| OCR Text |
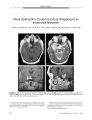
Show LETTERS TO THE EDITOR Editor's note: The Journal of Neuro- Opthalmology welcomes letters as written or e- mail correspondence. Send e- mail to: jdtrobe@ umich. edu. Optic Neuropathy without Retinopathy in AIDS and Cytomegalovirus Infection To the Editor: Optic neuropathy in AIDS is infrequent. When caused by cytomegalovirus ( CMV), it usually is accompanied by retinopathy. We have examined a 25- year- old patient with AIDS who presented with a right optic neuropathy without retinitis. She also had a right oculomotor nerve palsy and a lower limb polyradiculomyelopathy, subsequently attributed to opportunistic infection with CMV. Prompt treatment largely reversed the oculomotor neuropathy and polyradiculomyelopathy. A 25- year- old woman from Swaziland with newly diagnosed HIV infection complicated by esophageal candidiasis and profound weight loss presented with a 1- month history of a throbbing bilateral supraorbital and frontal headache. She also complained of blurred vision affecting her OD and binocular diplopia. Two weeks earlier she had noticed bilateral lower limb weakness, which was becoming progressively worse. There was no significant previous ocular history. Uncorrected Snellen visual acuities were 20/ 200 in the OD and 20/ 20 in the OS. There was no improvement with pinhole. She had a right relative afferent pupillary defect and dilated funduscopy revealed diffuse pallor of the right optic disc. Goldmann visual fields showed an inferior altitudinal defect in the OD and a full visual field in the OS. Ocular motility assessment demonstrated a complete right oculomotor nerve palsy. Tone and strength were normal in the arms and legs, and strength was normal in the arms. There was bilateral lower limb weakness, more marked on the right side. Sensation was impaired to light touch, pinprick, and temperature in the distribution of L3 to SI nerve roots. Vibration sense was diminished in the right leg, and joint position sense was diminished in both great toes. Upper and lower limb tone and reflexes were normal. Both plantar responses were flexor. A complete blood count revealed leukopenia of 2.2 x 109/ 1 ( normal range 4.0- 11.0 x 109/ 1) with a lymphocyte count of 0.3 x 109/ 1 ( normal range 1.3- 3.5 x 109/ 1). The CD4 lymphocyte cell count was 3 cells/ mm3 ( normal range 500- 1500 cells/ mm3). Human immunodeficiency virus ( HIV) ribonucleic acid ( RNA) viral load was 84,000 copies/ ml. Cerebrospinal fluid ( CSF) biochemistry showed a protein level of 0.98g/ l ( normal range 0.20- 0.40g/ l) and glucose level of 4.6mmol/ l. The CSF/ plasma glucose ratio was 0.77 ( normal ratio 0.66). CSF microscopy demonstrated the presence of 25 nucleated cells/ mm3, predominantly lymphocytes. No organisms were seen on Gram, india ink, or Ziehl- Neilson stains. Other negative studies included serology and CSF polymerase chain reaction for toxoplasma ( PCR), CSF cryptococcal antigen tests, prolonged CSF culture for Mycobacteria and Cryptococcus, serum IgM for Herpes Simplex virus and Varicella Zoster virus, and syphilis serology ( VDRL). PCR was positive for CMV in blood and CSF. On the basis of abnormal F waves, we diagnosed CMV polyradiculo- myelopathy of the cauda equina. The patient was treated with zidovudine, lamivudine, abacavir, and intravenous ganciclovir followed by twice monthly infusions of cidofovir with granulocyte colony stimulating factor ( GCSF) cover. Because of initial neurologic deterioration characterized by worsening of the bilateral lower limb weakness, adjunctive therapy was commenced with intravenous methylprednisolone 1 g per day for 4 days and 500 mg per day for 3 days. Two months later, her visual acuity and visual field had improved only slightly in the OD, but there was almost complete resolution of the right oculomotor nerve palsy and lower limb weakness. The CD4 cell count had risen to 6 cells/ mm3, HIV RNA viral load had fallen to 130 copies/ ml, and blood CMV PCR was negative. At her last review 6 months following initial presentation, her ophthalmic status was unchanged. She had gained 20 kg in weight, blood CMV PCR remained negative, HIV RNA viral load was < 80 copies/ ml, and CD4 count had risen to 70/ mm3. Patients with CMV optic neuropathy have been