| OCR Text |
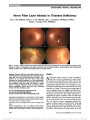
Show Positive Apraclonidine Test in Horner Syndrome Caused by Thalamic Hemorrhage Courtney Y. Kauh, MD, Lulu L. C. D. Bursztyn, MSc, MD Abstract: Reversal of anisocoria following instillation of apraclonidine 0.5% has been reported in Horner syndrome caused by lesions of the central and peripheral nervous system. The shortest documented latency between symp-tom onset and a positive apraclonidine test is 36 hours, occurring in a patient with a pontomedullary infarct. We present the case of a 69-year-old man with Horner syndrome due to thalamic hemorrhage in whom apraclonidine testing demonstrated reversal of anisocoria 4 days after symptom onset. This is the first reported case of a positive apraclo-nidine test in a Horner syndrome caused by a lesion at this site. It suggests that apraclonidine testing is useful in confirming the diagnosis within days of onset even in a lesion located at the most proximal portion of the oculosympathetic pathway. Journal of Neuro-Ophthalmology 2015;35:287-288 doi: 10.1097/WNO.0000000000000222 © 2015 by North American Neuro-Ophthalmology Society Horner syndrome occurs when there is a disruption of the oculosympathetic pathway, leading to ipsilateral miosis, lid ptosis, and facial anhidrosis. Topical cocaine eye drops, which blocks reuptake of norepinephrine, has traditionally been used to diagnose Horner syndrome (1). Topical apraclonidine is gaining acceptance for pharmacologic testing due to lower cost, increased avail-ability and a more easily visible endpoint (2). However, sympathetic denervation must occur before the weak alpha-1 activity of apraclonidine causes pupillary dilation and reversal of anisocoria (3,4). The length of time required for sympathetic denervation has not been established. CASE REPORT A 69-year-old man developed sudden profound lethargy, as well as numbness and weakness of the right arm. He was taking no medications and had no known medical history. On arrival at our hospital 2 days after symptom onset, he was alert with normal vital signs. Neurologic examination disclosed right hemibody hypoesthesia and reduced strength in the right arm. Muscle stretch reflexes were normal. Brain magnetic resonance imaging demonstrated acute hemor-rhage in the left thalamus (Fig 1). Ophthalmologic examination was normal apart from the findings of 2 mm of left upper lid ptosis, left lower lid (reverse) ptosis, and anisocoria. In dim illumination, pupils measured 5 mm in the right eye and 3.5 mm in the left eye (Fig. 2A) constricting to 3 and 2 mm, respectively. There was no relative afferent pupillary defect. Apraclonidine 0.5% drops were administered 4 days after the onset of symptoms. Thirty minutes after instillation, pupils mea-sured 3.5 mm in the right eye and 5 mm in the left eye, and there was slight reduction of the left upper and lower lid ptosis (Fig. 2B). DISCUSSION Apraclonidine is gaining acceptance as a pharmacologic diagnostic tool to confirm Horner syndrome, particularly in patients presenting with anisocoria without other localizing signs or symptoms. It is primarily an alpha-2 agonist with weak affinity for alpha-1 receptors, which are the pre-dominant receptors in the iris dilator muscle (5). Apraclo-nidine has little effect on pupils in normal eyes. However, it exerts a mydriatic effect in Horner syndrome where sympa-thetic denervation leads to upregulation of the alpha-1 re-ceptors (3,4). Instillation of apraclonidine causes a reversal of anisocoria, with dilation of the sympathetically dener-vated pupil. The overall sensitivity and specificity of 0.5% apraclo-nidine in the diagnosis of Horner syndrome seems to be comparable with that of topical cocaine, the traditional Department of Ophthalmology and Visual Sciences, Kellogg Eye Center, University of Michigan, Ann Arbor, Michigan. The authors report no conflicts of interest. Address correspondence to Lulu L. C. D. Bursztyn, MSc, MD, Department of Ophthalmology and Visual Sciences, Kellogg Eye Center, University of Michigan, 1000 Wall Street, Ann Arbor, MI 48105; E-mail: lulu.bursztyn@gmail.com Kauh and Bursztyn: J Neuro-Ophthalmol 2015; 35: 287-288 287 Clinical Observation Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. agent used in pharmacologic testing for Horner syndrome (4,6-8). In the only series to report the effect of apracloni-dine on control eyes (6), mydriasis was noted in 19% and lid elevation in 45% of normal eyes, but no reversal of anisocoria was observed. In one series, cocaine administra-tion was shown