| OCR Text |
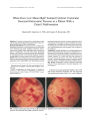
Show Journal ofNeuro- Ophthalmology 21( 2): 109- 111, 2001. © 2001 Lippincott Williams & Wilkins, Inc., Philadelphia Case Report Interferon- Alpha 2a Treatment of Neuro- Behcet Disease John C. Nichols, MD, Akgun Ince, MD, Levent Akduman, MD, and Eric S. Mann, MD, PhD Behcet disease is a multisystemic, chronic, recurrent inflammatory disorder characterized as a triad of hypopyon uveitis, oral aphthae, and genital ulcers. Neurologic involvement in Behcet disease ( neuro- Behcet) is common. Neuro- Behcet disease typically manifests late after disease onset, rarely coincides with ocular involvement, and often heralds a poor prognosis for final vision and survival. We present a case of neuro- Behcet disease with neurologic onset concomitant with systemic and ocular involvement that was responsive to treatment with interferon- alpha 2a. Key Words: Interferon- alpha 2a- Behcet disease- Neuro- Behcet disease. CASE REPORT A 25- year- old man was referred to us because of his 2- week history of painful oral and genital ulcers. The patient denied any similar episode in the past or travel outside the United States. Although the patient was born in the United States and does appear Semitic, he denies any Japanese, Asian, or Mediterranean ancestry. Before the onset of aphthous ulcers, he reported transient blurred vision, headache, and fever. Ocular examination revealed visual acuity 20/ 25 OU. Confrontation visual fields were full to finger counting. Pupils appeared normal with no relative afferent pupillary defect. There was bilateral iridocyclitis without hypopyon and trace vitreitis OU. Optic nerve examination revealed bilateral disc edema ( Fig. 1) without spontaneous venous pulsations. Indirect ophthalmoscopy revealed retinitis and retinal vasculitis in the midperiphery OU. Dermatologic evaluation upon hospital admission revealed papulopustule lesions and folliculitis on his back. The patient exhibited pathergy with pustule formation at the site of an intravenous catheter placement. Subsequent Manuscript received September 22, 2000; accepted February 6, 2001. From the Saint Louis University Eye Institute ( ICN, ESM) and the Department of Internal Medicine ( AI), Saint Louis University Health Sciences Center, and The Retina Center ( LA), Saint Louis, Missouri. Address correspondence and reprint requests to Eric S. Mann, MD, PhD, Saint Louis University Eye Institute, 1755 South Grand Boulevard, St. Louis, MO 63104; e- mail: manne4@ slu. edu. biopsy of this site demonstrated a leukocytoclastic vasculitis by histopathology. Although the results from a formal pathergy test were negative, skin manifestations were consistent with Behcet disease. The patient had a generalized tonic- clonic seizure upon hospitalization. A magnetic resonance imaging ( MRI) scan of the brain showed a right temporal lobe lesion ( Fig. 2). An electroencephalogram confirmed the focus of the seizure in the right temporal lobe. A lumbar puncture was performed with an opening pressure of 21.6 cm of H20. The cerebral spinal fluid ( CSF) revealed a lymphocytosis ( white blood cells, 58/ mm3 with 99% lymphocytes) and elevated protein at 50 mg/ dL. A subsequent magnetic resonance venogram ( MRV) performed at 6 weeks showed no dural sinus thrombosis. Extensive laboratory evaluation for infectious etiologies, collagen vascular disease, and occult malignancy was unremarkable. Syphilis serology, human immunodeficiency virus ( HIV), acute and convalescent antibody titers in the serum and CSF, and polymerase chain reaction of the CSF revealed no detection of herpes virus infection. Bacterial and viral cultures of the throat, CSF, blood and genital lesions were negative. Interferon- alpha 2a ( 9 million units administered sub-cutaneously three times per week for 5 weeks; total dose approximately 135 million units) and colchicine ( 1.2 mg/ day) were initiated with retinitis, and retinal vasculitis resolved at 2 weeks. Neurologic manifestations markedly improved as the temporal lobe lesion improved ( evidenced by MRI scan), and disc edema nearly resolved at the 6- week follow- up. A repeat MRI scan of the brain and ocular examination at approximately 3 months showed resolution of the temporal lobe lesion ( Fig. 3), disc edema, intraocular inflammation and systemic manifestations. The patient remains without systemic, ocular, and neurologic manifestations through the 8- month follow- up period, maintained only on colchicine ( 1.2 mg/ day). Comment Current immunosuppressive therapy of ocular and neurologic manifestations of Behcet disease may lack efficacy ( 1), cause neurotoxicity, or accelerate the development of central nervous system ( CNS) manifestations 