separated into three groups: 1) those with extensive retinitis and spread to the optic nerve; 2) those with juxtapapillary retinitis with spread to the optic nerve; and 3) those with primary optic nerve infiltration by CMV ( 1). The majority of cases of CMV optic neuropathy are of juxtapapillary retinal origin ( 1). Only rarely do patients with CMV retinitis develop, as our patient did, progressive loss of vision that is unaccompanied by retinitis and that is unassociated with optic disc swelling ( 1,2). This form of retrobulbar optic neuropathy associated with CMV is attributed to direct invasion of the retrolaminar portion of the optic nerve by the virus. Peter Cackett, MD, C. R. Weir, MD, Robert McFadzean, MD, R. A. Seaton, MD Princess Alexandra Eye Pavilion Edinburgh, Scotland peter@ pdcackett. demon. co. uk 94 JNeuro- Ophthalmol, Vol. 24, No. 1, 2004 Letters to the Editor JNeuro- Ophthalmol, Vol. 24, No. 1, 2004 REFERENCES 1. Walsh, Hoyt. Clinical Neuro- Ophthalmology. 5th Ed. Baltimore: Williams and Wilkins, 1998, 5107. 2. Harkins T, Maino JH. Cytomegalovirus retinitis complicated by optic neuropathy: a longitudinal study. J Am Optom Assoc 1992; 63: 21- 7. Postoperative Ophthalmoplegia and Ataxia due to Carbamazepine Toxicity Facilitated by Diltiazem To the Editor: We recently noted severe carbamazepine neurotoxicity likely facilitated by an interaction with diltiazem. A 47- year- old woman with bipolar disorder was admitted for aorto- iliac bypass surgery. Her bipolar disorder had been treated for years with carbamazepine 1600 mg/ d without side effects. On the first postoperative day, carbamazepine was restarted. She received one dose of 800 mg. Because of a sinus tachycardia, she was also started on diltiazem 120 mg/ d. On the second postoperative day, she developed confusion, agitation, and slurred speech. She was disoriented to place but following commands. There was a complete volitional and reflex ophthalmoplegia in all directions. The pupils measured 7 mm and constricted normally to light. There was a profound ataxic dysarthria and marked bilateral dysmetria with past finger pointing and rebound. The laboratory evaluation revealed normal findings except for a carbamazepine serum level of 26.2 micrograms per mL ( normal 3- 12 mg/ mL). After discontinuation of carbamazepine, she recovered horizontal eye movements within 24 hours, but she still had restricted vertical gaze. The pupils returned to normal size. The dysmetria was still noticeable on fmger- to- nose testing. The carbamazepine level had declined gradually to 15.2 micrograms/ ml. By the third postoperative day, all neurologic manifestations had resolved. The carbamazepine level had declined to 9.0 micrograms/ ml, within the normal range. MRI, including diffusion- weighted sequences, was normal. Although we anticipated an increase in the carbamazepine serum level after the introduction of diltiazem, our case is remarkable for the development of an extreme form of carbamazepine neurotoxicity/ 1- 3- 1 The calcium channel blocker diltiazem is well known to inhibit the P450 enzyme system. This attribute is shared with verapamil but not nifedipine. Severe neurotoxicity due to carbamazepine is typically associated with ataxia and nystagmus on neurologic examination. Vomiting and dysarthria usually are early clinical signs that prompt reduction of the dose. Diplopia is commonly noted, but complete ophthalmoplegia is a very uncommon presentation. In our review of the literature, only a few anecdotal reports were found.( 4' 5) In these cases, toxicity of carbamazepine was not caused by drug interaction but overdose.( 4) It is difficult to predict the individual response to this drug interaction, but when carbamazepine is used with a calcium channel blocker such as diltiazem or verapamil, the dose should probably be substantially reduced while awaiting serum levels. Eelco F. M. Wij dicks, MD Christopher Arendt, RPH Mark C. Bazzell, MD Departments of Neurology, Pharmacy, and Anesthesiology Mayo Clinic, Rochester, Minnesota wijde@ mayo. edu REFERENCES 1. Bahls FH, Ozuna J, Ritchie DE. Interactions between calcium channel blockers and the anti convulsants carbamazepine and phenytoin. Neurology. 1991; 41: 740- 742. 2. Shaughnessy AF, Mosley MR. Elevated carbamazepine levels associated with diltiazem use. Neurology. 