| OCR Text |
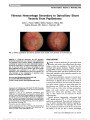
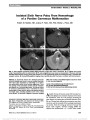
Show Recurrent Third Nerve Palsy as the Presenting Feature of Neurofibromatosis 2 Victoria J. M. Barrett, MB ChB, FRCOphth, Mei H. Tan, MB BCh BAO, PhD, FRCOphth, John S. Elston, MD, FRCOphth Abstract: Neurofibromatosis 2 (NF2) is a rare autosomal dominant disorder associated with the development of multiple central and peripheral nervous system tumors. Patients with NF2 are often diagnosed in adulthood, with symptoms of an isolated tumor or hearing loss associated with vestibular schwannomas. Diagnosing NF2 in children is complicated by the fact that the diagnostic criteria often are not met at presentation and there is usually no family history of the disease. The authors describe the diagnostic challenge posed by a pediatric patient who developed a relapsing and remitting third nerve paresis and was later diagnosed with NF2. A mechanism for the recurrent cranial mononeuropathy is proposed. Journal of Neuro-Ophthalmology 2012;32:329-331 doi: 10.1097/WNO.0b013e3182726b49 © 2012 by North American Neuro-Ophthalmology Society Recurrent third nerve palsy in any age group is rare; in childhood, most cases are attributed to ophthalmople-gic migraine (OM). This entity is characterized by onset in the first decade of life with headache or periorbital pain, nausea, and the simultaneous or subsequent development of a unilateral third nerve palsy followed by recovery over several weeks. During the acute phase, thickening and enhancement of the cisternal segment of the involved third nerve may be seen on brain magnetic resonance imaging (MRI), which resolves with recovery of third nerve function. Ipsilateral recurrences are common. OM is no longer clas-sified as a migraine variant but as an inflammatory neuralgia; resolution of the palsy is accelerated by systemic steroid treatment (1). We present a case in which an ipsilateral isolated third nerve palsy occurred twice in the first 6 years of life of a healthy girl with complete spontaneous recovery. On both occasions, patient evaluation was unremarkable. Recurrence at the age of 9 years led to discovery of a schwannoma of the affected third nerve and bilateral vestibular schwannomas. CASE REPORT A healthy 2-year-old girl presented with complete right third nerve palsy with pupillary involvement that evolved over 1 week. There was no history of preceding illness or trauma. General physical and neurologic examinations were otherwise normal. The patient was born at term by Cesarean section and her medical history was unremarkable. Her visual development was normal. Her parents were both in good health, and there was no relevant family history. Computed tomography (CT) and contrast-enhanced MRI of the brain were normal. Hematological and bio-chemical screening was negative for inflammatory markers and autoantibodies, including antiacetylcholine receptor and anti-GQ1b. Lumbar puncture showed normal opening pressure and cerebrospinal fluid. The patient remained well, and her ptosis resolved within 3 weeks and pupillary and eye movement function were normal within 6 weeks. Because the right eye became amblyopic, a patching regimen was begun, and the patient regained visual acuity of 20/30. At the age of 5 years, she again developed a painless isolated pupil involving right third nerve palsy over the course of a week. An unenhanced MRI of the brain was normal. Again, there was complete recovery of right third nerve function over a 6-week period. At the age of 9 years, a partial right third nerve palsy with partial pupillary dilation developed slowly over 6 months. There was no sensory disturbance, and other cranial nerve function was normal. A focal posterior lens opacity in the right eye was noted for the first time. Contrasted MRI Department of Ophthalmology, Oxford Eye Hospital, Oxford, United Kingdom. The authors report no conflicts of interest. Address correspondence to John S. Elston, MD, FRCOphth, Oxford Eye Hospital, John Radcliffe Hospital, Headley Way, Oxford OX3 9DU, United Kingdom; E-mail: john.elston@orh.nhs.uk