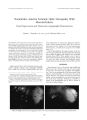
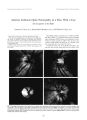
| OCR Text |
Show Jmmutl ,•! Xc '•(> l> luli, ilmi l, S7 I'll. / W. o IW8 l. i| ipincull Willi. mis , V Wilkins. Philadelphia Intracranial Ewing's Sarcoma Valerie Biousse, M. D., Nancy J. Newman, M. D., Andrew G. Lee, M. D., Eric Eggenberger, D. O. James R. Palrinely. M. D.. and David Kaufman. D. o. Three patients witli intracranial fiwing's sarcoma had neuro-ophthahnologic manifestations. In one patient, the primary tumor was in the skull and in two. it involved the long bones. Two patients complained of intermillenl headache associated with bilateral, transient visual symptoms suggestive of migraine, which prompted imaging thai showed occipital metastases. The third patient hail an orbital syndrome. Key Words: Ewing's sarcoma- Migraine- Visual field defect. Ewing's sarcoma is one of the most common bone tumors ( I). It can involve intracranial structures by direct extension from a primary lesion in the skull or. more frequently, it is a brain metastasis. Clinical manifestations depend on the location of the lesion. We report three patients who bad intracranial Fwing's sarcoma with ncuro- ophlhalmologic manifestations. CASK KKPORTS Case 1 A 15- year- old boy complained of headache associated with black spots in the vision. His medical history was remarkable for a frontoparietal skull tumor diagnosed as primary Fwing's sarcoma in July 1994 ( Fig. I A). Me underwent extensive resection and a year of chemotherapy and local radiation therapy. On completion of therapy in August 1995, he was in complete remission. In May 1996, he had extensive reconstructive surgery Manuscript received September IW7; accepted January I'WS. I'Vcm the Departments of Ophthalmology, and Neurology. Kmorv I ' Diversity School of Medicine iV. B.. W. I. N, i. Atlanta, Georgia; the Departments of Ophthalmology ( A. O. I... J. R. P.). Neurology ( A. G. I..). Neurosurgery ( A. G. I..), anil Plastic Surgery ( J. R. P.). Baylor College of Medicine, I touslon. Texas; the Division of Neurosurgery. M. I). Anderson Cancer Center. The University of Texas ( A. G. I..). Houston. Texas; and the Unit tor Neuro- Visual Disorders ( U. H.. D. K.). Michigan Stale I ' niversilN. Hast Lansing. Michigan. U. S.. A. Supported in part by an unrestricted grant to the Hmory liye Center. Hinory University School of Medicine, and to the Cullen live Institute. Bavlor College of Medicine from Research to Prevent Blindness. New York. New York. Address correspondence and reprint requests to Dr. Nancy .1. Newman. Nemo- Ophthalmology Unit, hinory live Center. I365.- B Chiton Road NH. Atlanta. GA 303: 2. U. S. A. with good results. One month after the reconstructive surgery, he began to see bright spots in front of both eyes, lasting several minutes and followed by left- side headache, described as a sharp pain lasting a few hours to a whole day. The spots were always followed by headache, but headache could occur without the spots. By August 1996, he was experiencing one episode of headache a day. Ibuprolen aborted the headache when taken as soon as the headache started, and thereafter he experienced no visual phenomena for 3 weeks before referral. His mother and maternal grandmother had a history of migraine, and his cousin had a history of Ewing's sarcoma. On examination ( September 1996), he appeared healthy. Vision was 20/ 15 Ol) and 20/ 20 OS. with 12/ 14 Ishihara color plates correctly identified in both eyes. Orbital, lid. and slii lamp examination findings were unremarkable. Pupils were normal and motility was full. Dilated funduscopy showed slight disc swelling in both eyes. Humphrey visual fields ( 24- 2) showed a small single spol of depression just to the right of the vertical meridian in both eyes ( Fig. IB). Humphrey visual fields ( 10- 2) showed a small right homonymous scolomatous deled ( Fig. IC). Findings in neurologic examination were normal, as were those in the patient's general examination. ' I' 1- weighted magnetic resonance imaging of the brain ( September 5, 1996) showed a curvilinear area of high signal with associated enhancement of the left occipital lobe and adjacent dura ( Fig. ID) that was new since the previous magnetic resonance imaging study of January 1996. Lumbar puncture showed 38 mm lymphocytes with mildly elevated protein ( 59 mg/ dl). normal glucose concentration, negative cultures, and negative findings in cytologic analysis. The patient's headache continued, and computed tomographic scan of the brain ( September 16) revealed a cerebral hemorrhage of the left occipital lobe. The following day, the occipital lesion was resected and proved to be an infiltrating, small, blue- cell neoplasm consistent with his previously diagnosed Fwing's sarcoma and confirmed by immunohislochemical stains. Adjacent meninges were not infiltrated by the tumor. He subsequently received radiation therapy to the tumor bed. as well as three cycles of chemotherapy. Subsequent IH7 188 V. BIOUSSE ET AL. vC & 4?