1992; 42: 937- 938. 3. Brodie MJ, MacPhee GJ. Carbamazepine neurotoxicity precipitated by diltiazem. BMJ Clinical Research Ed. 1986; 292: 1170- 1171. 4. Mullally WJ. Carbamazepine- induced ophthalmoplegia. Arch Neurol. 1982; 39: 64. 5. Noda S, Umezaki H. Carbamazepine- induced ophthalmoplegia. Neurology. 1982; 32: 1320. Superior Oblique Myokymia Improved with Cabapentin To the Editor: We would like to report a patient in whom superior oblique myokymia ( SOM) has been successfully controlled with oral gabapentin therapy. A 65- year- old man presented to us with a 12- month history of vertical diplopia lasting for a few minutes, more noticeable when tired and on sudden change in gaze position. Slit lamp examination demonstrated low- amplitude high- frequency torsional movement of the OS, especially on prolonged dextroversion, a feature characteristic of SOM. There was no other ocular motility deficit. MRI of the brain and orbit was normal. The patient was commenced on oral carbamazepine 150 mg twice daily. This treatment was discontinued within 8 weeks due to perceived failure to control the manifestations. On a subsequent visit, oral carbamazepine was reintroduced in increasing dosage, reaching 300 mg three times daily over a period of 3 weeks. Despite the increased dose, the patient continued to have manifestations of SOM. Gabapentin was begun at 100 mg daily and increased to 300 mg daily over 3 days. On a visit 2 months later, the patient reported a noticeable improvement in his symptoms. Episodes of transient vertical diplopia were far less frequent. Symptomatic improvement has been maintained for over 12 months, and the patient has experienced no medication side effects. 95 JNeuro- Ophthalmol, Vol. 24, No. 1, 2004 Our case supports the assertion of Tomsak et al. ( 1) that oral gabapentin may be an effective treatment of SOM. Among their two cases, one was lost to long- term follow- up and the second case had only a 5- month telephone follow-up. Our patient's long- term relief of symptoms suggests that gabapentin may be a welcome addition to the treatment options for this rare condition. Sunil Deokule, FRCSEd Mike Burdon, MRCP, FRCS Tim Matthews, FRCS Birmingham & Midland Eye Center Birmingham, United Kingdom spdeokule@ hotmail. com References 1. Tomsak RL, Kosmorsky GS, Leigh RJ. Gabapentin attenuates superior oblique myokymia. Am J Ophthalmol 2002; 133: 721- 3. Recurrent Para- Infectious Third Nerve Palsy with Cisternal Nerve Enhancement on MRI To the Editor: We have examined a child with recurrent unilateral third cranial nerve palsy in whom magnetic resonance imaging ( MRI) demonstrated acute enhancement of the cisternal portion of the affected nerve. The first episode occurred in April, 2001, when the patient was 11 months old. Two weeks after hospitalization for viral pneumonitis, he developed complete right- sided ptosis and paresis of the extraocular muscles innervated by the third cranial nerve. The right pupil was 5 mm and sluggish; the left pupil was 3 mm and briskly reactive. The remainder of his neuro- ophthalmologic examination and cerebrospinal fluid analysis was normal. MRI showed enhancement of the oculomotor nerve at its exit from the brainstem ( Fig. la). After 3 days of intravenous methylprednisolone, the ptosis dramatically improved; after 2 months, the ophthalmoplegia and pupillary abnormalities had resolved. Repeat MRI was normal ( Fig. lb). The patient received no further medical treatment apart from that for amblyopia. In July 2003, at the age of 39 months, he developed a recurrent pupil- involving right third cranial nerve palsy following an acute viral gastroenteritis. Examination showed complete ptosis and paresis of the muscles innervated by the right third cranial nerve. The right pupil was 7 mm and sluggish, and the left pupil was 4 mm and briskly reactive to light. The remainder of the neuro- ophthalmologic examination was normal. Repeat MRI showed enhancement of the right third cranial nerve in a region identical to that implicated in the first 96 FIGURE 1. A. Axial T1 MRI reveals enhancement of the cisternal portion of the right third cranial nerve. B. Axial T1 MRI 2 months after onset of right third cranial nerve palsy shows complete resolution of the enhancement. © 