions and long-term outcome. Blood. 2003;101:2496-2506. 2. Nakanishi T, Sobue I, Toyokura Y, Nishitani H, Kuroiwa Y, Satoyoshi E, Tsubaki T, Igata A, Ozaki Y. The Crow-Fukase syndrome: a study of 102 cases in Japan. Neurology. 1984;34:712-720. 3. Bolling JP, Brazis PW. Optic disk swelling with peripheral neuropathy, organomegaly, endocrinopathy, monoclonal gammopathy, and skin changes (POEMS syndrome). Am J Ophthalmol. 1990;109:503-510. 4. Chong DY, Comer GM, Trobe JD. Optic disc edema, cystoid macular edema, and elevated vascular endothelial growth factor in a patient with POEMS syndrome. J Neuroophthalmol. 2007;27:180-183. 5. Imai H, Kusuhara S, Nakanishi Y, Teraoka Escano MF, Yamamoto H, Tsukahara Y, Negi A. A case of POEMS syndrome with cystoid macular edema. Am J Ophthalmol. 2005;139:563-566. 6. Witoonpanich R, Phankhian S, Jootar S, Poonyathalang A, Worapongpaiboon S, Phudhichareonrat S, Chanplakorn N. POEMS syndrome with venous sinus thrombosis and visual failure: a case report. J Med Assoc Thai. 2005;88:690-694. 7. Bourdette DN, Rosenberg NL. Infiltrative orbitopathy, optic disk edema, and POEMS. Neurology. 1984;34:532-533. 8. Gandhi D, Vashisht S, Mahajan A, Kapoor A, Berry M. Proptosis with orbital soft tissue and bone changes and unilateral papilloedema: unusual presentation of POEMS syndrome. Clin Imaging. 2000;24:193-196. 9. Yeung SN, Paton KE, Dorovini-Zis K, Chew JB, White VA. Histopathologic features of multiple myeloma involving the optic nerves. J Neuroophthalmol. 2008;28:12-16. 10. Fung S, Selva D, Leibovitch I, Hsuan J, Crompton J. Ophthalmic manifestations of multiple myeloma. Ophthalmologica. 2005;219:43-48. 11. Shimada Y, Shibuya M, Ohki R, Yoneya S, Nakamura Y. Bilateral optic neuropathy associated with multiple myeloma. J Neuroophthalmol. 2006;26:117-120. FIG. 3. Six weeks after vision loss in the left eye, contrast-enhanced T1 coronal (A) and axial (B) MRI shows enlargement of the suprasellar mass (arrowhead), while the appearance of the left optic nerve (arrow) is unchanged. Moss and Liu: J Neuro-Ophthalmol 2012; 32: 45-47 47 Clinical Observation Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. |