* ® M yw \^ B E9ff.- Pv'• '^ » ^ H m • • • urn- • • • • • • e D •" " A, " * ,8, " kS" •! - 3 -; I - 5 - 13 - 15 - J! m i • a M p ,11, « , | 8 , , f l , » A i, * ,9, a » J , 5*, 4t: i :•;;,;. - rU- - - - • • • • • • FIG. 1. Case 1. A: Coronal T1- weighted magnetic resonance imaging of the brain after the administration of gadolinium showing a frontoparietal tumor consistent with primary Ewing's sarcoma of the skull. B: Axial T1 - weighted magnetic resonance imaging of the brain after the administration of gadolinium showing a curvilinear area of high signal with associated enhancement of the left occipital lobe and adjacent dura. C: Humphrey visual fields ( 24- 2) showing a single spot of depression just to the right of the vertical meridian in both eyes. D: Humphrey visual fields ( 10- 2) showing a small, right- side homonymous scotomatous defect. J Neum- Ophllwlmol, Vol. IK, No. 3, 1998 IXTRACRAMAI. i:\ VINcrS SARCOMA M' 9 FIG. 2. Case 2: Axial T1 - weighted magnetic resonance imaging of the brain before and after the administration of gadolinium, showing a 2.5- cm enhancing lesion with surrounding edema and mild mass effect in the right posterior parietal-occipital lobes, consistent with a metastatic lesion. high- dose chemotherapy followed by autologous blood stem cell transplantation was planned. Case 2 A 2 I- year- old woman had headache associated with positive visual phenomena in October 1994. Her medical history was significant for Ewing's sarcoma of the right tibia, diagnosed in I WO and treated with resection and chemotherapy. A local relapse in 1992 was treated with excision, chemotherapy, and radiation therapy. The patient remained well until October 1994 when headache developed, associated with nausea, photophobia, and shimmering lights leading to " patchy vision." The hcailaclics responded to aspirin. She remained active as a college student; there was no anorexia or weakness. Her maternal aunt, grandmother, and a cousin hail a history of migraine headaches. In January 1995. she experienced a severe headache with " blind spots" and blurred vision that occurred in association with her menses. Ncuro- ophlhalmologic examination ( January 1995) revealed visual acuity of 20/ 1? OU and normal color vision in both eyes. Orbital, lid, and slit lamp examination findings were normal. Pupils were normal and motility was full. Dilated funduscopy revealed normal discs without edema, and the vessels and macula were unremarkable in both eyes. Results of ( loklmann perimetry were normal in both eyes. Magnetic resonance imaging of the brain re\ ealed a 2.5- cm enhancing lesion with surrounding edema and mild mass effect in the right posterior parietal occipital lobe, consistent with a metastatic lesion ( big. 2). She came to the emergency department 48 hours later with acute worsening of headache and lethargy. A computed tomographic scan revealed hemorrhage into ( he tumor site. While in the emergency department, a waxing anil waning level of consciousness was noted with a left homonymous hemianopia. She subsequenlh showed right third nerve palsy and left hemiparesis with stupor. She was intubated anil treated with mannitol anil ilexa-methasone. A chest radiograph revealed a right mediastinal mass. The patient remained in a coma receiving ventilatory assistance and showed a dilated and light-fixed right pupil tor the next 4 days. Her condition then improved, and she was exlubated and could converse appropriately. Radiation therapy was delivered to the brain and lung. She died several months later with widespread systemic metastases. Case 3 A 30- year- old man had a right- side temporal mass, right proptosis. and diplopia. His medical history was remarkable for Hwing's sarcoma of the left forearm diagnosed in September 1994 after a 7- month history of pain anil forearm swelling. At that