2004 Lippincott Williams & Wilkins Letters to the Editor JNeuro- Ophthalmol, Vol. 24, No. 1, 2004 FIGURE 2. Axial T1 MRI during the second episode, occurring 2 years after the first, shows recurrent enhancement of the cisternal portion of the right third cranial nerve. episode ( Fig. 2). After 2 weeks of therapy with oral prednisolone, 5 mg three times daily, the ptosis and ophthalmoplegia slightly improved. Two months later, there was minimal ptosis and the ophthalmoplegia had completely resolved. Although postviral cranial neuropathies most commonly affect the sixth cranial nerve, involvement of the third cranial nerve has been reported ( 1- 6). MRI shows enhancement of the cisternal portion of the nerve. Similar enhancement occurs in ophthalmoplegic migraine ( 7- 9), neuroma ( 10), and meningitis ( 5). To our knowledge, this is the first report of recurrent para- infectious third cranial nerve palsy. Sayeda A. Nazir, BS, Scott A. Murphy, MD, R. Michael Siatkowski, MD Department of Ophthalmology Dean A. McGee Eye Institute University of Oklahoma College of Medicine, Oklahoma City, Oklahoma rmichael- siatkowski@ ouhsc. edu Acknowledgment Supported in part by an unrestricted grant from Research to Prevent Blindenss, New York, New York. REFERENCES 1. Miller NR. Solitary oculomotor nerve palsy in children. Am J Ophthalmol 1977; 83: 106- 11 2. Keith CG. Oculomotor nerve palsy in childhood. Aust N ZJ Ophthalmol 1987; 15: 181- 4. 3. Ohtsuka K. Enhanced magnetic resonance imaging in a patient with acute paralysis of the inferior division of the oculomotor nerve. Am J Ophthalmol 1997; 124: 406- 9. 4. Mark AS, Blake P, Atlas SW, et al. Gd- DTPA enhancement of the cisternal portion of the oculomotor nerve on MR imaging. Am J Neuroradiol 1992; 13: 1463- 70. 5. Carlow TJ. Oculomotor ophthalmoplegic migraine: is it really migraine? J Neuroophthalmol 2002; 22: 215- 21. 6. Hansen SL, Borelli- Moller L, Stange P, et al. Ophthalmoplegic migraine: diagnostic criteria, incidence of hospitalization and possible etiology. Acta Neurol Scand 1990; 81: 54- 60. 7. Prats JM, Mateos B, Garaizar C. Resolution of MRI abnormalities of the oculomotor nerve in childhood ophthalmoplegic migraine. Cephalgia 1999; 19: 655- 9. 8. Aers I, Van Zandijcke M, Dehaene I, et al. Magnetic resonance imaging in a case of migraine with ophthalmoplegia. Eur J Neurol 1997; 4: 85- 9. 9. Wong V, Wong WO Enhancement of the oculomotor nerve: a diagnostic criterion for ophthalmoplegic migraine? Pediatr Neurol 1997; 17: 70- 3. 10. Norman AA, Farris BK, Siatkowski RM. Neuroma as a cause of oculomotor nerve palsy in infancy and early childhood. J AAPOS 2001; 5: 9- 12. Bilateral Sixth Nerve Palsy in West Nile Meningoencephalitis To the Editor: We report a novel case of bilateral sixth nerve palsy associated with West Nile meningoencephalitis. A 73- year- old previously healthy man presented with vertigo, vomiting, headache, and fever. On examination, he was lethargic, confused, and febrile to 39.1° C ( 102.4° F). He was oriented to self, but not place or date. He was inattentive, followed simple commands only after repeated requests, and could not perform calculations. Although the patient had difficulty naming objects, he could recall the names of the president of the United States and the quarterback of the New England Patriots. General physical examination was notable for mild meningismus. On neurologic examination, bilateral sixth nerve palsies, with inability to abduct either eye past the midline, were present. A mild left facial nerve palsy was observed, with flattening of the nasolabial fold. The other cranial nerves were normal. Motor strength was normal, and without involuntary movements. Deep tendon reflexes were slightly diminished throughout, and the plantar responses were flexor. No release signs were observed. Cerebrospinal fluid ( CSF) examination revealed a leukocyte count of 56/ mm3 ( 84% polymorphonuclear, 14% lymphocytic) and red blood cell count of 2/ mm3. CSF glucose was normal, and CSF protein slightly elevated at 120 mg/ dl. Ampicillin, ceftriaxone, and acyclovir were administered. CSF cultures were negative for bacterial and fungal pathogens. CSF VDRT, Lyme antibody, cryptococcal antigen, and PCR for herpes simplex virus were also negative. CSF immunoglobulin M ( IgM) for West Nile virus, sent to the Massachusetts State Laboratory, was positive at 4.15 ( normal, < 2.0). 