109 110 J. C. NICHOLS ET AL. FIG. 1. A: Right and B: left optic nerve photographs demonstrate optic disc edema. ( 2,3). These signs and symptoms resemble those of patients with neuro- Behcet disease. Alternative therapeutic agents are thus necessary to manage this leading cause of mortality and morbidity in Behcet disease. Interferon has antiviral, immunomodulatory, antiproliferative, and antitumoral properties. Interferon- alpha 2 treatment of Behcet disease in the absence of ocular or neurologic symptoms has been described ( 4). Recently prophylaxis ( 5) and treatment ( 6) of the ocular manifestations of Behcet disease have been reported with interferon- alpha 2. This report describes resolution of ocular, systemic, and neurologic manifestations of Behcet FIG. 2. Fluid Attenuated Inversion Recovery ( FLAIR) image of the brain demonstrates right temporal lobe lesion. FIG. 3. Fluid Attenuated Inversion Recovery ( FLAIR) image of the brain at 3 months after treatment reveals resolution of the right temporal lobe lesion and atrophy of the body and tail of the right hippocampus. / Neuro- Ophthalmol, Vol. 21, No. 2, 2001 INTERFERON- ALPHA 2a TREATMENT OF NEURO- BEHCET DISEASE 111 disease concurrent with interferon- alpha 2 treatment. The efficacy of interferon in the management of Behcet disease may occur through resolution of pathologic cytoki-nemia and endothelial disturbance found in this disease. Neurologic involvement in Behcet disease is present in 5.3 to 25% of patients, depending on the geographic region studied ( 7). Clinical patterns of neuro- Behcet disease include parenchymal and nonparenchymal CNS involvement ( 8). Secondary or nonparenchymal CNS patterns include aseptic meningitis and bilateral disc edema without intracranial hypertension ( 8), as found in our patient. The presence of bilateral disc edema without dural sinus thrombosis by MRV at 6 weeks and MRI scrutinized at diagnosis emphasizes that nonparenchymal neuro- Behcet may occur in the absence of vascular involvement. A focal inflammatory lesion within the temporal lobe is atypical for parenchymal lesions in neuro- Behcet disease. Parenchymal lesions are more commonly found in the midbrain and brain stem ( 7). The occurrence of both patterns of CNS involvement in this patient in the absence of dural sinus thrombosis supports a similar pathogenic mechanism for each. Criteria ( 9,10) establish the diagnosis of Behcet disease in this case because other diseases were excluded by diagnostic testing. Polymerase chain reaction and antibody testing for herpes viruses in the CSF and serum exclude herpetic meningoencephalitis as an alternative diagnosis. The resolution of ocular, systemic, and CNS manifestations concurrent with interferon- alpha 2a therapy is suggestive of a causative effect of treatment, and spontaneous improvement was unlikely given the typically progressive nature of neuro- Behcet disease without therapy. Controlled randomized studies are warranted to demonstrate efficacy of interferon- alpha 2 treatment of ocular and neurologic manifestations of Behcet disease. REFERENCES 1. Saenz A, Ausejo M, Shea B, et al. Pharmacotherapy for Behcet's syndrome. Cochrane Database Syst Rev 2000; 2: CD001084. 2. Kotake S, Higashi K, Yoshikawa K, et al. Central nervous system symptoms in patients with Behcet's disease receiving cyclosporine therapy. Ophthalmology 1999; 106: 586- 9. 3. Igarashi T, Ishigatsubo Y, Ohno S, et al. Central nervous system toxicity related to FK506 in patients with Behcet's disease. Ann Rheum Dis 1994; 53: 350- 1. 4. O'Duffy JD, Calamia K, Cohen S, et al. Interferon- alpha treatment of Behcet's disease. J Rheumatol 1998; 25: 1938^ t4. 5. Demiroglu H, Ozcebe OI, Barista I, et al. Therapy with interferon-alpha 2b demonstrates prophylaxis of recurrent eye attacks in Behcet's disease: a randomized trial of interferon alpha 2b, colchicine, and benzathine penicillin versus colchicine and benzathine penicillin. Lancet 2000; 355: 605- 9. 6. Kotter I, Eckstein AK, Stubiger N, et al. Treatment of ocular symptoms of Behcet's disease with interferon alpha 2a: a pilot study. Br J Ophthalmol 1998; 82: 488- 94. 7. Serdaroglu P. Behcet's disease and the nervous system. J Neurol 1998; 245: 197- 205. 8. Akman- Demir G, Serdaroglu P, Tasci B, et al. Clinical patterns of neurological involvement in Behcet's disease: evaluation of 200 patients. Brain 1999; 122: 2171- 81. 9. Yamamoto S, Toyokawa H, Matsubara J. A nationwide survey of Behcet's disease in Japan: 1. Epidemiological survey. Jpn J Ophthalmol 1974; 18: 282- 90. 10. International Study Group for Behcet's Disease. Criteria for diagnosis of Behcet's disease. Lancet 1990; 335: 1078- 80. J Neuro- Ophthalmol, Vol. 21, No. 2, 2001 |