lime, he had an extensive metastatic evaluation that showed pulmonary nodules, and he underwent six cycles of chemotherapy. On examination in March 1995. \ ision was 20/ 60 - 2 Ol) and 20/ 20 OS. Results of an Ishihara lest of color vision were 8/ 14 Ol) and 14/ 14 OS. External examination showed 7 mm of proptosis on the right with hypo-globus of the right globe. Slit lamp examination results were unremarkable. Intraocular pressure was 24 mm Hg Ol) and 16 mm Hg OS. Pupils were normal. Motility examination showed a deficit in all directions in the right eye; the left eye moved normally. Dilated funduscopy showed choroidal folds in the right macula. Optic discs were normal. Visual fields were full to confrontation. A computed tomographic scan of the head showed a destructive soft tissue mass involving the greater wing of the right sphenoid bone and lateral orbital wall ( big. 3). The mass extended posteriori) into the subcutaneous soft tissues of the right temporal fossa with a soft tissue component extraconally involving the right orbit and resulting in medial displacement of the right lateral rectus muscle. The mass was in direct continuity with the brain. Extensive " sunburst" calcifications were noted, thought to be consistent with ( he patient's diagnosis of metastatic Ewing's sarcoma ( big. 3A. 3B, anil } C). The brain was otherwise unremarkable. One month later, his visual acuitv was 20/ 80 Ol). and he had a right relative afferent pupillars defect, worsening ophthalmoplegia, and choroidal folds in the right eye. 190 V. BIOUSSE ET AL. 9 ^ ^ K ; v3W If * » m_ : KE% ^ flfc&^ W^^ - B^^ Ba • L "* aBj FIG. 3. Case 3. Axial computed tomographic scan views of the brain and orbits ( with contrast) showing a destructive soft tissue mass involving the greater wing of the right sphenoid bone and lateral orbital wall. Note the posterior extension of the mass into the subcutaneous soft tissues of the right temporal fossa with a soft tissue component extraconally involving the right orbit ( A, B) and resulting in medial displacement of the right lateral rectus muscle ( B). The mass is in direct continuity with the brain ( C). The patient was treated again with chemotherapy and subsequently underwent orbital radiotherapy. Five months later ( September 1995), his visual acuity was 20/ 50 OD, and he had a persistent relative afferent pupillary defect. His ocular motility still showed moderately impaired ductions in all directions of gaze in the right eye, but the proptosis had improved ( 3 mm). The patient was subsequently lost to follow- up. DISCUSSION These three patients had Ewing's sarcoma metastatic to the brain, and manifested neuro- ophthalmologic symptoms and signs. Ewing's sarcoma is the second most common primary bone tumor in children and the fourth most common malignant tumor of the bone ( 1). It belongs to a group of small, round- cell neuroectodermal- ./ NniiihOphllmlmol, Vol. / « . No. J, 1998 INTRACRANIAL EWING'S SARCOMA 191 derived tumors and also includes primitive ectodermal tumor, atypical Hwing's tumor. Askin's tumor, and neuroepithelioma. Cytogenetics and immunocylochemistry help to differentiate these tumors from lymphoma and embryonal cell rhabdomyosarcoma ( 1,2). Ewing's sarcoma most often occurs in the long bones of the extremities and in the pelvis ( 1,2). In one patient ( case I) the primary tumor was in the skull, and in two ( cases 2 and 3) it involved the long bones. The skull is a rare primary site for Ewing's sarcoma. No more than 20 cases of primary Hwing's sarcoma of the skull have been reported to date ( 3- 10). It can involve the cranial vault, the cranial base, or the orbit. Symptoms at the time of diagnosis include local swelling of the scalp associated with headache, and papilledema related to raised intracranial pressure. Eventually, focal neurologic or orbital symptoms and signs develop, depending on the location of the tumor. Increased intracranial pressure can be explained by compression of the venous sinuses by the tumor, by local tumor involvement of the adjacent meninges and brain, or by diffuse sarcomatous meningitis ( 3- K)). Metastatic disease in Hwing's sarcoma is common, occurring in as many as 70% of cases within the first year of diagnosis ( 1.2). Metastases are usually to the lung and soft tissues. However, late brain metastases are becoming more frequent. Current systemic chemotherapeutic regimens may protect the more