| OCR Text |
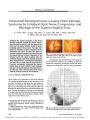
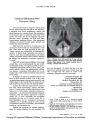
Show PHOTO ESSAY Positron Emission Tomography in Diagnosis of Visual Variant Alzheimer Disease Pasquale F. Finelli, MD FIG. 1. A. Axial FLAIR MRI (in ascending sections from left to right) in our patient shows no obvious atrophy. B. Positron emission tomography (PET) using 2-[18F]fluorodeoxyglucose, performed 2 weeks later, shows hypometabolism in the parieto-occipital regions bilaterally (arrowheads). C. PET of age-matched and sex-matched control subject shows normal metabolism in those regions. (Red, yellow, green, and blue represent a decreasing scale of glucose metabolism.) Abstract: A 65-year-old man with a 3-year history of difficulty seeing had normal ophthalmologic and neurologic examinations except for impaired visual spatial and perceptual function. Brain MRI failed to disclose any structural abnormalities, but positron emission tomography (PET) performed 2 weeks later Department of Neurology, Hartford Hospital, and University of Connecticut School of Medicine, Hartford, Connecticut. Address correspondence to P. Finelli, MD, Hartford Hospital, 80 Seymour Street, Hartford, CT 06102-5037; E-mail: pfinell@harthosp.org showed prominent hypometabolism in the parieto-occipital regions bilaterally. These findings were considered consistent with the visual variant of Alzheimer disease (VVAD). Although the dissocia-tion between normal structural and abnormal functional imaging has been reported before in VVAD, this patient is a reminder that PET may be useful to confirm the diagnosis before the disease becomes advanced. (J Neuro-Ophthalmol 2009;29:149-150) J Neuro-Ophthalmol, Vol. 29, No. 2, 2009 149 Copyright © Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. J Neuro-Ophthalmol, Vol. 29, No. 2, 2009 Finelli A65-year-old man with a master's degree reported difficulty seeing and reading that had begun 3 years earlier. Ophthalmologic examination was normal. Neuro-logic examination was remarkable only for a score of 26 of 30 points on the Mini-Mental Status Examination and slow reading with poor comprehension. Formal neuro-psychometric testing confirmed borderline impaired cog-nitive function with a predominant deficit in visual perceptual and visual spatial processing. Brain MRI (Fig. 1A) was normal. Results of other ancillary studies, including carotid Doppler ultrasonogra-phy, complete blood count, routine blood chemistry analyses, rapid plasma reagin (RPR) serology, thyroid function tests, and vitamin B12, were also normal. PET performed 2 weeks after the brain MRI study showed prominent hypometabolism in the parieto-occipital region bilaterally (Fig. 1B), moderate hypometabolism in temporoparietal regions, and normal metabolism in the posterior cingulate region, as compared to a normal control study (Fig. 1C). These findings were considered charac-teristic of the visual variant of Alzheimer disease (VVAD). Our patient with VVAD is noteworthy because brain MRI failed to disclose brain atrophy. Correlation with the visual perceptual and spatial dysfunction found on clinical testing was found only with posterior hemispheric hypo-metabolism on PET. One study of patients with other variants of demen-tia showed an 83% sensitivity and 85% specificity for Alzheimer disease using a visual rating scale for temporal lobe atrophy (1). Quantitative MRI studies with serial volume measurement might be more sensitive, but because of lack of automation and their labor-intensive nature, they have limited usefulness in clinical practice (2). PET using 2-[18F]fluorodeoxyglucose has proven diagnostic value in VVAD with hypometabolism seen before structural imaging discloses atrophy (3). In VVAD, visual manifestations may precede memory and cognitive impairment by years, leading sometimes to a misdiagnosis of psychogenic visual loss (4,5). Alexia, visual spatial dysfunction, the inability to interpret complex scene (simultanagnosia), difficulty recognizing familiar objects (visual agnosia), and sometimes visual field defects are features of VVAD (4,6) Visual spatial tests, such as draw-ing a clockface, copying the Rey diagram, and interpreting pictures, can bring out deficits not readily recognized in the standard ophthalmic or neurologic examinations. Interestingly, our patient became claustrophobic in the magnetic resonance scanner, and three attempts to perform MRI failed despite increasing oral sedation before successful completion with general anesthesia. Others (6) have noted a higher dropout rate among VVAD study patients than among those with other variants of dementia because of failure to complete the imaging portion of the protocol (6). This excessive claustrophobia may be due to disintegration of a coherent representation of visual space. REFERENCES 1. O'Brien JT, Desmond P, Ames D, et al. Temporal lobe magnetic resonance imaging can differentiate Alzheimer's disease from normal ageing, depression, vascular dementia and other causes of cognitive impairment. Psychol Med 1997;27: 1267-75. 2. Petrella JR, Coleman RE, Doraiswamy PM. Neuroimaging and early diagnosis of Alzheimer disease: a look to the future. Radiology 2003; 226:315-36. 3. Bokde AL, Pietrini P, Ibenez V, et al. The effect of brain atrophy on cerebral hypometabolism in the visual variant of Alzheimer disease. Arch Neurol 2001;58:480-6. 4. Lee AG, Martin CO. Neuro-ophthalmic findings in the visual variant of Alzheimer's disease. Ophthalmology 2004;111:376-81. 5. Atchison M, Harrison AR, Lee MS. The women who needed a PET. Surv Ophthalmol 2006;51:592-5. 6. Nestor PJ, Caine D, Fryer TD, et al. The topography of metabolic deficits in posterior cortical atrophy (the visual variant of Alzheimer's disease) with FDG-PET. J Neurol Neurosurg Psychiatry 2003;74:1521-9. 150 © 2009 Lippincott Williams & Wilkins Copyright © Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. |