97 JNeuro- Ophthalmol, Vol. 24, No. 1, 2004 Magnetic resonance imaging of the brain without contrast was unremarkable. The patient defervesced over the next 3 days, and all antibiotics were discontinued. He was discharged to rehabilitation 9 days after admission with significant improvement in his mental status and cranial neuropathies. No residual neurologic deficits were present 6 months after hospital discharge. Neurologic syndromes associated with West Nile infection include meningoencephalitis, encephalitis, aseptic meningitis, cerebellar ataxia, flaccid paralysis, and a poliomyelitis- like syndrome. Autopsy studies have shown most severe inflammation in the medulla and cranial nerve roots ( 1- 3). No specific data are available on the prevalence and outcome of sixth nerve palsies in West Nile infection. In one study, cranial neuropathies were reported in two ( 11%) hospitalized patients with West Nile infection in New York and New Jersey in 2000, but neither had an ocular motor palsy ( 1). In the original New York City outbreak in 1999 ( 2), 13 of 59 ( 22%) hospitalized patients had cranial neuropathies, but ocular motor involvement was not specified. There is at least one previous report of sixth nerve palsy associated with West Nile infection. Vaispapir et al. ( 4) reported a patient with bilateral optic neuritis, right lateral rectus palsy, right facial nerve palsy, and cerebellitis. West Nile encephalitis also has been associated recently with anterior uveitis, vitritis, and chorioretinitis ( 5,6). Reports on the long- term outcomes of patients with West Nile meningoencephalitis are conflicting. In one study of hospitalized older patients with West Nile infection ( 7), 88% of survivors had regained baseline function 3 months after discharge. However, only 19% of patients had focal neurologic findings at presentation. By contrast, most survivors of the 1999 New York outbreak ( 8) had persistent manifestations 1 year later, including fatigue ( 67%), memory loss ( 50%), difficulty walking ( 49%), and muscle weakness ( 44%). West Nile virus infection reached epidemic proportions in the United States in 2002, with 3389 confirmed human cases ( 9). Physicians should suspect West Nile infection when patients present in the summer and fall months with fever and neurologic or ophthalmologic manifestations. John J. Ross, MD Michael G. Worthington, MD Division of Infectious Diseases Caritas Saint Elizabeth's Medical Center Boston, Massachusetts jrossmd@ cchcs. org References 1. Weiss D, Carr D, Kellachan J, et al. Clinical findings of West Nile virus infection in hospitalized patients, New York and New Jersey, 2000. EmergInfect Dis 2001 ; 7: 654- 8. 2. Nash D, Mostashari F, Fine A, et al. The outbreak of West Nile virus infection in the New York City area in 1999. New Engl J Med 2001; 344: 1807- 14. 3. Leis AA, Stokic DS, Polk JL, Dostrow V, Winkelmann M. A poliomyelitis- like syndrome from West Nile virus infection. NEngl J Med 2002; 347: 1279- 80. 4. Vaispapir V, Blum A, Soboh S, Ashkenazi H. West Nile virus meningoencephalitis with optic neuritis. Arch Intern Med 2002; 162: 606- 7. 5. Bains HS, Jampol LM, Caughron MC, Parnell JR. Vitritis and chorioretinitis in a patient with West Nile virus infection. Arch Ophthalmol 2003; 121: 205- 7. 6. Adelman RA, Membreno JH, Afshari NA, Stoessel KM. West Nile virus chorioretinitis. Retina 2003; 23: 100- 1. 7. Berner YN, Lang R, Chowers MY. Outcome of West Nile fever in older adults. J Am Geriatr Soc 2002; 50: 1844- 6. 8. Petersen LR, Marfin AA. West Nile virus: a primer for the clinician. Ann Intern Med 2002; 137: 173- 9. 