| OCR Text |
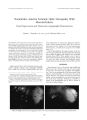
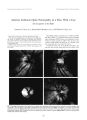
Show Journal of Nntro- Opluhalmology 18( 3): 176- 177, 1998. © 1998 Lippincoll Williams & Wilkins, Philadelphia Elevation of Serum Tumor Marker CA 15.3 Levels as the First Manifestation of Metastatic Breast Cancer to the Cavernous Sinus Rangram Chandran, M. D., and Andrew G. Lee, M. D. We report rising tumor marker levels of CA 15.3 as the presenting manifestation of metastatic breast cancer to the cavernous sinus and orbit. A 39- year- old woman with a history of breast cancer developed increasing levels of tumor marker CA15.3. Ten months later, she developed vision loss in the right eye, diplopia, and right- sided ptosis. A magnetic resonance scan of the head showed a mass involving the right cavernous sinus and superior orbital fissure. Biopsy of the lesion showed metastatic breast cancer. She was treated with surgery and radiotherapy and did well. Ophthalmologists should be aware of the significance of increasing levels of tumor markers, such as CA 15.3, in patients with a history of breast cancer and new neuroophthalmologic signs or symptoms. Key Words: CA 15.3- Breast cancer- Cavernous sinus. CA 15.3 is a glycoprotein tumor marker that is used in monitoring for the relapse of breast cancer ( 1,2). We report elevation of CA 15.3 as the presenting sign of metastatic breast cancer to the cavernous sinus. CASE REPORT A 39- year- old patient was diagnosed with adenocarcinoma of the breast in 1991 and underwent a left modified radical mastectomy, chemotherapy, and radiotherapy. The results of a complete metastatic evaluation at that time were negative. She did well until May 1995, when serial routine tumor- associated antigen CA 15.3 measurements demonstrated elevated levels at 113 U/ ml ( normal < 31 U/ ml) that remained elevated over a 7- month period. Results of metastatic evaluation in December 1995, including chest radiograph, bone scan, Manuscript received June 1997; accepted November 1997. From the Departments of Ophthalmology, Neurology, and Neurosurgery ( A. G. L.), Baylor College of Medicine ( R. C.), Houston, Texas, and the Division of Neurosurgery, University of Texas, M. D. Anderson Cancer Center, Houston, Texas ( A. G. L.). Address correspondence and reprint requests to Dr. Andrew G. Lee, Department of Ophthalmology, Baylor College of Medicine, 6565 Fannin St., NC- 205, Houston, Texas 77030, U. S. A. computed tomography ( CT) scan of the chest, abdomen, and pelvis, and magnetic resonance ( MR) imaging of the head, were negative. She was otherwise healthy. Her only medication was megestrol acetate. In January 1996 she reported new binocular vertical diplopia and ptosis of the right upper lid. In March 1996, she noted painless progressive loss of vision in the right eye and worsening diplopia. She was referred to the neuroophthalmology service on March 25, 1996, and was found to have visual acuity of 20/ 100 in the right eye and 20/ 20 in the left eye. The pupils measured 4 mm in the right eye and 3 mm in the left eye with a sluggish response to light in the right eye and a normal response to light in the left eye. There was a right relative afferent pupillary defect. Hertel exoph-thalmometer measurements showed 18 mm in the right eye and 16 mm in the left eye. Kinetic visual field testing by Goldmann technique showed a superotemporal quadrantic defect extending to central fixation in the right eye. The visual field of the left eye was normal. Motility examination showed a mild deficit in elevation of the right eye with a hypotropia of five prism diopters in the right eye in primary gaze and 30 prism diopters of right hypotropia in upgaze. The right optic nerve was diffusely pale. The left optic nerve was normal. An MR scan showed an infiltrative mass lesion involving the right cavernous sinus, orbital apex, and superior orbital fissure. A craniotomy was performed on April 1, 1996, and biopsy of the cavernous sinus region showed metastatic breast adenocarcinoma. The patient underwent 5,000 cGy of whole brain radiotherapy and chemotherapy. Postoperatively, the CA 15.3 levels decreased to 43 U/ ml. On October 9, 1996, the patient had no diplopia or ptosis. The visual acuity was 20/ 20 in the right eye. There was a persistent unchanged visual field defect in the right eye, a relative right afferent pupillary defect, and only mild underaction of elevation in the right eye. In May 1997, results of the patient's ophthalmologic examination were stable. Neuroimaging showed resolution of the abnormal infiltrative mass, but there was slight fullness of the right cavernous sinus area and postoperative changes in the right frontal region. 