| OCR Text |
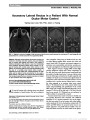
Show Papilledema as the Initial Presentation of Castleman Disease Guohong Tian, MD, PhD, Yun Jing, MD, PhD, Hanqiu Jiang, MD, PhD, Jingwen Wang, MD, PhD, Xiaojun Zhang, MD, PhD Abstract: Castleman disease is a rare lymphoproliferative disorder that has many presentations ranging from unifocal or multifocal mass lesions to a monoclonal gammopathy. It has features that may overlap with osteosclerotic myeloma or POEMS (polyneuropathy, organomegaly, endocrinopathy, M protein, skin changes) syndrome. We report a patient with papilledema, enlarged lymph nodes, and monoclonal IgG, who subsequently developed a polyneuropathy. Biopsy of enlarged mediastinal lymph nodes confirmed the diagnosis of Castleman disease. Journal of Neuro-Ophthalmology 2014;34:169-172 doi: 10.1097/WNO.0000000000000096 © 2014 by North American Neuro-Ophthalmology Society Castleman disease, also known as angiofollicular lymph node hyperplasia or giant lymph node hyperplasia, is characterized by over growth of lymph node tissue at a single site or throughout the body. It can mimic a number of benign and malignant disorders, including POEMS (polyneurop-athy, organomegaly, endocrinopathy, M protein, skin changes) syndrome, lymphoma and myeloma. The initial presentation of papilledema without evidences of polyneur-opathy and skin lesions differentiates our patient from POEMS syndrome, although peripheral nerves were involved at a later stage of the clinical course. CASE REPORT A 28-year-old woman complained of bilateral blurred vision for 2 months. She also reported occasional transient visual obscurations while changing positions and frequent pulsatile tinnitus at night. She denied headache, eye pain, fever, skin rash, and joint pain. She was a healthy, slim young woman and had given birth to a boy 3 months previously. She had not been taking oral contraceptives, systemic corticosteroids, or vitamin A derivatives. She reported a recent unintentional weight loss of 5 kg. Neuro-ophthalmological examination revealed the patient to be alert and oriented. Visual acuity was 20/60, right eye, and 20/20, left eye. Pupils were equal in size with a right relative afferent pupillary defect. Eye movements were full and visual fields showed generalized contraction, more so in the right eye. Ophthalmoscopy revealed diffuse edema of both optic discs with peripapillary hemorrhages, and macular exudes (Fig. 1). Brain magnetic resonance imaging (MRI) demonstrated an empty sella and dilation of the optic nerve sheaths without enhancement of the optic nerves (Fig. 2). Magnetic reso-nance venography was normal. The opening pressure on lumbar puncture was 450 mmH2O. The cerebrospinal fluid (CSF) was acellular with normal glucose (2.79 mmol/L, nor-mal: 2.5-4.4 mmol/L), chloride (126.6 mmol/L, normal: 120-130 mmol/L), and elevated protein (71 mg/dL, normal: 15-56 mg/dL). Other laboratory tests showed: white blood cell (WBC) 5.4 · 109/L, red blood cell 3.26 · 1012/L, hemoglobin 108 g/L, erythrocyte sedimentation rate (ESR) 35 mm/h, C-reactive protein (CRP) 8.6 mg/L (normal: ,5 mg/L), serum free T3 1.71 pmo1/L (normal: 2.0- 6.5 pmo1/L), free T4 6.12 pmo1/L (normal: 7.5-15), and thyroid-stimulating hormone 7.5 pmol/L (normal: 0.4-6.5 pmol/L). Serum protein electrophoresis revealed elevated IgG 2,600 mg/dL (normal: 751-1,560 mg/dL), IgA 341 mg/dL (normal: 82-453 mg/dL), and IgM 203 mg/dL (normal: 46- 304 mg/dL). IgG monoclonal spike: Kappa 2,520 mg/dL (normal: 629-1,350 mg/dL) and Lamda 150 mg/dL (nor-mal: 313-723 mg/dL). Bone marrow aspirate showed a slight increase in plasma cells, and biopsy of bone mar-row was otherwise normal. Department of Ophthalmology (GT), Eye and ENT Hospital, Fudan University, Shanghai, China; and Departments of Neurology (YJ, HJ, XZ) and Hematology (JW), Beijing Tongren Hospital, Capital Medical University, Beijing, China. The authors report no conflicts of interest. Address Correspondence to Xiaojun Zhang, MD, PhD, Department of Neurology, Beijing Tongren Hospital, Capital Medical University, No.1 Dong Jiao Min Xiang Street, Dongcheng District, Beijing 100730, China; E-mail: zxjune@gmail.com Tian et al: J Neuro-Ophthalmol 2014; 34: 169-172 169 Clinical Observation Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. Computed tomography (CT) of the chest showed multiple enlarged lymph nodes in the mediastinum and hilum and bilateral hydrothorax (Fig. 3). In addition, the liver and spleen were enlarged on abdominal CT. Lymph node biopsy revealed marked follicular hyperplasia with plasma cell infiltrates consistent with Castleman disease (Fig. 4). The patient was treated with CHOP (cyclophosphamide, doxorubicin, vincristine, and prednisolone) chemotherapy for 4 