Collection of materials relating to neuro-ophthalmology as part of the Neuro-Ophthalmology Virtual Education Library.
NOVEL: https://novel.utah.edu/
TO
- NOVEL966
Filters: Collection: "ehsl_novel_novel"
| Title | Creator | Description | Subject | ||
|---|---|---|---|---|---|
| 251 |
 |
Idiopathic Intracranial Hypertension | NANOS | Idiopathic intracranial hypertension (IIH), also called pseudotumor cerebri, is a condition in which there is high pressure in the fluid surrounding your brain, spinal cord, and optic nerves. This can cause headaches and problems with vision. | Idiopathic Intracranial Hypertension; Patient Brochure |
| 252 |
 |
Giant Cell Arteritis | NANOS | Giant cell arteritis is a condition that can cause vision loss, new persistent headaches, scalp tenderness, and jaw pain with chewing. It is due to inflammation of blood vessels primarily of the head and neck. | Giant Cell Arteritis; Patient Brochure |
| 253 |
 |
Thyroid Eye Disease | NANOS | Thyroid eye disease, also called dysthyroid orbitopathy, is an autoimmune condition in whichyour body's immune system triggers inflammation in the eye socket (also called the orbit),affecting the muscles that move the eye and the fatty tissue behind the eye. | Thyroid Eye Disease; Thyroid Orbitopathy; Patient Brochure |
| 254 |
 |
Neuro-ophthalmic Disorders in Pregnancy: With an Eye to Future Eye Health | Kathleen B. Digre, MD | Presentation covering conditions relevant to neuro-ophthalmology, including vascular disorders that affect vision, Pseudotumor Cerebri Syndrome, venous sinus thrombosis, idiopathic intracranial hypertension, and severe pre-eclampsia and eclampsia. | Pregnancy |
| 255 |
 |
Optic Nerve Sheath Meningioma | NANOS | Optic nerve sheath meningioma is a benign (not malignant) tumor which involves the covering of the optic nerve. Meningiomas (along with gliomas and pituitary tumor) are the most common tumors inside the skull. | Optic Nerve Sheath Meningioma; Patient Brochure |
| 256 |
 |
Menieres Disease | NANOS | Menière's Disease is named after Prosper Menière, a French physician who first described the condition in 1861. It is an inner ear disorder that can cause vertigo (false sensation of motion). | Menieres Disease; Patient Brochure |
| 257 |
 |
Eyelid Myokymia | NANOS | Eyelid myokymia is a very common condition that many people have experienced at least briefly at one time or another, though the exact prevalence is not known. Myokymia is characterized by involuntary fine contractions or "twitching" of the eyelids. | Eyelid Myokymia; Patient Brochure |
| 258 |
 |
Progressive Supranuclear Palsy | NANOS | Progressive Supranuclear Palsy (PSP) is a rare progressive neurodegenerative disorder that affects certain parts of the brain, resulting in difficulty with balance, walking, swallowing, and vision. | Progressive Supranuclear Palsy; Patient Brochure |
| 259 |
 |
Lateral Orbitotomy with Bone Window | Richard C. Allen, MD, PhD, FACS | Narrated video of lateral orbitotomy with bone removal for improved orbital decompression. | Orbitotomy; Orbital Decompression |
| 260 |
 |
Lateral Orbitotomy #3 | Richard C. Allen, MD, PhD, FACS | Narrated video of lateral orbitotomy and biopsy of presumed benign cavernous hemangioma. | Orbital Biopsy; Orbitotomy |
| 261 |
 |
Lateral Orbitotomy #2 | Richard C. Allen, MD, PhD, FACS | Narrated video of lateral orbitotomy and biopsy of presumed orbital inflammatory condition. | Orbital Biopsy; Orbitotomy |
| 262 |
 |
Lateral Canthotomy Incision | Richard C. Allen, MD, PhD, FACS | Narrated video of lateral canthotomy procedure. | Lateral Canthotomy |
| 263 |
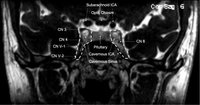 |
Cavernous Sinus | Andrew R. Carey, MD | Cavernous sinus imaging with labels. | Cavernous Sinus |
| 264 |
 |
The Mental Status Examination (MSE): The Basics | Victoria S. Pelak, MD | An overview of the Mental Status Examination. | Mental Status Examination; Examinations |