776 TUMOR MARKER CA 15.3 LEVELS 177 DISCUSSION Up to 50% of patients with breast cancer will develop distant metastasis within 5 years of primary treatment ( 1,2). Breast cancer remains a main cause of death due to malignancy in the United States, and early detection of metastasis is critical because survival may be improved by earlier treatment of a smaller metastatic tumor mass ( 1- 3). In addition, breast cancer is the most common metastatic tumor to the ocular structures ( 3). There are a number of tumor markers used to detect metastatic breast cancer. Carcinoembryonic antigen ( CEA) was one of the earliest antigenic glycoprotein tumor markers ( 1,2). Other classes of high molecular weight glycoproteins/ mucins or mucinlike components have been reported as useful tumor markers. It is hypothesized that these markers are released into the circulation by the loss of functional polarity of tumor cells and the disruption of normal tissue architecture ( 1- 3). Monoclonal antibodies that react with breast cancer- associated mucins also have been developed. These include CA 15.3, mucinlike carcinoma- associated antigen ( MCA), and CA 549. Unfortunately, CA 15.3 and CEA are not specific for breast cancer, and benign entities may cause elevation of these markers. Nevertheless, overall sensitivity for these tumor markers in detecting metastatic breast cancer may be as high as 45% for CEA, 59% for MCA, and 80% for CA 15.3 ( 1). Molina et al. reported a sensitivity of CA 15.3 of 40% and a lead time before diagnosis of 4.2 ± 2.3 months. These authors felt that these tumor markers were " useful tools in early diagnosis of recurrence." Bullock and Yanes reported 30 patients with metastatic breast cancer and ophthalmic manifestations, including cranial nerve involvement ( nine patients), brain involvement with papilledema ( one patient), Horner's syndrome ( seven patients), choroidal tumor ( four patients), and orbital tumor ( 10 patients). CEA was elevated in 18 of 22 patients. The mean interval from diagnosis of breast cancer to the onset of ophthalmic signs was 4.9 years, and ophthalmic signs were the first evidence of metastatic disease in 27% of cases ( 3). Martoni et al. reported CA 15.3 to have a specificity of 99%, and CA 15.3 levels were found to be elevated in 41% of 201 patients before the clinical diagnosis of recurrence. In fact, CA 15.3 levels may be elevated for > 6 months before any clinical evidence of relapse ( 1). In our patient, increasing CA 15.3 levels were detected 10 months before the clinical finding of metastatic breast cancer. A complete metastatic evaluation, including neu-roimaging, performed at the lime of increasing CA 15.3 levels failed to demonstrate metastatic disease. The onset of neuroophthalmic signs or symptoms in such a patient should therefore be considered as metastatic disease until proven otherwise. Although promising, the role of tumor- associated antigens in screening for metastatic disease remains to be completely defined. Nevertheless, patients with ophthalmic signs suggestive of metastatic breast cancer should undergo a complete metastatic evaluation including tumor markers, such as CA 15.3. Ophthalmologists should be aware of the clinical significance of increasing tumor marker levels such as CA 15.3 in patients presenting with neuroophthalmic signs or symptoms. Acknowledgment: This work was supported in pari by a grant from Research lo Prevent Blindness, Inc., New York, NY. REFERENCES 1. Martoni A, Zamagni C, Bcllanova B, et al. OKA, MOA, OA 15.3 and CA 549 and their combinations in expressing and monitoring metastatic breast cancer: a prospective comparative study. Ear .1 Cancer 1995; 31: 1615- 21. 2. Molina R, Zanon G, Kilella X, et al. Use of serial carcinoembryonic antigen and CA 15.3 assays in detecting relapses in breast cancer patients. Breast Cancer Res Treat 1995: 36: 41- 8. 3. Bullock JI). Yanes B. Ophthalmic manifestations of breast cancer. Ophthalmology 1980; 10: 961- 73. .1 Neuro- Ophtlwlmnl, Vol. IS. Ni>. .1. 1998 |