months without improvement in vision. Repeat lumbar puncture showed an opening pressure of 340 mmH2O. She started complaining of weakness of her legs, and neurological examination showed sensory deficits in stocking glove distri-bution and reduced deep tendon reflexes. Electromyography confirmed the diagnosis of motor and sensory peripheral neuropathy. The patient was referred for a clinical trial of rituximab. FIG. 1. Bilateral papilledema is present with macular exudates. FIG. 2. Brain magnetic resonance images. Noncontrasted axial T1 (A) and T2 (B) scans show normal brain structures, dilated optic nerve sheathes, and elevated optic discs. Coronal short-tau inversion recovery image (C) shows prominent cerebrospinal fluid signal surrounding the optic nerves while contrast-enhanced axial T1 image (D) reveals no enhancement of the optic nerves. 170 Tian et al: J Neuro-Ophthalmol 2014; 34: 169-172 Clinical Observation Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. One year later, visual acuity and fields were stable and optic discs showed pallor and gliosis with blurred margins. The patient became wheelchair bound due to progression of peripheral neuropathy and is being treated with rituximab, acupuncture, and physical therapy. DISCUSSION In 1956, Castleman et al (1) reported 13 cases of unicentric hyaline vascular disease of the chest with pathologic features of hypervascular lymph nodes containing hyalinized blood vessels. The disease may be unicentric or multicentric depending on the extent of lymph node involvement. Histopathogenetic classifi-cation includes hyaline vascular Castleman disease, plasma cell Castleman disease, human herpes virus 8 (HHV-8)-associated Castleman disease, and multicentric Castleman disease, as not otherwise specified (2). Approximately 70% of cases occur in the chest, 15% in the neck, and 15% in the abdomen and pelvis, involving primarily lymphatic tissues. Our patient's presenting symptom was blurred vision, associated with transient visual obscurations and pulsatile tinnitus. Her examination was remarkable for bilateral pap-illedema. The results of her brain MRI and elevated opening pressure on lumbar puncture were consistent with the diag-nosis of pseudotumor cerebri. However, the elevated CSF protein and abnormal ESR and CRP led to the diagnosis of papilledema secondary to an underlining systemic disease. The diagnosis of Castleman disease was established from the pathologic features of enlarged mediastinal lymph nodes. Central nervous system involvement in Castleman disease is uncommon. Since Black et al (3) reported a case of Castleman disease with pseudotumor cerebri in 1988, this association is rare although papilledema and increased intracranial pressure are noticed in many cases of the POEMS syndrome, which FIG. 3. Contrast-enhanced axial chest computed tomography. A. There is mediastinal and paratracheal adenopathy (arrow). B. A pericardial effusion (arrowheads) and a left-sided pleural effusion (arrow) are present. FIG. 4. Lymph node biopsy. A. Lymph node follicle contains penetrating, longitudinal vessels (arrow) and interfollicular re-gions with plasma cell infiltration (asterisks) (hematoxylin and eosin, ·100). B. Germinal center shows "onion skin" appearance (hematoxylin and eosin, ·400). Immunostaining is negative for CD34 (C) and positive for CD20 (D) (·100). Tian et al: J Neuro-Ophthalmol 2014; 34: 169-172 171 Clinical Observation Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. may be associated with plasma cell-type Castleman disease (4-8). The pathophysiology of papilledema in Castleman disease is unclear, although there are several potential mechanisms. In our case, optic disc swelling was likely due to increased CSF pressure rather than direct cellular infiltration, since the optic nerves did not enhance on MRI. We postulate that increased vascular permeability in our patient led to bilateral hydrothorax, pericardial effusion, and increased CSF volume resulting in intracranial hypertension and papilledema. Vascular endothelial growth factor (VEGF), which is expressed by osteoblasts, macrophages, and tumor cells (including plasma cells), is known to target endothelial cells, increasing vascular permeability, and stimulating angiogenesis (9,10). It is well known that elevation of the VEGF level in POEMS syndrome is associated with severe symptoms and can be used to monitor disease activity (11-13). In animal models of POEMS, mice that are transplanted with human glioblastoma exhibit high serum levels of VEGF, prominent edema with increased tissue volume, and pathologic findings in the liver, spleen, and kidney (13). Nishi et al (14) showed that the VEGF levels of the serum and supernatant fluid of cultured lymph nodes