usual systemic sites, thereby allowing the patient to live longer, but these agents cross the blood- brain barrier poorly ( 1,2). Patients in cases 2 and 3 had brain involvement from metastatic disease occurring within 1 year after diagnosis of the primary long bone tumor. In patient 1, the primary skull tumor was followed I year later by a brain metastasis to the occipital lobe. There was no involvement of the adjacent occipital bone and meninges. There was also no recurrence of tumor in the frontoparietal region. Repeated cytologic examination of the cerebrospinal fluid revealed no evidence of sarcomatous meningitis. We found no previous reports of brain metastases from primary Hwing's sarcoma of the skull. The occipital location and intratumoral hemorrhage so strikingly similar in two of our patients ( cases 1 and 2) is not a previously noted pattern among other reported cases of Hwing's brain metastases ( 1.3). In two patients ( cases I and 2). migraine- like symptoms prompted imaging that revealed occipital metastases. Both patients complained of intermittent headache associated with bilateral transient visual symptoms. Both had a familial history ol" migraine, and both patients' symptoms improved with the usual antimigraine treatments. The findings ol" mild disc edema and small homonymous central scolomata in patient I prompted neuroimaging, whereas in patient 2, findings in a neuro-ophthalmologic examination were normal. It is well known that migraine- like symptoms can be triggered by a brain lesion, especially if the patient has a propensity to true migraine ( that is, a preset low headache threshold) ( I 1,12). Migraine may be a constitutional predisposition of the neurovascular system to react excessively to internal or external stimuli by a pattern ol" hyperactivity of the brain and ol" the trigeminal vascular system ( 13). Hdmeads ( 13) and Moskowitz ( 14) suggested that the trigeminal vascular system is the final common pathway, not only for migraine, but for many other types of head pain that might be induced by neural impulses from the brain caused by a brain lesion, whatever its origin. Associated activity in the brain may produce typical migrainous symptoms such as visual aura when the lesion is occipital ( 1.3). The treatment of Hwing's sarcoma consists of multidrug chemotherapy followed by surgery, radiation, or both. Improvement in diagnosis and treatment has increased the 5- year survival rate for patients with Hwing's sarcoma to more than l( Y'/< ( 1,2). However, treatment of primary lesions localized to the skull and of metastatic lesions to the brain remains difficult. REFERENCES 1. Vlasak R, Sim H. living's sarcoma. I'nlialr Orlhop Oncol 1996: 27: 591 603. 2. ( iranowcltcr L. Hwing's sarcoma and extracranial peripheral neuroectodermal tumors. Curr Opin Oncol 1995; 7: 355- 60. 3. Mchata Y. Ilendrickson l'' R. C'NS involvement in liwinsa sarcoma. Cancer 1974: 33: 859 62. 4. Carroll R. Miketie I.. Hwing's sarcoma of the temporal hone: CT appearance. ./ Compiil Assist I'oino^ r 1987; I 1: 362- - 3. 5. Ilawaixl l). l, Lund V. I. Primary Hwing's sarcoma of the ethmoid hone. ./ I. nrvnvol Olol 1985: 99: 1019 23. 6. Mansfield . IB. Primary Hwing's sarcoma of the skull. Sur^ Ncnrol 1982: 18: 286 8. 7. Mishra I Hi, I laran RP, Joseph '[', Chandi SM. Primary Hwing's sarcoma of the skull. A report of two cases. /> Y ./ Neitrosurx 1993; 7: 683-- 6. 8. Sleinhok P. Hlodnutrk (), Norman MCI. Chan KW, Hugh HryerCS. Primary Hwing's sarcoma of ( he hase of the skull. Neurosurgery 1986: 19: 104- 7. 9. Watanabc 11. Tsubohawa ' I'. Kalayama Y. Koyaiua S. Nakamura S. Primary Hwing's sarcoma of the temporal bone. Suri; Neurol 1992; 37: 54- 8. 10. Alverez- licrdecia A. Scluu L. Bruce DA. Localized primary intracranial Hwing's sarcoma of the orbital roof. ,/ Ncurosur^ 1979: 50: 811- 3. 1 I. Olcsen .1. The secondary headaches. In: Olescn .1. Tfell Hansen P. Welch KMA. eds. The Headaches. New York: Raven Press. 1993: 619 21. 12. Horsyth PA. PosnerJB. the secondary headaches. Intracranial neoplasms. In: Olescn .1, Tfell- I lanscn P, Welch KMA, cds. The Headaches. New York: Raven Press. 1993: 705 14. 13. Hdmeads .1. Migraine: disease or s\ ndromc? I'aihol Biol 1992: 40: 279- 83. 14. Moskowitz MA. The visceral organ brain: implications for the pathophysiology of vascular headache. Neurology 1991 ; 4 I: I 82 - 6. ./ Keimi <> I> IIIII, IIIIIIII. Vol. IS, ,\ o, .1, IWS |