9. Centers for Disease Control and Prevention. Provisional surveillance summary of the West Nile virus epidemic- United States, January- November 2002. MMWRMorbMortal WklyRep 2002; 51: 1129- 33. Unilateral Pallid Optic Disc Swelling and Anemia Associated with Interferon Alpha Treatment To the Editor: In a recent Journal of Neuro- Ophthalmology article, Vardizer et al. ( 1) reported two patients with anterior ischemic optic neuropathy ( AION) in association with interferon alpha ( INF a) treatment. Including their article, eight reports of INF a- associated optic neuropathy photographically depict the optic disc swelling ( 1- 8). In none of these reports, however, was the optic disc swelling markedly pallid in a pattern akin to that of arteritic AION. I recently examined a 32- year- old woman with a history of hepatitis C and chronic iron deficiency anemia who had developed acute visual loss in the OS 1 week before examination. She had begun treatment with pegylated ( PEG) INF a 120 iig/ w by subcutaneous injection and ribavirin 1000 mg/ d orally 48 weeks before presentation. Her final doses of INF a and ribavirin were administered the day after the onset of visual symptoms. Hemoglobin at the onset of treatment was 12.0 g/ dL. Two months before initial ophthalmic examination, her hemoglobin had decreased to 10.6 g/ dL, and 1 month before examination to 9.4 g/ dL. Visual acuity was 20/ 20 OD and 20/ 50 OS with a prominent left relative afferent pupillary defect. Automated perimetry was normal in the OD and showed only a supe-ronasal island of visual field remaining in the OS. Ophthalmoscopy revealed a congenitally anomalous optic disc on 98 © 2004 Lippincott Williams & Wilkins Letters to the Editor JNeuro- Ophthalmol, Vol. 24, No. 1, 2004 FIGURE 1. Fundus photography reveals a congenitally anomalous right optic disc with an overlying glial tuft and marked pallor and swelling of the left optic disc with cotton wool spots inferior to it. the right, with a single cotton wool spot just outside the superotemporal vascular arcades, and markedly pallid optic disc edema with cotton wool spots just inferior to the optic nerve head on the left ( Fig. 1). Her hemoglobin was 8.3 g/ dL, and contrast- enhanced magnetic resonance imaging ( MRI) of the brain and orbits and magnetic resonance venography ( MRV) of the head were normal. There was no evidence of coagulopathy or vasculitis, but she had findings consistent with iron deficiency anemia. She was treated with intravenous dexamethasone 20 mg/ d for 3 days and iron sulfate 325 mg orally three times per day. Six weeks later, her left optic disc was pale without cupping, with resolving parapapillary hemorrhage. Her hemoglobin had increased to 10.1 g/ dL. I suspect that my patient's optic disc appeared more ischemic due to the superimposed anemia. Hepatitis C treated with INF a and ribavirin has been associated with anemia ( 9). Six of the eight prior reports depicting the optic disc swelling related to INF a noted that the complete blood count was normal ( 1- 6), and in two others the blood counts were not reported ( 7,8). Optic disc swelling from INF a may have differing appearances, most likely related to the degree of ischemia. In patients treated with INF a who develop pallid optic disc edema, underlying anemia should be suspected and a complete blood count obtained. Rod Foroozan, MD Cullen Eye Institute Baylor College of Medicine Houston, Texas References 1. Vardizer Y, Linhart Y, Loewenstein A, et al. Interferon- alpha-associated bilateral simultaneous ischemic optic neuropathy. J Neuro- Ophthalmol 2003; 23: 256- 9. 2. Purvin VA. Anterior ischemic optic neuropathy secondary to interferon alfa. Arch Ophthalmol 1995; 113: 1041- 4. 3. Norcia F, Di Maria A, Prandini F, Redaelli C. Natural interferon therapy: optic nerve ischemic damage? Ophthalmologica 1999; 213: 339^ 10. 4. Lohmann CP, Kroher G, Bogenrieder T, et al. Severe loss of vision during adjuvant interferon alfa- 2b treatment of malignant melanoma. Lancet 1999; 353: 1326. 5. Gabler B, Kroher G, Bogenrieder T, et al. [ Severe, bilateral vision loss in malignant melanoma of the skin. Anterior ischemic optic neuropathy with irreversible vision and visual field loss in adjuvant interferon alfa- 2b therapy]. Ophthalmologe 2001; 98: 672- 3. 6. Gupta R, Singh S, Tang R, et al. Anterior ischemic optic neuropathy caused by interferon alpha therapy. Am J Med 2002; 112: 683- 4. 7. Ockenfels M, Lisch W. [ Ocular complications of adjuvant interferon therapy for malignant melanoma: a review]. Hautarzt 2003; 54: 144- 7. 8. Schulman JA, Liang C, Kooragayala LM, King J. Posterior segment complications in patients with hepatitis C treated with interferon and ribavirin. Ophthalmology 2003; 110: 437- 42. 9. Sulkowski MS. Anemia in the treatment of hepatitis C virus infection. Clin Infect Dis 2003; 37 Suppl 4: S315- 22. 99 |