Barrett et al: J Neuro-Ophthalmol 2012; 32: 329-331 329 Original Contribution Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. of the brain showed enhancement of the subarachnoid portion of the right third nerve consistent with a schwannoma (Fig. 1) and small bilateral vestibular schwannomas (Fig. 2). The patient was thought to have NF2, and this was confirmed by genetic testing. A lymphocyte DNA sample revealed a single nucleotide substitution c.169C.T in exon 2 of the NF2 gene. This mutation results in a premature trun-cation of the polypeptide chain and, therefore, was a pathogenic mutation. Because there was no family history of neurofibro-matosis and screening of other family members was unremark-able, this was presumed to be a de novo mutation. Audiology testing showed no hearing loss. Spinal MRI revealed a small meningioma at the T3 level 3 that was asymptomatic. The diagnosis and implications of NF2 were explained to the patient's parents, and she was referred to the medical service dealing with NF2 patients. Her right third nerve paresis gradually worsened over the ensuing 2 years. DISCUSSION Isolated palsies of the third, fourth, and sixth nerves have been reported infrequently in NF2 patients (2). We are unaware of any other published cases of NF2 presenting with a relapsing-remitting third nerve palsy. There are 2 previous reports describing recurrent third nerve palsy beginning in childhood in individuals who were subsequently shown to have the magnetic resonance changes compatible with ipsilateral oculomotor nerve schwannoma (3,4). There were no other stigmata of NF2. In both cases, the ophthalmoplegic attacks were associated with focal headache and systemic symptoms, including nau-sea, supporting the diagnosis of OM. Thickening and enhancement of the third nerve may persist after an attack of OM, and it may be that repeated episodes of inflamma-tory demyelination followed by remyelination led to focal schwann cell proliferation giving the appearance of schwan-noma on MRI. In contrast, in our patient, there were no clinical features to suggest an inflammatory etiology for the initial 2 episodes of third nerve palsy, and neuroimaging was normal on both occasions. We propose a different mechanism in our case. Schwan-nomas develop in NF2 as a result of a mutation, which inactivates the tumor suppressor gene located on chromo-some 22q12 whose 17 exons encode a 69-kDa protein product called merlin found in schwann cells (5,6). Merlin is important in the control of schwann cell metabolism, including cell-to-cell interactions and both intracellular and intercellular signaling pathways. Schwannomas, consist-ing of abnormal mutated schwann cells in a collagen matrix, develop when the function of the normal NF2 allele is inactivated. The mechanism of inactivation is uncertain. FIG. 1. Contrasted T1 coronal magnetic resonance imaging of the brain shows an area of abnormal enhancement in the subarachnoid portion of the right third nerve (arrow), con-sistent with a schwannoma. FIG. 2. Contiguous contrast-enhanced T1 axial magnetic resonance images demonstrate bilateral vestibular schwannomas (arrows). 330 Barrett et al: J Neuro-Ophthalmol 2012; 32: 329-331 Original Contribution Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. And in tumorigenesis, merlin dysfunction causes defects in the stability of the cell plasma membrane as it connects to the cytoskeleton, leading to cell deformation and instability (7). We speculate that merlin dysfunction in our patient compromised one or more schwann cells integral to right third nerve function before the development of a tumor detectable on MRI. This resulted in 2 episodes of acute conduction block causing a third nerve palsy, which spon-taneously recovered. When NF2 presents in childhood with a mononeuropathy (e.g., facial palsy), spontaneous improvement may occur, possibly by the same phenome-non (8), with eventual progression of the cranial nerve palsy. We recognize that there are other possible explana-tions, including the presence of a microscopic schwannoma not detectable by MRI at the time of the