| 265 |
 |
Management of Non-Organic Vision Loss | Aumer Shughoury, BA; Devin D. Mackay, MD | A description of the management of non-organic visual loss. | Non-Organic Vision Loss; NOVL |
| 266 |
 |
Confrontation Visual Fields - A Concise Guide for Ophthalmology and Neurology Trainees | Stephen C. Pollock, MD | The guide describes the techniques required to competently perform confrontation visual fields. It outlines a basic screening protocol and discusses methods for further defining defects identified during the screening process. A mini-atlas of visual field defects is included as an appendix. | Confrontation Visual Fields; Visual Field Testing; Perimetry; Visual Field Loss; Visual Field Defect; Ocular Examination; Visual Sensory Evaluation; Neurologic Examination |
| 267 |
 |
Ocular Lateropulsion Left AICA Stroke | Jorge C Kattah, MD | 82 year-old patient with basilar artery stenosis, she developed an acute left AICA stroke. On examination within 24 hours from symptom onset, she had primary gaze, unidirectional, right beat nystagmus and a positive left head impulse test. Brief periods of eyelid closure were associated with a h-... | Ocular Lateropulsion; AICA Stroke |
| 268 |
 |
Right Lateral Medulla and Cerebellar Stroke | Jorge C Kattah, MD | This patient presented with an acute vestibular syndrome, he has a h-left beat nystagmus and a normal head impulse test . He had grade 3 truncal ataxia and severe ocular lateropulsion to the right (type 1 overt OL). Hypometric leftward, centripetal, slow saccades were video-recorded even six weeks... | Right Lateral Medulla; Cerebellar Stroke |
| 269 |
 |
Clinical Characteristics of Ocular Lateropulsion | Jorge C Kattah, MD | A discussion of the normal mechanism that maintain the eyes in normal horizontal position. | Ocular Lateropulsion; Unilateral Gaze Palsy; Radiographic h-CGD |
| 270 |
 |
Dual Visual Field Defect (Quadrantanopia and Central Scotoma) Unmasks the Hidden Brain Lesion in a Patient with Non-arteritic Ischemic Optic Neuropathy | A. Mohan Kannam; B. Rajat Kapoor; C. Ramesh Kekunnaya, FRCS; Virender Sachdeva, MS, DNB | This submission is an interesting case that highlights the co-existence of two different visual field defects in the same patient presenting to us with clinical picture of non arteritic ischemic optic neuropathy. The correct interpretation of the visual field defects led to the appropriate localizat... | Hemianopia; Central Field Defect; Non-Arteritic Ischemic Optic Neuropathy; Ischemic Infarct |
| 271 |
 |
Convergence-Retraction Nystagmus in Dorsal-Midbrain Syndrome | Paul Freund, MD, FRCSC; Edward Margolin, MD, FRCSC | A man in his early twenties was referred by optometrist for abnormal eye motility findings. He had a remote history of an excised pinealoma. On exam he had almost complete upgaze palsy, convergence-retraction nystagmus on attempted upgaze, and light-near dissociation of pupillary reaction, the class... | Dorsal Midbrain Syndrome; Parinaud Syndrome; Convergence-Retraction Nystagmus; Light-Near Dissociation |
| 272 |
 |
Clinical Visual Electrophysiology | Gregory P. Van Stavern, MD; Byron Lam, MD | A description of the use of electrophysiology to examine the visual system. | Electrophysiology; Visual Exam |
| 273 |
 |
Fundus Fluorescein Angiography: What Is It and When Is It Useful for Neuro-Ophthalmology? | Clare L. Fraser, MBBS; Elisa E. Cornish, PhD | An introduction to the use of fluorescein angiography. | Fluorescein Angiography; Visual Exam |
| 274 |
 |
Examination of the Orbit and Extraocular Structures | Julie Falardeau, MD | Introduction to the Examination of Orbit and Extraocular Structures in the NExT curriculum. | Exams; Orbit; Extraocular |
| 275 |
 |
Hirschberg Test Corneal Reflex Test | Nagham Al-Zubidi, MD | Description of the Hirschberg test a the corneal reflex test. | Hirschberg Test; Corneal Reflex |