of 2 Castleman disease patients were higher than those in normal controls. VEGF was strongly expressed in plasma cells in the interfollicular region of the lymph nodes of their patients. These results suggest that this cytokine may be involved in vascular proliferation in the interfollicular region of the lymph nodes of the plasma cell- type Castleman disease. Increased VEGF may affect the blood-brain barrier by increasing permeability. Other upre-gulated cytokines, such as matrix metalloproteases, may cause additional exudation of fluid and intracranial hypertension. Our patient's initial clinical findings extended beyond multicentric lymph node involvement and included organo-megaly, endocrinopathy, and monoclonal gammopathy. She eventually developed motor and sensory polyneurop-athy. While not satisfying the diagnostic criteria for PO-EMS syndrome (15), our case illustrates a wide spectrum of pathologic and clinical manifestation, which might be con-sidered an overlap syndrome (16). We have no experience with the use of carbonic anhydrase inhibitors as an add-on therapy to reduce the intracranial pressure in Castleman disease. Our patient's blood while cell count dropped dramatically after a single dose of methazola-mide (100 mg) and, therefore, was discontinued. Long-term studies are needed in patients with Castleman disease to evaluate the efficacy of systemic chemotherapy, as well as targeted anti-monoclonal CD20 antibody and anti- VEGF therapy (17,18). REFERENCES 1. Castleman B, Iverson L, Menendez VP. Localized mediastinal lymph node hyperplasia resembling thymoma. Cancer. 1956;9:822-830. 2. Cronin DM, Warnke RA. Castleman disease: an update on classification and the spectrum of associated lesions. Adv Anat Pathol. 2009;16:236-246. 3. Black DA, Forgacs I, Davies DR, Thompson RP. Pseudotumour cerebri in a patient with Castleman's disease. Postgrad Med J. 1988;64:217-219. 4. Bolling JP, Brazis PW. Optic disk swelling with peripheral neuropathy, organomegaly, endocrinopathy, monoclonal gammopathy, and skin changes (POEMS syndrome). Am J Ophthalmol. 1990;109:503-510. 5. Kaushik M, Pulido JS, Abreu R, Amselem L, Dispenzieri A. Ocular findings in patients with polyneuropathy, organomegaly, endocrinopathy, monoclonal gammopathy, and skin changes syndrome. Ophthalmology. 2011;118:778-782. 6. Rison RA. Papilloedema and hypertrichosis: the varied and harried manifestations of POEMS syndrome. BMJ Case Rep. 2009;2009. pii: bcr09.2008.1000. 7. Barnés C, Sánchez-Dalmau BF, Vela D, Alarcón S. Papilledema as an indicator of POEMS syndrome. Arch Soc Esp Oftalmol. 2008;83:709-711. 8. Chong DY, Comer GM, Trobe JD. Optic disc edema, cystoid macular edema, and elevated vascular endothelial growth factor in a patient with POEMS syndrome. J Neuroophthalmol. 2007;27:180-183. 9. Soubrier M, Dubost JJ, Serre AF, Ristori JM, Sauvezie B, Cathebras P, Piette JC, Chapman A, Authier PJ, Gherardi RK. Growth factors in POEMS syndrome: evidence for a marked increase in circulating vascular endothelial growth factor. Arthritis Rheum. 1997;40:786-787. 10. Endo I, Mitsui T, Nishino M, Oshima Y, Matsumoto T. Diurnal fluctuation of edema synchronized with plasma VEGF concentration in a patient with POEMS syndrome. Intern Med. 2002;41:1196-1198. 11. Watanabe O, Arimura K, Kitajima I, Osame M, Maruyama I. Greatly raised vascular endothelial growth factor (VEGF) in POEMS syndrome. Lancet. 1996;347:702. 12. Arimura K, Hashiguchi T, Watanabe O. Crow-Fukase syndrome and VEGF. Brain Nerve. 2008;60:611-619. 13. D'Souza A, Hayman SR, Buadi F, Mauermann M, Lacy MQ, Gertz MA, Kyle RA, Kumar S, Greipp PR, Lust JA, Russell SJ, Zeldenrust S, Dingli D, Witzig TE, Rajkumar SV, Dispenzieri A. The utility of plasma vascular endothelial growth factor levels in the diagnosis and follow-up of patients with POEMS syndrome. Blood. 2011;118:4663-4665. 14. Nishi J, Arimura K, Utsunomiya A, Yonezawa S, Kawakami K, Maeno N, Ijichi O, Ikarimoto N, Nakata M, Kitajima I, Fukushige T, Takamatsu H, Miyata K, Maruyama I. Expression of vascular endothelial growth factor in sera and lymph nodes of the plasma cell type of Castleman's disease. Br J Haematol. 1999;104:482-485. 15. Dispenzieri A. POEMS syndrome: update on diagnosis, risk-stratification, and management. Am J Hematol. 2012;87: 804-814. 16. Gherardi RK, Malapest D, Degos JD. Castleman disease- POEMS syndrome overlap. Ann Int Med. 1991;114:520-521. 17. Ramchandren S, Lewis RA. An update on monoclonal gammopathy and neuropathy. Curr Neurol Neurosci Rep. 2012;12:102-110. 18. Saeed-Abdul-Rahman I, Al-Amri AM. Castleman disease. Korean J Hematol. 2012;47:163-177. 172 Tian et al: J Neuro-Ophthalmol 2014; 34: 169-172 Clinical Observation Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. |