initial presentation or that the initial ophthalmoplegia was unrelated to the development of the schwannoma and the diagnosis of NF2. Our case highlights the difficulty in diagnosing NF2 in pediatric patients (9). NF2 has wide phenotypic variability, and only 18% of patients present in the first 15 years of life. Typically, adults initially develop hearing loss, tinnitus, and imbalance because of vestibular schwannomas; less than 30% of pediatric cases present this manner (9). Instead, children present with a mononeuropathy, most commonly affecting the seventh cranial nerve or rarely the peroneal nerve causing foot drop. The cranial nerve palsy may improve spontaneously and precede detection of a vestibular schwannoma by many years (8-10). Childhood NF2 is associated with more severe disease because of associated nonsense or frame-shift mutations that lead to truncation of a protein product. This was true in our patient, where the nucleotide substitution c.169C.T resulted in a nonsense mutation of the arginine residue at position 57 (p.Arg57X) and premature termination of the polypeptide chain. This also is true of mutations in exons 1 to 5 (9). In our patient, the mutation was detected on analysis of lymphocytes, eliminating mosaicism. Mosaicism occurs with high frequency in NF2, and patient with mosa-icism have tumors confined to a specific level of the neuraxis or milder of asymmetric involvement. Using the Manchester criteria (11), the presence of bilat-eral vestibular schwannomas coupled with the genetic find-ings enabled a diagnosis of NF2 to be made in our patient (Table 1). The characteristic focal lens opacity in the form of a posterior subcapsular cataract also was consistent with this diagnosis. REFERENCES 1. Headache Classification Subcommittee of the International Headache Society. The international classification of headache disorders. Cephalalgia. 2004;24(suppl 1):132. 2. Ragge NK, Baser ME, Riccardi VM, Falk RE. The ocular presentation of neurofibromatosis 2. Eye (Lond). 1997;11: 12-18. 3. Murakami T, Funatsuka M, Komine M, Hirayama Y, Suzuki H, Shishikura K, Aihara Y, Shibata K, Horf T, Kobayashi M, Osawa M. Oculomotor nerve schwannoma mimicking ophthalmoplegic migraine. Neuropediatrics. 2005;36:395-398. 4. Kawasaki A. Oculomotor nerve schwannoma associated with ophthalmoplegic migraine. Am J Ophthalmol. 1999;128: 658-660. 5. Evans DG, Huson SM, Donnai D, Neary W, Blair V, Newton V, Harris R. Clinical study of type 2 neurofibromatosis. Q J Med. 1992;84:603-618. 6. Bosch MM, Wichmann WW, Boltshauser E, Landau K. Optic nerve sheath meningiomas in patients with neurofibromatosis type 2. Arch Ophthalmol. 2006;124:379-385. 7. Viader A, Golden JP, Baloh RH, Schmidt RE, Hunter DA, Mibrandt J. Schwann cell mitochondrial metabolism supports long term axonal survival and peripheral nerve function. J Neurosci. 2011;31:10128-10140. 8. Evans DG, Birch JM, Ramsden RT. Pediatric presentation of type 2 neurofibromatosis. Arch Dis Child. 1999;81:496-499. 9. Asthagiri AR, Parry DM, Butman JA, Kim HJ, Tsilou ET, Zhuang Z, Lonser RR. Neurofibromatosis type 2. Lancet. 2009;373:1974-1986. 10. Evans DG. Neurofibromatosis type 2 (NF2): a clinical and molecular review. Orphanet J Rare Dis. 2009;4:16. 11. Evans DG, Raymond FL, Barwell JG, Halliday D. Genetic testing and screening of individuals at risk of NF2. Clin Genet. 2012;82:416-424. TABLE 1. Diagnostic criteria for neurofibromatosis type 2 Major Criteria Additional Criteria Bilateral VS or family history of NF2 plus Unilateral VS plus any 2 of: meningioma, glioma, neurofibroma, schwannoma, and posterior capsular lens opacity 1) Unilateral VS or or 2) Any 2 of: meningioma, glioma, neurofibroma, schwannoma, and posterior subcapsular cataract Multiple meningioma (2 or more) plus unilateral VS or any two of: glioma, neurofibroma, schwannoma, and posterior subcapsular lens opacity NF2, neurofibromatosis type 2; VS, vestibular schwannoma. Modified from the study by Evans et al. (11). Barrett et al: J Neuro-Ophthalmol 2012; 32: 329-331 331 Original Contribution Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. |