to produce anisocoria .0.5 mm in 9 of 50 normal patients as compared with 118 of 119 patients with Horner syndrome (1). There have been no reports of false positive tests with apraclonidine. The principal reservation about the value of apracloni-dine in diagnosis of Horner syndrome has been the question of whether it will be positive early enough. The delay before sufficient alpha-1 upregulation occurs to produce a positive apraclonidine test is unknown. Apraclonidine testing has been positive within 1 week of carotid artery dissection (9) and cluster headache with sinusitis (10), both due to lesions of the third-order neuron of the oculosympathetic pathway. However, in a patient with a first-order Horner syndrome due to a pontomedullary infarct, the reported interval between onset of symptoms and a positive apraclonidine test was 1.5 days (11). In our patient, apraclonidine testing was positive within 4 days of symptom onset, again suggesting that upregulation of alpha-1 receptors after denervation oc-curs very quickly and that apraclonidine testing is likely to be valuable even in Horner syndrome caused by a lesion in the most proximal portion of the oculosympathetic pathway. Although Horner syndrome caused by a thalamic lesion has been confirmed with cocaine testing (12), our case is the first to report a positive apraclonidine test in this set-ting. The 2 cases of Horner syndrome with reversal of anisocoria after less than a week of symptom onset [this case and that of a pontomedullary infarct (11)] both had central causes. A Horner syndrome due to carotid dissec-tion (9) tested at 4 days caused partial dilation of the affected pupil but not reversal of anisocoria. It is possible that a central lesion causes complete loss of sympathetic input and may lead to more rapid sympathetic denervation than a lesion of the second- or third-order neurons. It remains to be demonstrated how early apraclonidine will be positive in the setting of more peripheral lesions causing Horner syndrome. REFERENCES 1. Kardon RH, Denison CE, Brown CK, Thompson HS. Critical evaluation of the cocaine test in the diagnosis of Horner's syndrome. Arch Ophthalmol. 1990;108:384-387. 2. Kardon R. Are we ready to replace cocaine with apraclonidine in the pharmacologic diagnosis of Horner syndrome. J Neuroophthalmol. 2005;25:69-70. 3. Ramsay DA. Dilute solutions of phenylephrine and pilocarpine in the diagnosis of disordered autonomic innervation of the iris. Observations in normal subjects, and in the syndromes of Horner and Holmes-Adie. J Neurol Sci. 1986;73:125-134. 4. Morales J, Brown SM, Abdul-Rahim AS, Crosson CE. Ocular effects of apraclonidine in Horner syndrome. Arch Ophthalmol. 2000;118:951-954. 5. Abrams DA, Robin AL, Pollack IP, deFaller JM, DeSantis L. The safety and efficacy of topical 1% ALO 2145 (p-aminoclonidine hydrochloride) in normal volunteers. Arch Ophthalmol. 1987;105:1205-1207. 6. Koc F. The sensitivity and specificity of 0.5% apraclonidine in the diagnosis of oculosympathetic paresis. Br J Ophthalmol. 2005;89:1442-1444. 7. Davagnanam I, Fraser CL, Miszkiel K, Daniel CS, Plant GT. Adult Horner's syndrome: a combined clinical, pharmacological, and imaging algorithm. Eye. 2013;27:291-298. 8. Brown SM, Aouchiche R, Freedman KA. The utility of 0.5% apraclonidine in the diagnosis of Horner syndrome. Arch Ophthalmol. 2003;121:1201-1203. 9. Cooper-Knock J, Pepper I, Hodgson T, Sharrack B. Early diagnosis of Horner syndrome using topical apraclonidine. J Neuroophthalmol. 2011;31:214-216. 10. Garibaldi DC, Hindman HB, Grant MP, Iliff NT, Merbs SL. Effect of 0.5% apraclonidine on ptosis in Horner syndrome. Ophthal Plast Reconstr Surg. 2006;22:53-55. 11. Lebas M, Seror J, Debroucker T. Positive apraclonidine test 36 hours after acute onset of Horner syndrome in dorsolateral pontomedullary stroke. J Neuroophthalmol. 2010;30:12-17. 12. Faust-Socher A, Greenberg G, Inzelberg R. Thalamic-hypothalamic infarction presenting as first-order Horner syndrome. J Neurol. 2013;260:1673-1674. FIG. 2. Left Horner syndrome. A. Red-free photo reveals left upper and lower eyelid ptosis and pupillary miosis. B. Thirty minutes after instillation of 0.5 apraclonidine drops, the left pupil is now larger than the right with slight reduction in the left upper and lower lid ptosis. FIG. 1. T2 axial (A) and coronal (B) magnetic resonance imaging shows a left thalamic hemorrhage with vasogenic edema. 288 Kauh and Bursztyn: J Neuro-Ophthalmol 2015; 35: 287-288 Clinical Observation Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. |